Nowhere to Turn
Investigation into the Ministry of Community and Social Services’ response to situations of crisis involving adults with developmental disabilities.

Table of contents
Show
Hide
Investigation into the Ministry of Community and Social Services’ response to situations of crisis involving adults with developmental disabilities
"Nowhere to Turn"
Paul Dubé
Ontario Ombudsman
August 2016
Office of the Ombudsman of Ontario
We are
An independent offce of the Legislature that resolves and investigates public complaints about Ontario public sector bodies. These include provincial government ministries, agencies, boards, commissions, corporations and tribunals, as well as municipalities, universities, school boards, child protection services and French language services.
Our Values
Fair treatment
Accountable administration
Independence, impartiality
Results: Achieving real change
Our Mission
We strive to be an agent of positive change by promoting fairness, accountability and transparency in the public sector and promoting respect for French language service rights as well as the rights of children and youth.
Our Vision
A public sector that serves citizens in a way that is fair, accountable, transparent and respectful of their rights.
Contributors
Systemic Investigation
Director, Special Ombudsman Response Team
- Gareth Jones
Lead Investigator
- William Cutbush
Investigators
- Claran Buggle
- Grace Chau
- Rosie Dear
- Ronan O'Leary
- Adam Orfanakos
- Domonie Pierre
- Elizabeth Weston
General Counsel
- Laura Pettigrew
Individual Cases
Director, Investigations
- Sue Haslam
Investigators
- Anne Hart
- Jackie Esler
- Chris McCague
- Leanne Salel
Early Resolution Officers
- Sharon Anderson
- Heather Conklin
- Anna Gatova
- Alanna Maloney
- Andrea Marlow
- Dahlia Phillips
- Alexandra Saginur
General Counsel
- Wendy Ray
Press conference:
Minister accepts all 60 recommendations:
Executive summary
1 It is now recognized that the model of institutional care for individuals with developmental disabilities, which prevailed in this province for over a century, was a failure. The Premier, on December 9, 2013, apologized[1] for the suffering it caused, and Ontario has moved on to embrace a community-based approach for the developmental services sector, promoting social inclusion, individual choice and independence. This is a positive evolutionary policy shift. Unfortunately, despite the government’s recent efforts, there remain individuals on the margins, living with profound and complex disabilities and faced with extreme circumstances. When they reach a crisis point, service gaps often leave them and their families without any real choice, and dependent on a system unresponsive to their needs. Without significant additional reform, many uniquely vulnerable people will continue to be lost in the system and experience harm because of inadequate supports and services.
2 During the course of this investigation our Office received more than 1,436 complaints about the state of Ontario’s developmental services system and we continue to do so. Our investigation focused on how the Ministry of Community and Social Services responds to situations of crisis and administers the process for co-ordinating, monitoring, and facilitating urgent access to resources for adults with developmental disabilities. What we found was a fragmented, confusing, and complex assortment of hundreds of community agencies and local processes, impossible for many individuals with developmental disabilities and their families to navigate. The process for accessing supports and services in the developmental services sector is multi-layered, and inconsistent across the province. Families were often bewildered by the confusing web of service providers or oblivious to the distinctions between the various service agencies, Developmental Services Ontario offices and Ministry officials. Many were discouraged by interminable waitlist delays and desperate for help. Some were on the brink of crisis, others firmly in its midst.
3 The present demand for services far outstrips the supply, leaving thousands stranded on waiting lists. While steps have been taken to create more uniformity and standardization for accessing urgent resources, there is still marked inconsistency in how limited funds are prioritized and distributed.
4 We also discovered that without adequate safeguards, early warning systems, and effective monitoring of agency reporting obligations, in some cases adults with developmental disabilities are placed in jeopardy of domestic abuse. Insufficient crisis beds and supports can result in individuals remaining in unstable and unsafe homes or shuttled off to homeless shelters, where their vulnerability continues to place them at risk. For example, it took two years for one survivor of neglect, Adam[2], to secure steady funding and a residential placement. Then there was Layla, who was shunted between 20 temporary locations in 34 days, including a series of shelters, as she desperately but unsuccessfully attempted to escape an abusive home situation.
5 Despite the Ministry’s efforts and intent to transform the system away from the former institutional model, in reality some adults with developmental disabilities, particularly those who live with complex conditions or serious behavioural challenges continue to find themselves excluded from their communities. Institutional care no longer happens through design but by default. There are far too few community placements with the ability to accommodate the needs of individuals labelled as hard to serve. With nowhere else to turn, those in crisis can find themselves inappropriately housed in a variety of institutional settings from hospitals to jails.
6 Ontario’s general hospitals and psychiatric units have become hosts to hundreds of adults with developmental disabilities – many with multiple diagnoses – at significant cost to the health system. Some spend years hospitalized, for reasons unrelated to health care, while waiting for homes in the developmental services sector. Most hospitals typically lack the specialty training and programming necessary to serve those with developmental disabilities. Unnecessary hospitalization also increases the risk of infection and psychological harm. While in hospital, adults with developmental disabilities all too often find themselves sedated, under guard, and isolated on locked wards. For instance, Peter, who is diagnosed with autism spectrum disorder and functions cognitively at the level of an 18-month-old child, spent the better part of 12 years languishing on psychiatric units. When he lashed out due to under-stimulation, he would inevitably end up in physical restraints. The Ministry has recently made some attempts at inter-ministerial co-ordination and collaboration to solve the problem of unnecessary hospitalization. However, it must take on a more active and lead role to reverse this disturbing trend.
7 Long-term care homes have also become providers of institutional care to adults with developmental disabilities, despite the fact that such settings can be wholly unsuitable. Some, such as Patrick, who has cerebral palsy and entered a nursing home at the age of 24, are decades younger and considerably more active than the elderly residents who typically occupy these homes. Patrick initially rebelled against this inapt environment and, in one fit of frustration, accidentally broke the ankle of a frail senior. His wheelchair was confiscated, leaving him to crawl on the floor for four months. His lack of mobility and verbal communication skills also left him vulnerable to repeated sexual abuse by an elderly roommate. The Ministry has failed individuals like Patrick. It needs to take steps to ensure adults with developmental disabilities, whose interests are best served in community placements, do not find themselves consigned to live out their lives in long-term care homes and hospitals.
8 Unfortunately, incarceration of adults with developmental disabilities has also become a failsafe alternative to secure and supportive housing in the community. Individuals with developmental disabilities, particularly those who also live with psychiatric illness, are in jeopardy of being charged criminally when they act impulsively and aggressively. For example, at 55, Joe lives with developmental and psychiatric disabilities and functions at the cognitive level of a six-year-old. He has been jailed repeatedly for offences including theft and assault. While in the correctional system, Joe’s disruptive, combative, bizarre and suicidal behaviours typically earn him a stay in solitary confinement, isolated in a segregation cell. Then there is 25-year-old Andrew, a brain cancer survivor who lives with cognitive and developmental disabilities. He is a former Crown ward whose risky behaviour, including making false abuse claims, has rendered him a pariah in the developmental services system. Without satisfactory community supports, he has spent considerable time locked up in jail. Although court diversion programs exist, they are not tailored to the needs of persons with developmental challenges. The Ministry must work more effectively with the justice and correctional systems to minimize the risks of unwarranted criminalization and incarceration of vulnerable individuals. It must also take decisive steps to build capacity in the community to protect adults with developmental disabilities from such consequences.
9 Our investigation also revealed that there are adults with both developmental disabilities and complex medical conditions who are unable to access necessary community supports and services. For instance, 20-year-old Stella has a brain stem dysfunction and is non-verbal, incontinent and unable to move her limbs. She uses a wheelchair, is dependent on tubes for feeding and breathing, and requires constant supervision and suctioning to prevent sudden death. With no compatible local placements available, Stella’s family spent years on the verge of collapse. Similarly, 25-year-old Steven is medically fragile and completely dependent on others for all aspects of his care. His exhausted family continues to wait anxiously for resources to satisfy his urgent needs. The Ministry must do more to co-ordinate and plan care across ministries and communities to avert crises in such medically complex cases.
10 During our investigation, we heard from hundreds of beleaguered families at the breaking point. Many caregivers suffer from serious medical conditions arising from chronic physical and mental strain, and/or are elderly and terrified about what will become of their loved ones when they are no longer able to care for them. We also received multiple complaints about families held hostage in the home, victims of violence at the hands of loved ones who urgently require more intensive services and supports. Transition to adulthood is particularly stressful for individuals with developmental disabilities. No longer eligible for educational and children’s sector services, they often experience negative behavioral changes. Frequently, their families descend into crisis without stable, dependable, and consistent supports.
11 Caregiver exhaustion, illness, aging and death have also predictably led to cases of abandonment and homelessness. For instance, despondent parents relinquished care of their 19-year-old son, Serge, who has multiple diagnoses and functions at the cognitive level of a two-year-old, when escalating emergencies led them to conclude they could no longer safely support him at home. In the case of 41-year-old Cindy, who has a dual diagnosis and cognitive capacity of a young child, she waited seven years on a waitlist for a community placement, only to find herself on the brink of homelessness after her mother’s death. An aging aunt and uncle stepped in to provide temporary care. However, after Cindy’s uncle died, her grieving aunt could no longer cope and eventually gave up trying, leaving Cindy with temporary respite providers. The Ministry needs to engage in rigorous monitoring and supportive intervention to help break the cycle of abandonment and homelessness that plagues the developmental services sector.
12 Since our Office began this investigation in November 2012, the government committed in its April 2014 budget to invest an additional $810 million over three years to strengthen services and supports in the developmental services sector bringing current spending in the sector to $2 billion annually. The Ministry has also taken steps to improve how it responds to situations of crisis and administers the process for urgent access to services. However, progress has been incremental. Much more needs to be done to bridge the significant service gaps.
13 In my opinion, the Ministry’s response to urgent situations involving adults with developmental disabilities and its administration of the process to address crisis cases has been unreasonable and wrong. I have made 60 recommendations for reform, including a requirement that the Ministry report back on its progress in implementing necessary changes.
14 The Ministry has acknowledged that despite its efforts to transform the developmental services system to support personal choice, independence, and inclusion, some unacceptable situations identified in my report continue. In responding to my findings, it has fully committed to working with our office, individuals, families, and the developmental services sector to improve outcomes for adults with developmental disabilities. The Minister has personally agreed to all of my recommendations and the Ministry has provided a detailed response on how they will be implemented. I am encouraged by these developments and acknowledge the progress that has already been made in recent years to improve the developmental services system. I believe that the Ministry is well intentioned and earnest, but recognize that systemic flaws persist. I intend to closely monitor the Ministry’s success in meeting existing system challenges.
15 It is often said that societies are judged on how they treat the most vulnerable of their members. The time has come to move beyond apologies and work towards a consistent, co-ordinated, collaborative, and responsive developmental services system, able to effectively and humanely meet the needs of individuals and families in crisis.
Investigative Process
16 In 2012, the Ministry of Community and Social Services estimated that there were 62,000 adults in Ontario with developmental disabilities.[3] Within this group up to 40% are likely to have a concurrent mental health diagnosis – known as “dual diagnosis.”[4] For many years, our Office has received complaints about the Ministry’s response to situations of urgency and crisis involving adults with developmental disabilities and dual diagnosis. We have addressed individual concerns and met regularly with senior Ministry officials to discuss complaint trends. Despite these efforts, complaints about developmental services continued to rise, from 35 in 2010, to 45 in 2011, to 64 by mid-fall 2012.
17 Given the steady increase in complaints, the Special Ombudsman Response Team (SORT) conducted a preliminary assessment. Our Office notified the Ministry on November 28, 2012, and publicly announced the next day, that a systemic investigation would be conducted into how it responds to situations of urgency or crisis involving adults with developmental disabilities, and how it administers the process for co-ordinating, monitoring, and facilitating access to services for adults with developmental disabilities in situations of crisis.
18 Eight investigators, under the direction of the Director of SORT and assisted by general counsel, carried out the investigation, supported by a dedicated team of four investigators and seven Early Resolution Officers, who worked to resolve compelling individual complaints parallel to the systemic investigation. To date, we have addressed 1,436 individual cases since the launch of the investigation. The Director of Investigations and general counsel also met regularly with senior Ministry officials to identify trends and discuss egregious cases. The arrival of a new Assistant Deputy Minister for the Community and Developmental Services Division in the fall of 2013 signalled a positive change in the Ministry’s approach to crisis cases in the developmental services sector. Since that time, our Office has been able to facilitate resolution of many complex and urgent cases working in collaboration with Ministry officials. However, underlying systemic problems persist.
19 We conducted 221 interviews, including with assistant deputy ministers, regional directors, community program managers, senior program advisors, and senior policy analysts from the Ministry’s regional and corporate offices, and Developmental Services Ontario officials. We also spoke with stakeholders, including transfer payment service agencies, unions, hospitals, Local Health Integration Networks, police, and groups such as Community Living Ontario, Autism Ontario, the Centre for Addiction and Mental Health, and the Ontario Independent Facilitation Network.
20 The team also researched how other jurisdictions approached issues relating to services for adults with developmental disabilities in crisis. We found that while systems vary, other jurisdictions face similar challenges in meeting the needs of these individuals.
21 SORT investigators visited six of the original nine regions established by the Ministry for the provision of developmental services (there are now five). The selection of regions to visit was based on complaint volume, either high or low, as well as geographic location.
22 In total, 1,436 families, individuals and stakeholders contacted our Office to comment about adult developmental services and to share their stories and concerns with us. Some 191 complaints related to individuals living with dual diagnosis.
23 We obtained and reviewed more than 24,000 documents from the Ministry, including files relating to specific urgent situations. We requested additional documents and updates throughout the investigation, amounting to nearly 1,600 more documents. We also received and reviewed a number of submissions from stakeholders and complainants. The Ministry co-operated fully with our investigation.
24 Although staff worked tirelessly to address individual cases and raise systemic trends with senior Ministry management during our investigation, it was uniquely challenging. It was conducted against a backdrop of evolving developmental services policy and funding initiatives, and involved a system that proved multi-faceted and complex. The systemic investigation was extensive, and as it progressed, our efforts served as a catalyst for many positive improvements. Our interviews and discussions with senior Ministry officials helped propel the creation of a standardized urgent response process to facilitate more consistent and effective resolution of crisis cases. Our attempts to raise awareness for distressed individuals lost in the system led to a greater willingness on the part of Ministry officials to intervene to provide help. One of the most significant changes we witnessed was an increased focus on the part of the Ministry on finding residential supports for individuals with complex needs. During the investigation, the Ministry helped 20 individuals who had been unnecessarily institutionalized in hospitals secure homes in their communities. These and other reforms are reviewed in this report.
Investigation scope
25 The social services system is vast and involves multiple ministries and programs affecting tens of thousands of individuals with a diverse range of developmental disabilities, cognitive abilities, and capacity for making personal choices and living independently. In planning for this investigation, many serious issues of concern were raised by stakeholders. However, given our limited resources, and the compelling and urgent nature of crisis situations that we identified, we focused our attention on those adults most in need. For these individuals, a chronic lack of supports and services has deprived them and their families of practical options or any realistic chance for self-determination.
26 Significant concerns remain about such matters as inadequate services for high-functioning individuals with Autism Spectrum Disorder, who require assistance but do not qualify for developmental services, and the general lack of day and employment programs. The sufficiency of staff training and retention in the developmental services sector was also identified as a chronic problem. We continue to monitor these issues and work with the Ministry to address trends in complaints. However, the focus of this investigation was on services and programs for those with complex needs in urgent situations. Many of these vulnerable individuals found themselves living in untenable circumstances as a result of system failure. Their stories were profoundly compelling and clearly highlighted a need for systemic change.
Other reviews and related investigations
27 As part of our investigation, we monitored parallel inquiries, audits and recommendations addressing various aspects of the developmental services sector. These reviews were instructive and provided significant insights complementing our own investigative findings relating to adults with developmental disabilities in crisis.
Select Committee on Developmental Services
28 A Select Committee on Developmental Services was established by the Ontario Legislative Assembly on October 3, 2013, to address the educational, workplace, social, housing and other support needs of children, youth, and adults with developmental disabilities or dual diagnosis across the province. The Select Committee heard from more than 140 presenters at 14 public hearings, and received more than 300 submissions.
29 In July 2014, the committee issued its final report, Inclusion and Opportunity: A New Path for Developmental Services of Ontario, with 46 recommendations for reform. In its report, the committee stated:
Above all, the Committee heard repeatedly that individuals and families who need developmental services and supports are in crisis. We heard that after struggling to obtain services and enduring waitlists for years, many families feel pushed to the brink of disaster. Only when they are forced into crisis are they able to access desperately needed assistance. When that happens, others are bumped further down the waitlists.[5]
30 The Select Committee’s key recommendations relating to adults with developmental disabilities included eliminating the waitlists for services and supports; creating a 10-ministry inter-ministerial committee tasked with eliminating all waitlists in 12 months; better data collection and co-ordination; ensuring continuity of funding from the children’s to the adult system; improved services and co-ordination for individuals with complex needs, particularly those living in remote communities; improved health, dental care and education; creative housing solutions; and expansion of respite and day programming.
31 The Minister of Community and Social Services responded to the committee on October 28, 2014, indicating that most of its recommendations would be implemented. Although recommendations to transform developmental services and supports into mandatory entitlements and to eliminate all waitlists were rejected, the government’s 2014-2015 budget dedicated $810 million over three years to strengthen and increase the range of government-funded developmental services and supports.[6]
Auditor General
32 In 2014, Ontario’s Auditor General reported on the results of an audit conducted into whether the Ministry of Community and Social Services has effective mechanisms to meet the residential needs of individuals with developmental disabilities in a cost-effective manner, and to monitor service providers’ compliance with regulations, policies and contractual obligations.[7]
33 Many of the Auditor General’s findings parallel our observations relating to inconsistency of access to – and lengthy waitlists for – residential placements in the community. The Auditor General made 11 recommendations to the Ministry, including that it develop a consistent prioritization process and improve the management of wait times for residential services.
34 In response to the Auditor General’s recommendations, the Ministry indicated that it was building on the work of existing community prioritization processes to promote greater consistency and fairness in the introduction of provincially consistent prioritization.
Inquests
Guy Mitchell
35 Guy Mitchell was 38 years old when he drowned in a cistern in Ancaster on April 29, 2012. He had been living with a family in a host family placement, along with another man with developmental disabilities and an 11-year-old girl with autism. A coroner’s inquest was held in July 2015 to examine the events surrounding his death. The inquest resulted in 16 recommendations, released on July 24, 2015, which were addressed to multiple ministries and focused on improving the circumstances and monitoring relating to placements of adults with developmental disabilities in host family homes. The Ministry of Community and Social Services implemented new Host Family Program policy directives in April 2016, including rules on screening criteria for host families and enhanced monitoring requirements. It has also established one new working group and is using two existing working groups to address the inquest recommendations, including two inter-ministerial and stakeholder groups, one focused on protecting vulnerable individuals and the other directed at advising on improvements to the host family program. In addition, the Ministry is using an existing working group of ministerial and stakeholder representatives to discuss quality assurance measures applying to service agencies.
James (Jamie) Hawley
36 Jamie Hawley died at the age of 41 on May 26, 2008, from a combination of pneumonia, starvation, and infected bedsores. Jamie was non-verbal with a mental age around seven. He also lived with several physical disabilities, including partial paralysis, requiring him to use a wheelchair. Jamie’s condition steadily declined after his brother removed him from a community placement and took over his care in 2000. While Jamie’s circumstances were raised with several authorities, the Developmental Services Sector lost track of him, as a result of frequent moves. By the time he died, Jamie was suffering the consequences of chronic neglect and weighed only 57 pounds. After Jamie’s death, his brother was convicted of manslaughter and sentenced to 20 years in jail. A coroner’s inquest was held in December 2015, and 17 recommendations were issued in February 2016, addressed at preventing similar tragedies.[8] The jury’s recommendations included a call for proper discharge planning and monitoring by service agencies, screening of caregivers, increased information sharing amongst service providers and public officials, and an effective system for reporting risks of harm to vulnerable individuals.
Lessons from the Past
37 In the 1800s, from a medical and social standpoint, there was little distinction in the treatment of those with intellectual and mental health conditions. In the early part of the century, adults with mental and developmental disabilities who could not be cared for in their family homes often found themselves housed in jails.[9] In 1839, the Ontario government passed An Act to Authorise the Erection of an Asylum within this Province for the Reception of Insane and Lunatic Persons. In 1841, Ontario opened its first “asylum” under this Act, initially located at the Old York Jail in Toronto, and eventually moved to 999 Queen Street.[10]
38 In 1876, the first large-scale segregated asylum for individuals with developmental disabilities was established in a rural setting in Orillia (later known as the Huronia Regional Centre).[11] Over the next century, the demand for residential services increased exponentially and additional institutions were founded across the province. These facilities were administered on a medical model through the Department of Health, (now the Ministry of Health and Long-Term Care). By the 1970s, there were 16 institutions in Ontario, serving more than 10,000 individuals with developmental disabilities.[12]
39 In the 1950s and 1960s, public concern emerged over the overcrowded and deteriorated conditions in Ontario’s residential institutions. The “community living” movement was also spreading across North America, promoting participation by those with developmental disabilities in the community rather than in isolated institutional environments.
40 In 1955, the Ontario government passed the Rehabilitation Services Act, which provided for a full range of services for individuals with physical and developmental disabilities. Various community-based programs run by private agencies and family members emerged, funded by the Department of Public Welfare (now the Ministry of Community and Social Services).
41 With the advent of Ontario’s Human Rights Code in 1962 and the UN Declaration of the Rights of Persons with Intellectual Disabilities in 1971, came greater recognition of the rights of individuals with developmental disabilities. By the 1970s, increased emphasis was placed on improving the programs and services available to institutional residents. In addition, there was growing support from within the evolving disability rights movement and academia for replacement of institutional care with community supports.[13]
42 In 1974, Ontario brought in the Developmental Services Act, which established a framework for the creation, funding, and operation of community services for people with intellectual disabilities. Responsibility for operation of Ontario’s institutions also shifted from the Ministry of Health to the Ministry of Community and Social Services. In addition, Ontario established an Adult Protective Services Worker program, to provide client advocacy, case management and counselling services for individuals with developmental disabilities living in the community.[14] Workshop programs also began to appear in community-based settings.
43 The transition from a medical and institutional services model to community-based programing for individuals with developmental disabilities gained momentum in 1977, when the Ontario government launched its first multi-year plan to increase community supports and decrease reliance on institutional care.[15] By 1982, five provincial institutions had closed. In 1987, the Ministry of Community and Social Services announced that within 25 years, it planned to shutter all of the remaining residential facilities.
44 As the Ministry moved forward with its deinstitutionalization plans, it increased financial supports for those living within the community. In 1990, the Special Services at Home program, which provided supports to help children with physical or developmental disabilities live at home with their families, was expanded to include adults with developmental disabilities.[16]
45 In 1996, the Ministry of Community and Social Services launched its “Community Living Initiative,” resulting in some 1,000 individuals moving into the community, and by 2000, three more institutions had closed. In 2004, six more institutions were decommissioned, and the remaining facilities were no longer admitting residents. That was also the year the government commenced an initiative to transform the adult developmental services sector to streamline service delivery and provide more equitable access across the province.
46 In 2008, the province introduced a new model for provision of supports and services in the developmental services sector. On March 31, 2009, the last institution for the care of individuals with developmental disabilities closed its doors.
Institutional legacy
47 Ontario’s institutional system for individuals with developmental disabilities has left a bitter legacy. In recent years, there have been a series of revelations about dehumanizing abuse suffered by former residents. Several class action lawsuits were filed and settled on their behalf.[17] In the case of the oldest institution, the Huronia Regional Centre, as part of a $35-million settlement, in December 2013, the Premier offered a formal apology in the Legislative Assembly:
Mr. Speaker, we take responsibility for the suffering of these people and their families… I offer an apology to the men, women and children of Ontario who were failed by a model of institutional care for people with developmental disabilities. We must look in the eyes of those who have been affected, and those they leave behind, and say: We are sorry.[18]
48 While the Ministry has made progress over the course of the last few years, significant additional improvements are required to meet the needs of those in crisis.
Overview of Legislation
49 Today, the Services and Supports to Promote the Social Inclusion of Persons with Developmental Disabilities Act, 2008, administered by the Minister of Community and Social Services, governs the provision of services and supports for adults with developmental disabilities. Passed on October 8, 2008, the Act has been proclaimed into force in stages and is not yet fully operational.
50 The Act was intended to modernize developmental services in Ontario and replace the outdated, 35-year-old Developmental Services Act. It supports provision of more independence and choice for individuals with developmental disabilities, transition towards a community-based living model, and greater social inclusion. It is also intended to ensure increased fairness and uniformity in terms of eligibility, assessment and access to services and to simplify the process for accessing supports, services, and funding.
51 The Act includes a definition of developmental disability, which covers someone who has:
…the prescribed significant limitations in cognitive functioning and adaptive functioning and those limitations:
- Originated before the person reached 18 years of age
- Are likely to be lifelong in nature; and
- Affect areas of major life activity, such as personal care, language skills, learning abilities, the capacity to live independently as an adult or any other prescribed activity. (s.3)
52 The terms “adaptive functioning” and “cognitive functioning” are further defined in subsection 3(2).
53 One of the Act’s key concepts is the creation of application entities. These entities act as a single point of access for services and supports within various geographic regions in Ontario (s.8(5)). They are also responsible for assessing whether individuals are eligible for developmental services. The application entities, known as Developmental Services Ontario offices, opened their doors for business on July 4, 2011. These offices are private, non-profit organizations, which are required to comply with regulated quality assurance measures and reporting requirements.
54 The Act also contemplates the establishment of funding entities, responsible for prioritizing the provision of services, supports, and funding and managing waitlists. The relevant provisions of the Act relating to these entities have not yet come into force. There is no anticipated date for them to take effect. In the absence of the funding entities, the Ministry has continued to provide funding directly to service providers, which handle prioritization and waitlist management.
55 Under the Act, service agencies is the term used to refer to the variety of organizations in the community that provide services and supports under funding agreements with the Ministry of Community and Social Services (s.1). Service agencies, which receive transfer payments from the Ministry, must comply with regulatory requirements, including quality assurance and reporting measures, funding agreements, and policy directives establishing performance standards and measures. They must also have written complaint-handling policies (ss. 22-26).
56 The Act contemplates six areas of services and supports:
- Residential services and supports;
- Activities of daily living services and supports;
- Community participation services and supports;
- Caregiver respite services and supports;
- Professional and specialized services; and
- Person-directed planning services and supports (s.4).
57 Under the Act, the Ministry can provide funding to service agencies under agreements (s.10). Unproclaimed sections of the Act would also allow the Ministry to provide funds to Developmental Services Ontario offices so that they may enter into direct funding agreements with individuals seeking services. (s.11) The Ministry has indicated that the direct funding option would improve choice by allowing people to tailor supports to their needs.
System Overview
58 Currently, the adult developmental services system is rather daunting and complex. While the Ministry of Community and Social Services provides funding, individual service agencies decide on the type and nature of the supports and services they will offer. In this sense, the phrase “developmental services system” is a bit of a misnomer. As one former senior Ministry official explained to us, unlike other social service areas, residential and other support programs for adults with developmental disabilities evolved through the grassroots efforts of parent groups and advocates in response to concerns with provincially-run institutional care. Community supports and services grew organically and in an ad hoc manner over an extended period. Consequently, access to and availability of services and supports differs across the province. Today’s developmental services system does not reflect long-range strategic planning on the part of the Ministry, but rather a matrix of diverse and individualized visions of hundreds of non-governmental agencies involved in this sector.
The Ministry of Community and Social Services
59 The Ministry is responsible for development of policy and administration of programs relating to developmental services. The Ministry does not administer or provide services directly, but manages the developmental services system through its regional offices. At the outset of our investigation, there were nine regional offices with more than 60 staff members associated with developmental services. In fiscal year 2013-2014, the Ministry reorganized and reduced its regions to five, while retaining the same staffing level.[19]
60 The regional offices administer various developmental services programs through contractual arrangements with service agencies. Regional offices are headed by regional directors, who report to the Assistant Deputy Minister for the Community and Developmental Services Division, who in turn reports to the Deputy Minister. Regional offices have responsibilities in other program areas. There are about 40 regional program supervisors, who are primarily responsible for working directly with agencies delivering adult developmental services.
Service agencies
61 The Ministry’s regional offices contract with non-profit community service agencies to deliver supports and services. The Ministry transfers base funding annually to some 370 transfer payment agencies throughout the province. Most agencies provide direct services and supports to individuals with developmental disabilities for such things as residential care, assistance with daily living, help with community participation, and providing caregiver respite. Some provide specialized services such as behaviour management and treatment.
62 One of the services that some service agencies provide is case management to individuals with developmental disabilities. Case managers meet with individuals and their families regularly and help plan for and co-ordinate services. They can also help them apply for funding, attend medical appointments with clients, connect with programs and services, and sometimes assist with tasks of daily living.
Community planning tables
63 Every region has several community-based or local planning tables, which are chaired by local service agencies. These bodies are involved in addressing individual and systemic issues relating to services in their geographic areas. They have many roles and functions, and in larger geographic areas, often have specialized subcommittees. Planning tables are typically responsible for regional or area system planning, prioritization of those found eligible for developmental services, and finding temporary solutions for individuals in crisis.
Developmental Services Ontario
64 Nine not-for-profit community agencies operate as Developmental Services Ontario offices. They work in association with the Ministry’s regional offices. Developmental Services Ontario offices are the central access point for all developmental services and supports funded by the Ministry. They are responsible for:
- Informing the public about what services are available in their communities;
- Managing the application process, including confirming eligibility;
- Initiating the local process for resolving service issues; and
- Matching persons with developmental disabilities to available Ministry-funded adult developmental services and supports.
Funding for developmental services and supports
65 Decades ago, when developmental services were considered part of the health care system, institutional services were fully funded as an entitlement program, similar to other universal health care services. When the program responsibility transferred to the Ministry of Community and Social Services, the nature of the funding changed. Spending on developmental services is currently considered discretionary and restricted to set funding envelopes. In addition to funding service agencies, the Ministry provides funding to individuals through various programs. The total budget for developmental services in fiscal year 2012-2013 was $1.69 billion. An additional $42.5 million was budgeted the next fiscal year. Based on the government’s budget announcement in April 2014, adding an additional $810 million in funding over the next three years, funding in this sector reached $2 billion in 2016-2017.
66 Until 2014, the Ministry did not have comprehensive information about individuals receiving developmental services. Rather, service agencies kept their own records. In December 2014, after analyzing results from a survey of service agencies, the Ministry determined there were 33,615 adults receiving Ministry-funded developmental services. Of those, 29% were classified as dual diagnosis.
Developmental Services System Overview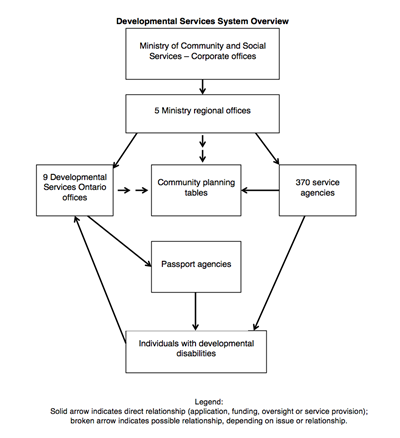
Special Services at Home
67 Today, several government programs are available to families of children with severe disabilities, including the Special Services at Home program. This program helps families of children with developmental or physical disabilities pay for special services in or outside the family home. As of April 1, 2012, eligibility for the program is limited to children under 18 years of age. A set envelope of funding is allocated and distributed under this program annually. Accordingly, even someone who was found eligible for the program might have waited for a significant period before receiving funding. Some aged out of the children’s system without ever receiving funds from this program. In March 2015, the Ministry announced that the 2014 waitlist for the program had been eliminated, as a result of increased funding introduced through the 2014 budget.
Ontario Disability Support Program
68 The Ministry’s Ontario Disability Support Program provides assistance with essential living expenses, including shelter, food, and drug and vision care, as well as employment supports to individuals living with substantial physical and mental impairments. To qualify, an individual must be at least 18 years old, an Ontario resident, and otherwise meet the program’s disability and financial threshold requirements. This program is an entitlement program. This means that funding is provided to all those who qualify for support. A single individual receiving benefits under this program may receive up to $1,110 a month for basic needs and shelter, depending on living circumstances, and may be eligible for other benefits.[20]
Passport program
69 In the adult developmental services sector, the Ministry’s primary program for direct funding of supports and services is the Passport program. Passport funds are used for a range of services and supports to enable adults with developmental disabilities to take part in community classes or recreational programs, develop work, volunteer, and daily life skills, hire a support worker, create a life plan and access temporary respite for their caregivers. Developmental Services Ontario offices manage the application process for Passport. They refer application packages for qualified applicants to the regional “Passport agency” to assess the appropriate funding level. The maximum annual funding available is $35,000. Passport prioritization is divided into high, medium, and low priority, based on several factors including medical and behavioural issues, other available supports, and the length of time the individual has been waiting for funding. Subjective considerations are also included, such as the ability of the individual’s family to cope. In 2014, the Ministry introduced a prioritization tool that assists in allocating funds for the Passport program.
70 Individuals who receive Passport funding for community participation or caregiver respite can choose to receive their funding directly and purchase services themselves, or use the existing service agency system. Recipients can use up to 10% of their total approved funding to cover an administration fee, if they use a service agency to administer their Passport funding.
71 Like Special Services at Home, Passport funding is limited by a specific annual budget. Once the funds for any given year are distributed, other eligible applicants are placed on a waitlist in their region unless and until additional funds are allocated mid-year. In 2011, when the Developmental Services Ontario offices were established, there were hundreds of eligible applicants on waitlists for Passport funding. Today, there continue to be long waitlists for Passport funding. Ministry records indicate that in March 2012, there were 3,700 individuals waiting for Passport supports. In 2012-2013, the Passport budget was $97.3 million. It increased by $10 million in 2013-2014. As part of the government’s 2014-2015 budget regarding the multi-year developmental services investment strategy, it aimed to eliminate the 2014 waiting lists for Passport funding by 2017-2018. By December 2015, the Ministry had funded 7,200 individuals through that strategy. Although the Ministry told our Office that it remains on track to provide new Passport funding to 5,800 more applicants by April 2018, there were still 14,402 individuals on the Passport waitlist as of December 2015.
Flex funding / temporary supports
72 The Ministry has also provided limited flex funding to address short-term urgent situations. Until June 2014, flex funds were allocated to a lead service agency and distributed by a planning table according to locally developed criteria. For instance, in the eastern region, the relevant community services planning table established three categories of flex funding – urgent response, bridging and respite. Respite funding in that region was capped annually at $3,000 per family, and bridging and urgent response funding were restricted to three months and could only be requested once a year for the same individual. In other communities, different distribution rules applied, creating considerable inconsistency in access to funding.
73 We found that many were confused by the disparity in the distribution of flex funding, which also frustrated our efforts to help adults with developmental disabilities in crisis situations. We raised concerns with Ministry officials about the patchwork approach to flex funding when resolving individual cases. In response, in June 2014, the Ministry standardized requirements for distribution of flex funding, now called Developmental Services temporary supports funding. The funding is intended to address unexpected changes in circumstances and enable individuals to maintain and sustain their living situations and support systems on a temporary basis. The funds are now accessed through local urgent response committees made up of service agencies. The total flex funding provided to all regions in 2013-2014 was $4.5 million. This was increased to $6 million in 2014-2015. At the end of 2015, the Ministry also relaxed some of the restrictions on temporary supports funding.
Transition from children’s developmental services
74 The transition from adolescence to adulthood for those with developmental disabilities and their families is marked by a significant shift in available services and supports. At 18 years of age, access to the Special Services at Home supports ends and individuals may apply for Ontario Disability Support Program benefits. Individuals who were receiving services and programming through the Ministry of Children and Youth Services no longer qualify for children’s supports, and must apply for them through local Developmental Services Ontario offices.
75 In addition, up to the age of 21, many individuals with developmental disabilities participate in daily school programming through the Ministry of Education. After this point, they must rely on day programming that is funded privately or by the Ministry of Community and Social Services.
76 Before May 2011, transitional planning for individuals with developmental disabilities was fragmented. The Ministries of Children and Youth Services, Community and Social Services and Education all engaged in some planning for individuals in these circumstances, but their efforts were unco-ordinated and incomplete.
77 In recognition of the importance of planning for the transition to adulthood, in May 2011, the Ministries of Community and Social Services and Children and Youth Services released the Provincial Transition Planning Framework. The framework contemplated that each region in the province would have a joint ministerial transition planning process, which would include consultation with several stakeholders, including adult and child service agencies and families. An important concept in the framework was that planning was to be proactive and not dependent on parent or guardian requests. As part of the transition planning process, the Ministry of Community and Social Services receives reports from the Ministry of Children and Youth Services on the number of people aged 14-18 who qualify for children’s developmental services.
78 The Framework mandates that transition planning for every individual with a developmental disability must begin by age 14, and eligibility for adult services should be confirmed by age 16.
79 By 2013, another key ministerial partner, the Ministry of Education, was added to the joint initiative. That ministry is responsible for developing transition plans for students with special needs from school to further education, work, and/or community participation (O.Reg. 181/98). On January 31, 2013, the three ministries issued a tri-ministry memorandum as an addendum to the framework.
80 In accordance with the tri-ministry memorandum under the guidance of the ministries and relevant service agencies, boards of education, and schools now engage in developing a single, integrated transition plan for each individual with a developmental disability, which addresses their goals upon leaving school. However, the existence of an integrated transition plan does not guarantee an individual access to services and supports at age 18. Many transitions to the adult system result in long waits for services and supports.
81 The situation is somewhat different for children with developmental disabilities who have been made Crown wards. The Ministry of Community and Social Services considers that it has a moral obligation to address the needs of these individuals as a priority. Their Developmental Services Ontario assessments are fast-tracked. In addition, they also have funding attached to them, although supports still need to be created to accommodate them in the adult system.
82 In March 2016, the Ministry revealed that as part of the provincial Special Needs Strategy to assist children and youth to receive timely services at home, school, in the community and as they transition to adulthood, it will be investing $17.8 million over the next three years.
Applying for services
Confirming eligibility
83 All applications for adult developmental services and supports must be made through local Developmental Services Ontario offices. A psychological assessment is normally required to demonstrate the degree of disability contemplated by the Services and Supports to Promote the Social Inclusion of Persons with Developmental Disabilities Act, 2008. While individuals can pay for psychological assessments privately, every Developmental Services Ontario office offers Ministry-funded psychological assessments provided by third party assessors on contract. Recently, the Ministry has encouraged Developmental Services Ontario offices to identify best practices for improved efficiency and consistency to enhance their capacity and help streamline the application process. In addition, $3.5 million was allocated for the next two years as part of the 2014-2015 budget to increase assessor capacity. The Ministry expects the new investment to clear the backlog by the end of March 2017 of those who do not have assessments and are not receiving services.
84 When an eligibility decision is made, it is entered into a database referred to as the Developmental Services Consolidated Information System (DSCIS). There is also a three-level review process to challenge denials of eligibility.
Needs assessment
85 If an individual is considered eligible for services, the next step is a needs assessment. This is based on the person’s application as well as evaluation using the Supports Intensity Scale, which is administered by a certified assessor retained by the local Developmental Services Ontario office. Assessors meet with applicants, usually with their caregivers, and ask a series of pre-set questions. The assessment covers home living, community living, lifelong learning, employment activities, health and safety, and social activities. As circumstances may change over time, Ministry policy requires that all individuals be reassessed every five years, whether they are receiving services or waiting for them. Reassessments may also take place more frequently, if appropriate.
Prioritization
86 The next step in the process involves assigning a priority to the individual for supports and services. This diverges from what was envisioned by the Act. Unproclaimed sections of the Act provide that funding entities will be responsible for prioritization and managing waitlists for services. However, since funding entities do not yet exist, Developmental Services Ontario offices rely on community organizations to assign priorities.
87 Typically, local planning tables are responsible for establishing prioritization processes under the Ministry’s Interim Prioritization Guidelines, and then assigning priorities to individual applicants. There is no standard prioritization process; each of the six regions we reviewed assigned priorities differently.
88 Developmental services sector workers told us that the prioritization process for services and supports varied across the province and was too complicated and ineffective. One case manager from a service agency told us that in her area, the committee responsible for prioritization met once a month at most. In 2014, the Ministry introduced a standardized prioritization tool used in allocating Passport program funds. The tool was later evaluated and the Ministry is considering next steps for rolling out standardized prioritization measures for all services and supports. The Ministry has also committed to taking steps to improve reporting and monitoring of waitlist information.
89 Usually, individuals with urgent needs are rated at the highest priority. Before June 2014, there was no set definition of urgency, though planning tables would often consider situations involving abuse or neglect, high risk of self-harm or injury to others, extraordinary medical intervention and a significant deterioration in a caregiver’s health compromising care to come within this category. In June 2014, the Ministry created a consistent definition of urgency.
90 Once the planning table or other prioritization group has assigned a priority and notified the Developmental Services Ontario office, the next step is for that office to link or match prioritized individuals to available services and supports offered by various service agencies.
Matching and waiting lists
91 Developmental Services Ontario offices are required to gather detailed information from service providers about available supports and services within their regions. They then identify individuals to receive them based on their priorities. Ultimately, it is up to individual service agencies to confirm the suitability of a match.
92 In the case of residential placements, matching to a specific placement only takes place once a vacancy is reported. As of July 1, 2011, all service agencies were required to report residential vacancies to the Developmental Services Ontario offices. By June 2012, all vacancies for services funded under the Act were required to be reported.
93 Unfortunately, the prioritization process typically leads to applicants being placed on several waitlists, as the demand for supports and services far outstrips availability.
94 Historically, every developmental services agency, community, and region kept its own waitlist, often leading to significant duplication and uncertainty as to the actual demand for specific services. In March 2012, the Ministry announced that Developmental Services Ontario offices would be using the new DSCIS data system to hold all the records of individuals receiving or waiting for developmental services. The waitlist data from the agencies has been migrated to the new system. The Ministry plans to add matching and linking functions to the data system by the end of 2016. This function will enable service agencies to report vacancies directly into the database, which will assist Developmental Services Ontario offices in matching and linking individuals to available supports and services.
95 To further complicate the picture, waitlists are not kept chronologically. It is not a “first come, first served” system. Waiting lists are based on prioritization of individuals, from those most in need down to those with very low needs.
Urgent response
96 In accordance with Ministry policy, the Developmental Services Ontario offices are responsible for initiating the urgent response process when individuals present with urgent needs. When there is a crisis creating an urgent need for service, Developmental Services Ontario offices are to refer the case to the regional urgent response process for consideration. Every region has one or more community-based urgent response mechanisms, administered by one or more service agencies.
97 The urgent response process typically involves an agency contacting the individual and/or family affected, as well as any referring agency, to obtain further information. The agency will then try to find a solution. In doing so, it may contact service providers and apply for flex funding. In some instances, the Ministry of Health and Long-Term Care or justice sector officials may be also be contacted. Unfortunately, in many cases there simply are no services or supports available.
Defining urgency
98 When we began this investigation, the Ministry had not provided service agencies with clear and comprehensive direction on what should be considered urgent. It became apparent that there was considerable divergence in the application of urgent response processes across and within regions, and a lack of clarity around what situations should qualify for crisis resources. We repeatedly raised this issue with senior Ministry officials, and in June 2014, the Ministry finally released provincewide Urgent Response Guidelines. The guidelines are intended to support the urgent response mechanism in each region by providing standardized policies, procedures, forms and definitions. Urgent response is defined in the guidelines as follows:
An urgent response shall be considered for an adult with a developmental disability who is at high risk due to the following circumstances:
- the person’s unpaid primary caregiver (e.g. family member) is unable to continue providing care that is essential to the individual’s health and wellbeing; OR,
- the individual has no residence or is at risk of having no residence in the very near future; OR,
- the individual’s support needs have changed to such an extent that their current support arrangement may soon become untenable and their wellbeing is likely to be at risk; AND,
- formal and informal supports are not available to reduce the risk of harm or address the need.
- Any supports provided under an urgent response are time-limited to six months. However, a single six-month extension may be granted in exceptional circumstances, if removal of temporary supports would likely result in the need for another urgent response.
99 The guidelines establish new urgent response committees made up of all Ministry-funded service agencies in specific service areas. The committees are to develop short-term supports for the individual and may also refer complex and difficult cases to the relevant Developmental Services Ontario office for urgent response case management services, which are provided by designated service agencies.
Residential services
100 In December 2014, the Ministry determined, based on a survey of service agencies, that of 33,615 adults obtaining some form of Ministry-funded developmental services, 15,246 were receiving residential services in Ontario. However, nearly as many were left waiting, and that number appears to be growing. The Ministry’s records indicate that some 10,900 were in a queue for some form of residential services in March 2012, while by April 1, 2014, there were 12,808 adults on a waitlist for residential services.[21]
101 The Ministry funds five different types of residential services for adults, ranging from supported independent living in home-like settings to intensive-support residences that provide 24-hour care. The Ministry also funds two types of temporary beds that can be used in crisis situations. There are 31 safe beds, used exclusively for people with developmental disabilities in crisis, and 70 treatment beds, generally intended for people also experiencing behavioural or mental health challenges.[22] In 2013-2014, some 87 individuals in crisis used these beds throughout Ontario.[23]
102 In 2014, the Ministry committed $3 million in annualized funding to explore and test innovative housing solutions. The Ministry also created a Housing Task Force in response to a housing study, which the Ministry had commissioned. The task force is responsible for reviewing and recommending housing projects to the Ministry for funding. In 2015, the task force reviewed 80 proposals and recommended 12, which the Ministry approved for funding. In 2016, the task force issued a second call for initiatives. In May 2016, the Ministry announced that it had approved six projects recommended by the task force for funding over two years.
103 In April 2016, the Ministry told us that as part of the multi-year Developmental Services investment strategy, more than 800 adults with developmental disabilities received new residential supports.
104 When housing is required on an urgent basis, individuals can find themselves in respite beds, temporary safe or treatment beds, but they may also end up in shelters, hospitals, boarding homes, long-term care homes – and even jail.
The Many Faces of Crisis
105 The process for accessing supports and services in the developmental services sector is complex, multi-layered, and inconsistent across the province. The 1,436 individuals, families, caregivers, and other stakeholders we heard from during this investigation were often bewildered by the developmental services system and confused by or oblivious to the distinctions amongst its various parts. Many were discouraged by interminable waitlist delays and desperate for help. Some were on the brink of crisis; others firmly in its midst.
106 The following stories underscore some of the systemic failings we uncovered relating to services and supports for adults with developmental disabilities in crisis. Although the names have been anonymized for reasons of privacy, the circumstances are all too real and tragic.
Victims of abuse
107 Most of the families we encountered during our investigation were fierce advocates and protectors of their loved ones. Unfortunately, this is not always the case. Those with developmental disabilities are uniquely vulnerable and voiceless in the face of domestic assault and neglect. We heard from concerned individuals about 23 adults with developmental disabilities, who had reportedly suffered abuse.
Falling off the cliff: Adam’s story (East Region)
108 Adam, now 23, is a young man with severe autism who functions at a developmental age below five years. He is non-verbal, incontinent, and self-injuring when anxious. He is also a survivor of longstanding parental neglect.
109 In 2011, Adam was living with his parents and attending school. A local service agency was familiar with Adam’s family, and the filthy conditions in their home. However, it closed its file after his parents rejected offers to arrange for cleaning and other services. By December 2011, school officials had become so concerned with Adam’s physical state and poor hygiene that they filed a formal report with the Ottawa Police Service. They explained to police officials that Adam repeatedly arrived at school in soiled diapers, smelling of urine, feces and mold, with his skin often inflamed and raw. His lunch boxes were also regularly unclean and moldy. They noted that attempts at addressing these issues with Adam’s parents had been largely unsuccessful.
110 In early January 2012, Adam’s father acknowledged that he was concerned about the state of his home and Adam’s situation, and requested assistance. He arranged to drop him off at a service agency, which managed to find him temporary lodging and also connected his parents with a service to help clean their home.
111 Fortunately, the Ottawa Police Service has a two-person Elder Abuse and Vulnerable Persons Task Force, familiar with the challenges of adults with developmental disabilities. Its officers took an active interest in Adam’s case. They provided us with a general occurrence report dated January 5, 2012, describing what officers observed in the home:
Upon entering the premises officers found appalling living conditions with a stench so strong it was difficult to breathe. Rotting garbage was all over the house with fecal and other unidentified litter spread over the walls and floors. Piles of dirty clothing were everywhere and it was difficult to walk without stepping on clutter. The bathroom and kitchen were completely unsanitary.
112 As a result of their findings, Adam’s parents were charged with the criminal offence of failing to provide the necessities of life. According to police, Adam’s father was co-operative, but his mother did not comprehend the seriousness of the situation, was aggressive, and assaulted the arresting officer.
113 By the end of January 2012, the Office of the Public Guardian and Trustee had become Adam’s guardian of property, responsible for administering his Ontario Disability Support Program benefits as well as respite funding.
114 After the court prohibited Adam’s parents from caring for him while charges were pending, his stay in the temporary placement was extended. However, even though Adam was effectively homeless, he had no access to secure residential funding. As he did not personally have the financial resources to pay the cost of the placement ($256 a day), the agency providing the housing was forced to approach the local community service planning table to request additional funding. In the six-month period Adam was housed by this agency, flex funding to cover his residential costs was only approved for one month, leaving the agency with a significant budget shortfall.
115 Meanwhile, the police officers dealing with Adam’s case became increasingly concerned that agency officials, responsible for facilitating Adam’s access to residential and other services, were planning for Adam to return home if the charges against his parents were dropped. Arrangements were apparently underway for their house to be renovated and cleaned and for special-needs workers to attend if Adam returned.
116 On June 29, 2012, Ottawa police contacted the Ministry of Community and Social Services to emphasize that Adam would not be returning home to his parents, regardless of whether or not the charges were dropped. The officers told us that Ministry and service agency staff kept saying there was no money available for Adam’s housing needs. If Adam were discharged from temporary care, the officers feared they would have to apprehend him and take him to hospital for his own protection. As one remarked:
We went straight to the Ministry, and said, “What is going on? How can you say that this young man, with all of the needs that he’s gonna have ahead of him, has got nowhere?” There’s nothing. There’s no money. There’s nothing…
All [the case management agency] wanted was for [Adam] to go home. Like, there’s a home there, the parents want him…. They really were pushing for him to go home, despite everything. Despite, as well that there are court conditions on these parents to not have any contact with him.
117 Later that same day, the local community service planning table approved additional flex funds for Adam. The next day, he was moved to a new temporary placement, but there was still no permanent solution in sight.
118 In July 2012, the Crown withdrew charges against Adam’s parents, but only on condition that they never seek custody of him again. A peace bond was also issued limiting their contact with Adam until July 25, 2013. One of the conditions of the bond was that the parents would work with officials and provide support and co-operation so that the agency providing case management services could ensure Adam was well cared and provided for and not harmed in any way. This particular term incensed the case management agency. Astoundingly, one official even wrote the Crown attorney to explain that the agency was not:
…responsible to ensure any aspect of the young man’s care or security. We have no such legal duty, and no capacity to fulfill such an expectation… The care and safety of [Adam] is the dual responsibility of his legal guardians and whichever service provider assists the family.
119 By August 2012, Adam’s temporary funds were again due to expire and he was once more facing the prospect of homelessness. Eventually, in September, additional funding was approved to see him through to the end of October. But it was only on December 27, 2012, that the Ministry finally approved sufficient funding to cover Adam’s daily housing costs retroactively for November and December. After that, temporary funds were approved sporadically. In May 2013, a permanent vacancy became available, which appeared to be a perfect fit for Adam. His name was put forward, but the space ended up going to another man who required it on an urgent basis after his desperate family had abandoned him.
120 By October 2013, Adam’s presence in the temporary community residence was causing strain on the other three occupants, who were significantly older; 86, 63 and 51 years of age, with milder disabilities and mobility issues. Although Adam’s behaviours and condition had improved significantly since coming into care, the agency believed that he would derive greater benefit from a placement with peers.
121 In February 2014, Adam finally moved to a permanent placement at another agency better suited to his needs. The next month, annualized funding of $91,250 was approved for his housing. In June 2015, the Ministry reported that Adam was continuing to do well in this placement, and that his challenging behaviours had decreased in intensity and frequency. By February 2016, preventative intervention and behaviour management protocols had proved successful, and Adam was volunteering with Meals on Wheels, and participating in swimming, music lessons, and community outings.
122 Unfortunately, even though police removed Adam from his home to protect him from abuse, for a period of over two years, he faced an uncertain fate, dependent on temporary placements and intermittent funding. It is unconscionable that the developmental services system did not raise a warning flag earlier to protect Adam from the abuse he suffered. It is also shocking that once he was identified as a victim of neglect, he was left in limbo for so long. The 2015 coroner’s inquests into the deaths of Guy Mitchell and Jamie Hawley also reinforce the importance of ensuring that there are adequate measures and monitoring to prevent abuse and neglect in the developmental services sector. Witnesses at the inquest into Guy Mitchell’s death described the home-share environment he lived in as having no running water, no heat, with floors covered in feces, urine, and vomit, toilets overflowing with human waste, and no food in the fridge. A case worker testified that she visited the home two days before Guy’s lifeless body was discovered, but claimed she never noticed anything amiss – a statement the coroner’s counsel described as “incredibly astounding.”[24]
123 Similarly, the inquest into the death of Jamie Hawley revealed a series of missed opportunities to prevent and respond to his plight, on the part of police, social assistance, and health agencies.[25] One of the recommendations from the inquest into Jamie’s death was that the Ministries of the Attorney General and Community and Social Services jointly create a committee including ministry and stakeholder representatives, for the purpose of developing a mechanism for mandatory reporting of risk of harm to vulnerable adults.
Failure of early warning system
124 Since January 1, 2011, agencies serving individuals with developmental disabilities are legally obligated by Quality Assurance Measures regulations to immediately report to police any instances where alleged, suspected or witnessed incidents of abuse of a person with a developmental disability may constitute a criminal offence.[26] Abuse is defined to include any action or behaviour that causes or is likely to cause physical injury or psychological harm or both, or results or is likely to result in significant loss or destruction of their property and includes neglect.[27] Agencies must have policies and procedures relating to abuse prevention and reporting and provide mandatory training on prevention, identification, and reporting for all their staff and volunteers.[28]
125 Service agency case managers and one clinical psychologist told us that in the past, concerns about client confidentiality often prevented developmental services workers from reporting suspected abuse. However, even with the present reporting requirements, there appears to be uncertainty about their scope.
126 In Adam’s case, Ottawa police officers told us that support workers had previously observed filthy conditions in Adam’s home, and had documented that his mother insisted they wash Adam in a bathtub soiled with fecal matter. However, they had never alerted police. We questioned an official from the case management agency that had been dealing with Adam’s family about why it did not alert police to the situation. She told us she was aware from support worker accounts that Adam’s home was a “hovel,” and the agency’s case file recorded the difficulties some workers had experienced there. However, she explained that because case managers had not been physically present in the home, they could not report the situation to police. She told us there had been no home visits arranged, since Adam’s parents preferred to meet at the agency’s office. Accordingly, once Adam’s parents rejected further services, consistent with the agency’s normal practice, it closed the case after six months of inactivity.
127 It is troubling that the service agency in Adam’s case interpreted its reporting obligation so narrowly and incorrectly. The wording of the regulation clearly captures situations where abuse is also alleged or suspected, not just cases when staff members directly witness abuse. In Adam’s case, there was documented evidence of neglect in the agency’s files, which should have triggered a report to the police. However, no concrete action was taken to address his circumstances until school officials blew the whistle in December 2011. As one police officer said: “They left this kid rotting, literally rotting in this house.”
128 While the Quality Assurance Measures regulations place the responsibility for reporting abuse on service agencies, the Ministry has an obligation to ensure that agencies are fully aware of and complying with their duties. Accordingly, the Ministry should regularly and actively monitor and audit service agencies to confirm that they are meeting their reporting responsibilities. It should also educate agencies on the importance of their legal obligation to immediately report abusive situations to police. For this purpose, the Ministry should develop outreach materials, in consultation with police and other stakeholders, which explain what is involved in reporting to police, types of circumstances where this must be done, the possible outcomes e.g. criminal charges, and use examples, such as Adam’s case, to illustrate why it is imperative for reporting to be done at the earliest opportunity. The coroner’s jury reached similar recommendations in considering the death of Guy Mitchell, addressed at improving training to identify abuse or neglect within host family settings. In response to those recommendations, the Ministry is also testing a system for anonymous public reporting of abuse.
Recommendation 1
The Ministry of Community and Social Services should regularly monitor and audit agencies serving adults with developmental disabilities to ensure they are meeting their regulatory responsibilities to report abuse to police.
Recommendation 2
The Ministry of Community and Social Services should engage in education and outreach efforts with agencies serving adults with developmental disabilities concerning their legal obligation to report incidents of abuse to police, and include examples such as Adam’s story to emphasize the importance of early reporting.
Give me shelter: Layla’s story (East Region)
129 Layla has been diagnosed with pervasive developmental disorder, autism, an intellectual disability and psychiatric and behavioural problems. In 2011, when Layla turned 18, her behaviour significantly deteriorated. Her conduct compounded an already tense situation in the home and she began to experience abuse at the hands of her mother, who suffers from her own mental health challenges. In the spring of 2012, police and developmental services officials intervened and Layla was removed from her home for her own protection.
130 The local Developmental Services Ontario office’s assessment confirmed that Layla required alternative housing on an urgent basis. Unfortunately, there was no available safe bed for her. According to her case manager, Layla was moved to more than 20 locations in a period of 34 days because there was no suitable placement. During this period, Layla was housed in several shelters. Her case manager described to us how completely vulnerable Layla was in this type of setting, observing that she:
…didn’t … understand the culture of the shelter. Didn’t understand the amount of violence, the drugs, the prostitution, all of that. It was not safe for her to be around that. Not that the shelters didn’t want to serve her, but for her own health and safety, it was not right.
131 One of the reasons Layla was moved so frequently, even when funding was approved for one-on-one support staff, was because her needs were considered too high, particularly for the shelter system. For instance, she often ran out into traffic and tried desperately to get into passing cabs. She could also become quite aggressive. In one placement, she did extensive damage, breaking televisions, clay planters, a computer, a microwave and other items.
132 Some violent episodes resulted in Layla spending time in hospital, as there was nowhere else for her to go. At one point in the summer of 2012, Layla’s father left his employment in Western Canada and moved to Mississauga to care for her. But the arrangement did not work well. He could not obtain funding for adequate supports in the home, and Layla missed her school in Ottawa. Within a couple of weeks, Layla broke down, became hysterical, and destroyed property in her father’s apartment. Police were called. It became apparent that living with her father was not a viable option for Layla. Since the shelters would not take her, local hospitals would only do so for short periods if at all, and there were no openings available in the developmental services system, Layla found herself back living with her mother.
133 Within hours of Layla arriving back in Ottawa, the police were called, and she was taken to hospital. After two weeks in hospital, she returned to live with her mother. Her case manager explained to us that it took two and a half months of advocating before she could arrange for two hours of staffing a day for Layla at home. However, even with this assistance, Layla continued to experience aggressive episodes. To compound the situation, her mother’s mental health continued to deteriorate, and she lashed out verbally and physically towards Layla. Layla’s health declined and in response to the stressful environment, she began struggling with an eating disorder.
134 The Ministry’s serious occurrence reports document sporadic violent incidents in the home. One report from February 2013 records that Layla’s teacher and case manager observed that she had scratches, bruises and bite marks on her hand. Layla confided to them that her mother had hit and bitten her over the weekend. In February 2014, another report describes an incident in which Layla’s mother hit and screamed at her, when she accidentally woke her up. An April 2014 report notes that police were called after Layla was again verbally abused, threatened and hit by her mother, and she responded by breaking objects in the home. Another report from just 12 days later details incidents involving Layla and her mother, in which Layla was yelled at, threatened and hit, and the police were once again called to the home.
135 After being labelled as the highest priority for housing for over two years, Layla finally received a temporary residential placement in June 2014. A flex funding request prepared around this time for submission to the local community services planning table noted that Layla could not return to “an abusive situation in her family home.” It recorded that her case manager had ongoing contact with the Ottawa Police Service, that Layla had been physically, emotionally and verbally abused, and that she was living in fear. It also observed that police, Layla’s doctor, and school staff all felt that it was urgent for her to be placed in a safer setting. In addition, it was recorded that previous attempts to access shelters, domiciliary hostels and similar temporary placements had been unsuccessful.
136 According to the Ministry, Layla moved to a permanent vacancy in August 2014, but her mental health issues limited her ability to adapt to this setting. She returned home in January 2015 and received clinical, counselling and case management services. In September 2015, Layla transitioned to a residential placement in the community. The Ministry told us she is doing well, accessing dietician and psychiatric supports, and participating in community outings.
Safe room
137 In Layla’s case, when she first desperately needed to escape a volatile home situation in 2012, instead of finding refuge, she was stuck with a series of inappropriate temporary placements, including in hospitals and shelters. Without proper supports, she was forced to go back to an unstable and unsafe home, where she was subject to periodic verbal and physical abuse. Similarly, even when charges had been laid against Adam’s parents, service agency staff continued to consider placing him back home as a viable solution. If not for the efforts of Ottawa police, it is possible that Adam would have been returned to live in squalour and face further neglect.
138 The Ministry does not have any statistical information about the number of adults with developmental disabilities who have been discovered in abusive home situations. However, the police officers that assisted Adam explained to us that his case was not an isolated incident. For example, they told us about 18-year-old twin sisters – one who functioned cognitively at the level of a seven-year-old, the other at that of an 11-year-old – who had reported abuse to school officials. Their father, who regularly beat them with a bamboo stick, was subsequently charged with assault, and the twins had to be removed. One of the officers explained that service agency staff told her to take them to a homeless shelter. Knowing the danger that a shelter environment would present for these vulnerable young women, the officer sought out other options and was able to arrange for a relative to take them in. Unfortunately, the sisters eventually returned home, after apologizing to family members for bringing dishonour to the family for disclosing the abuse.
139 The officers also referred to a situation involving a woman with both a developmental disability and mental illness, who was living in an untenable situation at home. They explained that workers from social agencies refused to give them a statement detailing the abuse she was suffering because there was no place for her to go. The officers told us that the support workers felt that the young woman would be better off staying in a neglectful situation than ending up on the streets with her parents charged with abuse.
140 The limited number of available safe beds serves to undermine the regulatory requirements for reporting abuse. To be effective, the system for responding to abuse must include adequate provision for emergency placement of victims until permanent housing arrangements can be made. While agencies must report abuse, once police act on a report and a vulnerable adult is removed, they need someplace to go. The unfortunate reality is that emergency spaces for adults with developmental disabilities are not easy to come by, regardless of the reasons for an individual’s homelessness. There is simply insufficient capacity built into the system to deal with cases like Adam’s and Layla’s. As one official from the Developmental Services Ontario told us, the Ministry needs to:
…entrench in their budget some method of dealing with folks that are removed from their home because of abusive situations. You can’t open the door and just fall off the cliff.
141 The police officers that helped Adam also suggested to us that there should be emergency funding and a bank of workers available to assist adults in these situations. They told us that officials from developmental services agencies seemed to be under the impression that the police could simply lock up homeless adults with developmental disabilities for the weekend for their own protection, particularly, in cases where these individuals might be violent. The officers flatly rejected the proposition that a cell is a safe place for someone so vulnerable. They also observed that it is inappropriate to rely on the hospital system to house people in these circumstances.
142 The Ministry should provide clear direction to Developmental Services Ontario offices, as well as service agencies, that returning victims of abuse to their abusers’ care should never be considered an option. Instead, officials should be directing their efforts at arranging for temporary safe housing and secure permanent housing elsewhere. The Ministry should also collect information from service agencies and police services about the number of individuals with developmental disabilities who have been subject to abuse in the home. The Ministry should be making specific residential and other supports available to address these situations. Statistical information about abusive situations will help in planning for these placements and supports.
143 In addition, the Ministry should consult with the Ministry of Community Safety and Correctional Services, as well as police services throughout the province, to promote the establishment of specialty police units, able to address situations involving abuse of adults with developmental disabilities – similar to the model used by the Ottawa Police Service. In Ottawa, when police receive a call that an adult with a developmental disability is at risk of harm by a caregiver or someone else they are dependent on for supports or services, it is answered by the Elder Abuse and Vulnerable Persons task force. Task force officers have developed expertise and knowledge of resources available in the developmental services sector and can investigate allegations of physical, financial, and sexual abuse, as well as failure to provide necessities of life.
Recommendation 3
The Ministry of Community and Social Services should direct Developmental Services Ontario offices, as well as service agencies responsible for placing and/or housing adults with developmental disabilities, that victims of abuse should be placed in safe and secure housing and not returned to the care of their abusers.
Recommendation 4
The Ministry of Community and Social Services should regularly gather statistical information from agencies, as well as police services across Ontario, to identify the number of situations in which adults with developmental disabilities have been the victims of abuse by caregivers.
Recommendation 5
The Ministry of Community and Social Services should make specific resources available to be used in urgent situations to provide safe housing and services where an adult with developmental disabilities is the victim of abuse and requires removal from their home for their protection.
Recommendation 6
The Ministry of Community and Social Services should consult with the Ministry of Community Safety and Correctional Services, as well as police services throughout the province, to promote the establishment of specialty police units able to address situations involving abuse of adults with developmental disabilities.
Shelter shock
144 Whether a crisis arises because of domestic abuse or individuals find themselves homeless for other reasons, shelter housing remains a recourse of last resort in the developmental services system. Shelters are an inappropriate option for adults with developmental disabilities, particularly those who function with low intellectual capacity. We received six complaints about individuals housed in or referred to shelters in the absence of alternative residential placements. Shelter environments can be overwhelming, confusing and frightening for adults with developmental disabilities. For instance, Ottawa police officers told us about a young man with autism and significant developmental delay, who was thrown out of his home at Christmas because his parents were no longer able to cope. He was apprehended under the Mental Health Act and brought to hospital, but was not admitted, as he was not mentally ill. The officers’ only option was to take this man, who functioned at the level of a 9-10-year-old child, to a homeless shelter. He went missing the next day, but was later discovered hiding in his bed, terrified.
145 Several case managers told us they have placed clients with developmental disabilities in shelters because there was no other choice. As one case manager at a service agency said, shelters are now:
…being over-inundated with our clients because there’s no room in our system … We’re having to suggest shelters to our clients when we whole-heartedly know it’s not the right option, but it’s better than the streets, obviously. We know they’re getting fed. We know they have a bed. It’s far from ideal, but they’re getting their medication. The complete minimum, minimum basics are there, but it’s not right.
146 When we interviewed Dr. Susan Farrell, a clinical psychologist with the Royal Ottawa Mental Health Centre who has specialized training and experience working with individuals with developmental and mental disabilities, she told us quite bluntly that shelters are a wholly inadequate place for these individuals to be placed.
147 According to the Ministry’s December 2014 analysis of service agency survey results, over 300 adults with developmental disabilities have been living in domiciliary hostels or boarding homes. While the Ministry’s survey is a start, in order to understand the full scope of this issue, the Ministry should obtain additional and ongoing information from community shelters, service agencies and Developmental Services Ontario offices about the number of individuals with developmental disabilities who are forced to use shelters. It should also ensure that there are sufficient crisis beds specifically designed to serve those with developmental disabilities for use in urgent situations. Finally, the Ministry should create an online provincial inventory of these resources that is easily accessible to police and developmental services sector officials. There should be clear recognition that, in the case of individuals with developmental disabilities and dual diagnosis, homeless shelters and similar temporary options are completely unsuitable.
Recommendation 7
The Ministry of Community and Social Services should regularly collect statistical information about the use of community shelters by adults with developmental disabilities, which can be used for planning for crisis supports and services.
Recommendation 8
The Ministry of Community and Social Services should ensure that there are adequate crisis beds throughout the province to serve the urgent needs of adults with developmental disabilities.
Recommendation 9
The Ministry of Community and Social Services should create an online provincial inventory of crisis beds easily accessible to developmental services and police officials.
Recommendation 10
The Ministry of Community and Social Services should provide direction to service agencies that homeless shelters and similar temporary options are unsuitable for those with developmental disabilities and dual diagnosis.
Please call back during business hours
148 Developmental Services Ontario offices operate during normal business hours Monday to Friday. Unfortunately, crises often happen at night and on weekends. For instance, when the young Ottawa man was expelled from his home at Christmas, no service agency was open. The responding officers were faced with no alternative but to leave him at a shelter, an option they recognized was unsuitable.
149 Several witnesses we interviewed suggested that there should be an urgent response process operating 24 hours a day, seven days a week, across the province. The Ottawa Police Elder Abuse and Vulnerable Persons Task Force officers we spoke with noted that they can get emergency funding from the city for a hotel, but a vulnerable adult with a developmental disability who functions at a low level cannot be left alone in a hotel. They recommended that a bank of workers be available to assist.
150 Ottawa Police told us they faced a similar issue with vulnerable seniors found in crisis situations outside of regular business hours. In one case, the officers described that they rescued a battered senior from a home at 3 a.m. on a Sunday, and there were no services available to assist her. As a result of this and similar incidents, the police worked out an arrangement with a local seniors’ residence, which agreed to take seniors in crisis at any time on a moment’s notice. After the young man with developmental disabilities went missing from the shelter, officers met with a key service agency in the region to try to work out a similar arrangement for adults with developmental disabilities. However, no resolution was reached.
151 In recognition of the fact that crises are not limited to business hours, and to deal with cases where individuals are in urgent need of assistance, the Ministry of Community and Social Services should ensure that caregivers and emergency service workers such as local police have recourse to urgent response mechanisms on a 24/7 basis. There should be an agency or individuals in every region, who can always be reached to arrange for temporary emergency placements of vulnerable adults with developmental disabilities. There should also be funding available for crisis workers who can assist individuals in these circumstances – for instance, remaining with them to provide temporary support in hotels or other crisis placements, until more permanent and appropriate housing can be organized.
Recommendation 11
The Ministry of Community and Social Services should develop an urgent response mechanism that is available and accessible province-wide on a 24-hour, seven-days-a-week basis.
Recommendation 12
The Ministry of Community and Social Services should ensure that crisis workers are available to assist adults with developmental disabilities who require urgent assistance to access temporary residential placements.
Breaking point: Nancy’s story (East Region)
152 Abuse of adults with developmental disabilities in the home is intolerable. Regrettably, lack of adequate supports can contribute to the development of abusive situations. We have seen cases where family members who have had to cope with their loved ones’ unpredictable and aggressive behaviour for prolonged periods succumb to emotional and psychological burnout, and physically and emotionally lash out in frustration at the very children they have nurtured and protected.
153 When our Office was first introduced to Nancy, she was 20 years old. Nancy has a severe developmental disability arising from a childhood illness. She is non-verbal, but can communicate through some sign language, and functions at the level of a young child. Nancy’s behaviour deteriorated significantly as she went through late adolescence, and her parents, both in their sixties, found themselves progressively unable to manage her violent rages in the home. Nancy regularly sleeps only a few hours a night. It is also common for her to awake agitated and begin lashing out at those around her, typically her mother.
154 Over the years, Nancy’s mother has desperately sought additional relief. She has openly acknowledged that she has gone through periods where she has felt so helpless that she has contemplated suicide and feared that she would turn to violence. In fact, Nancy’s mother made this clear in a series of letters she wrote to the Ministry, in which she begged for more help.
155 In August 2009, she wrote the Ministry’s regional office about Nancy’s aggressive behaviours and explained the family was in crisis describing how “we feel like we are hostages, in constant fear and dread of what her behaviour will be like every day.”
156 In August 2010, she wrote a similar letter to the regional office, emphasizing how her marriage was suffering and admitting, “sometimes, I am so emotionally overwhelmed that I fear that I might treat her violently.”
157 By June 2012, a case manager described Nancy’s parents as “incredibly burnt-out.” Nancy’s violent episodes were more acute in the home environment, where her parents had difficultly successfully implementing behaviourial management strategies. Her case manager suggested, “I’m sure their level of exhaustion has a lot to do with this.” The situation further deteriorated when Nancy finished school and there were no day programming supports in place. Recognizing how fragile Nancy’s mother was becoming with no stable funding for supports in sight, the case manager encouraged her “to only think of the future in blocks of three months at a time.”
158 As a result of our intervention in the fall of 2012, Nancy began receiving serial flex funding and her parents were able to temporarily cobble together day programming supports for her, using this funding, Passport benefits and their own savings. Nancy’s name was also placed on a waiting list for residential placements, but there were no vacancies. However, by August 8, 2013, Nancy’s mother wrote yet another letter, this time escalating her concerns to the Minister:
Our situation has not changed since 2009 except for the fact that we are older, exhausted beyond belief, helpless, and at our breaking point. … Her behaviour is aggressive, difficult, and her disrupted sleep patterns have put immense strain on our family. Sometimes, I am so emotionally overwhelmed that I fear that I will treat her violently. We live in a constant state of fear for the future of our family.
159 Nancy’s mother’s calls for help went largely unheeded, and tragically, she began to succumb to the urges she had tried for years to suppress. On August 26, 2013, Nancy’s case manager filed an enhanced serious occurrence report with the Ministry, recording that a day program provider was concerned that the situation with Nancy’s family was getting volatile and presented a safety risk. She noted that the parents were exhausted, neither parent was sleeping, and the mother “admitted to feeling very resentful.” The case manager also documented her own discussion with Nancy’s mother:
She admits to feeling so drained and angry, she is having negative thoughts. [Nancy] is only sleeping 3.5 hours and she can’t think properly. [Nancy] is very cranky and screaming and hitting them all the time, sometimes she slaps [Nancy] back. She reports that after slapping [Nancy] back, [Nancy] stops hitting for a while and that she doesn’t want to continue doing this because she knows it is wrong.
160 Nancy’s case manager committed to attempting to get some emergency respite for the family. The police were contacted but did not take any further action. After the occurrence report was filed, some flex funds for respite services were obtained, but the situation did not improve significantly.
161 In September 2013, Nancy’s mother admitted to the case manager that she had been using her hands again to stop Nancy from hitting her. The police were called once more, but did not intervene. A month later, Nancy’s case manager was able to secure additional temporary funds to assist with Nancy’s programming. However, Nancy remained at home in the care of her aging and beleaguered parents. It was only in early 2015 that Nancy began to receive stable respite and day supports. She has since found a residential placement in the community, where she is reportedly doing well.
Reporting of serious incidents
162 Agencies serving adults with developmental disabilities are required to report various incidents to the Ministry’s regional offices under the March 2013 Serious Occurrence and Enhanced Serious Occurrence Reporting Guidelines. The guidelines identify eight categories of serious occurrences that must be reported, including:
- Death of a client while participating in a service;
- Serious injury of a client while participating in a service, including medication errors that result in illness;
- Alleged, witnessed or suspected abuse;
- Any situation where the client is missing;
- Disaster on the premises;
- A complaint about the operational, physical or safety standards;
- A complaint made by or about a client involving a serious occurrence, for instance, when a client has been criminally charged, has assaulted someone or been assaulted by another client or by a non-caregiver, complaints concerning sexual contact between clients, and admissions to hospital as an inpatient; and
- Restraint of a client.
163 The guidelines also differentiate between a serious occurrence and an “enhanced” serious occurrence. An enhanced occurrence involves situations where emergency services have responded to a “significant incident” involving a client, and/or the incident is likely to involve “significant” attention from the public or media. Service agencies must have a designated authority appointed who is responsible for determining if an incident is an enhanced serious occurrence.
164 Service agencies must send a report within 24 hours for serious occurrences, and within three hours for enhanced serious occurrences. The report form is faxed to the regional office on weekdays, and to a weekend early alert system on the weekends. The guidelines also indicate that in the case of incidents where the suspected, alleged or witnessed abuse may constitute a criminal offence, the agency must call the police immediately. This includes neglect, defined as “the failure to provide a person with a developmental disability with the support and assistance that is required for their health, safety or well-being and includes inaction or a pattern of inaction that jeopardizes the health or safety of the person.”
165 Service agencies must also submit an Annual Summary and Analysis Report of all serious occurrences to the Ministry every year.
166 The Ministry’s regional office is responsible for reviewing and responding to all occurrence reports as well as the annual reporting. It may identify trends, issues or items requiring follow-up by the service agency, and monitor outcomes.
167 Serious occurrence reports are also reviewed and used by the Ministry’s Developmental Services Compliance Unit in its compliance audits, focused on ensuring that service agencies meet the regulated quality assurance measures.
168 Enhanced serious occurrences are all sent to the Assistant Deputy Minister of the Community and Developmental Services Division, who can direct the regional office to take specific action to redress problems and can also ask for an immediate compliance audit.
169 What the Ministry’s reporting scheme fails to capture are situations like Nancy’s, where for years the Ministry received a series of early warnings that Nancy was at risk of abuse at the hands of her mother, whose emotional state was progressively deteriorating as a result of limited community supports. It was only when the risk materialized and Nancy was abused that an occurrence report was sent to the regional office. As Nancy’s case illustrates, well-intentioned but exhausted parents may become abusive if left with no hope or relief. The Ministry should have actively engaged with service providers when it first became aware of the situation, to ensure that Nancy’s interests were protected through available programming and services. The Ministry should develop a process for service agencies to immediately report to its regional offices and for Ministry staff to effectively respond to information received from parents, caregivers, service agencies or others that an adult with a developmental disability is at risk of abuse in the home – beyond the current process for reporting of serious occurrences. The Ministry should closely monitor and proactively address these situations by ensuring urgent supports are made available to minimize the potential for abuse.
170 At present, the Urgent Response Guidelines lack sufficient detail to clearly qualify a family such as Nancy’s for urgent services until the point when abuse actually materializes. The Ministry should ensure that the Urgent Response Guidelines specifically include circumstances where caregivers, service agencies, Developmental Services Ontario, police services or other officials identify that there is an increasing risk of abuse of an adult with developmental disability by overextended caregivers. If a broader and clearer definition of urgent circumstances had been in place, Nancy’s situation might not have descended into violence.
Recommendation 13
The Ministry of Community and Social Services should develop an expanded reporting system so that service agencies, Developmental Services Ontario offices, police or other officials can identify situations where there is potential for an abuse to develop, if adequate developmental services and supports are not provided on an urgent basis.
Recommendation 14
The Ministry of Community and Social Services should expand the definition of urgent circumstances in the Urgent Response Guidelines to address situations where a risk of abuse has been identified.
Institutionalization by Default
171 In principle, the government has decried the concept of placing those with developmental disabilities in large institutions. However, in reality, hundreds of adults with developmental disabilities still find themselves living in institutional settings in Ontario. The lack of appropriate residential resources in the community has, by default, resulted in many adults with developmental disabilities being inappropriately housed in hospitals, long-term care homes and even in jails, for prolonged periods. In July 2016, the Ministry told us that it was planning for some 250 individuals, living in hospitals and long-term care facilities, who were on waiting lists for residential supports.
Hospitalization – the Band-Aid solution
172 Adults with developmental disabilities can periodically require acute care within a hospital setting for a host of medical issues. Those with a dual diagnosis may need to be admitted to hospital to address acute psychiatric issues, often in specialized settings. However, all too frequently, after their acute symptoms have subsided with treatment, adults with developmental disabilities remain hospitalized, commonly in psychiatric units, because there is no alternative safe and secure housing for them in the community.
173 This situation is unacceptable on a number of levels. To begin, developmental disability is not an illness, and should not be treated as one. These individuals should not be held in facilities where they are exposed to infection, and which do not have the training and resources to provide appropriate programming and supports. This situation also has a domino affect, reducing the number of acute care beds available to those experiencing medical crisis. In addition, housing healthy individuals in hospitals places considerable financial and resource pressures on hospital administrators. In the case of individuals who represent a flight risk or are aggressive, some hospitals have had to hire additional security and/or outside support workers to prevent the individuals from harming themselves or others.
174 We received 79 complaints that raised the issue of using hospitalization as a Band-Aid solution to address the lack of residential placements in the developmental services sector. Some of the affected individuals had been hospitalized for years. In one case, a 33-year-old man lived in hospital for seven years because of his aggressive behaviour. A 40-year-old man lived in a psychiatric unit for more than five years because his elderly parents could not manage his volatile conduct in their home. Our Office worked with the Ministry of Community and Social Services to address these cases and successfully facilitated 20 individuals moving from hospital into community placements.[29]
12 years too long: Peter’s story (East Region)
175 Peter has been diagnosed on the autism spectrum. When he was 15, Peter was placed in residential care, as his single mother was struggling to manage him at home. Since 2002, he has spent the better part of 12 years in psychiatric hospitals, after the agency that had been providing him with adult group housing found him too aggressive to handle.
176 At age 36, Peter functions cognitively at the level of an 18-month-old child. He is non-verbal, often crying and crawling like a baby. We learned about Peter in November 2013 from a social worker at the mental health centre where he was living on the schizophrenia unit, although he has not been diagnosed with schizophrenia. The social worker was trying to help his mother find him services, and expressed concern that Peter was progressively deteriorating as a result of his extended institutionalization.
177 We were told that typically Peter’s days began on the unit with him sitting on the floor. If he was not kept active, he became progressively aggressive. He often hit other patients, and was normally placed in physical restraints a couple of times a week. Understandably, the psychiatric hospital was not equipped to provide Peter with the developmental services, staff and structured activities necessary to stimulate and calm him. In 2012, arrangements were made for support workers to take him out for weekly outings. However, these were insufficient to meet his needs.
178 Peter had been given the highest priority on the waiting list for a residential group placement in 2006. Beginning in March 2012, he had also been discussed at the local community services planning table. But he had never been selected for any of the residential vacancies arising in the community. A senior hospital official who was involved with attempting to facilitate Peter’s transition to the community explained to us that while members at the community services planning table “very eloquently expressed that of course a hospital should never be considered a home,” Peter was not considered a priority because he was living in the hospital.
179 Peter’s case was one of those that our Office worked on actively and followed closely. We made repeated inquiries and alerted senior Ministry officials to our concerns about his continued hospitalization. Finally, after 12 years in institutional purgatory, Peter was approved for funding to allow him to move to a placement created for him and another individual with high needs. The move was initially set to happen on September 1, 2014, but it still took another eight months. He is now in his new home in the community, where we understand that he is doing well.
Room, board and restraints: John’s story (West Region)
180 John is 29 years old and lives with cerebral palsy and global developmental delay. He is non-verbal and often becomes very upset and engages in harmful behaviour; he bangs his head, and hits, bites, and grabs people, sometimes causing serious injury. For many years, John’s family was able to look after him in the home with available developmental supports. However, eventually their circumstances shifted. His younger brother, who used to help with John’s care, suffered a traumatic brain injury in 2008. His mother also began experiencing health problems, including stroke activity. As the family underwent increasing strain, John’s behaviours began to escalate. His parents realized that keeping him at home was no longer an option, and his name was placed on a waiting list for residential supports.
181 While the family waited for John’s name to come up for a residential placement, his self-abusive and violent behaviours increased. John did not have a case manager, but fortunately, he was matched with an adult protective service worker. Adult protective service workers normally provide supports to individuals with developmental disabilities living independently in the community, although in John’s case he lived with his family. The Adult Protective Service Worker program can be accessed through Developmental Services Ontario offices and is provided by various service agencies in the province. Under this program, a worker meets regularly with an adult who has a developmental disability to help with access to services and developing life skills.
182 John’s worker stepped in to assist the family navigate the developmental services system and seek increased supports. In December 2012, she wrote to a program supervisor at the Ministry’s regional office and the local Developmental Services Ontario office, urging them to find additional resources for the family and emphasizing: “The stressors within their family unit are reaching a breaking point, as are the health, safety and well-being of the family.” On February 1, 2013, the Ministry’s regional director wrote in response to an inquiry from the family’s Member of Provincial Parliament, urging the family to work with local service providers.
183 On August 7, 2013, John was brought to the emergency department of the local hospital. He had been running at vehicles, bit a support worker and hit his mother. There was nothing medically wrong with him, but he was admitted because it was considered unsafe for him to return home. One-to-one nursing supervision was ordered, as well as medication to keep him calm.
184 By August 23, 2013, the hospital’s vice-president contacted the assigned Ministry program supervisor, notifying her that John’s behaviours had become unmanageable. He had injured several staff and was trying to grab patients. Nurses were turning down shifts because they did not want to work with him and the hospital had to provide 2:1 nursing care to try to keep him under control. The hospital subsequently transferred John to a mental health unit at another hospital for a psychiatric evaluation. The Ministry’s program supervisor also confirmed with Developmental Services Ontario that John had been waitlisted for various developmental services.
185 By August 30, John was back in the local hospital after the psychiatric assessment confirmed his issues were related to his developmental disabilities, not a psychiatric disorder. John was not sick, did not require hospitalization, and the hospital wished to discharge him. But his parents expressed that they could no longer care for him in the home, a position supported by John’s adult protective support worker. Accepting that returning John home was no longer a viable option, the hospital continued to care for him for non-medical reasons.
186 In November 2013, with no sign of any community placement for John on the horizon, the hospital’s Chief Executive Officer wrote to the program supervisor in frustration. He observed that the physical environment of the hospital posed restrictions on John’s level of activity and independence and exposed him to illnesses and infections. He noted that the only area for John to run in was the hallway, amidst staff, equipment, and at times fragile elderly patients. He also remarked:
[John’s] agitation increases when the acute care unit is busy which can lead to outbursts of physical aggression towards staff and patients. … He exhibits self-harm and chemical restraint is necessary at times to keep him safe. Acute care hospital staff are not trained in long-term management of mentally challenged patients.
187 He emphasized the high cost – $417 a day – associated with keeping John in an acute care setting, and that doing so was not in John’s “best interest physically or emotionally.”
188 The program supervisor’s November 18 response to the hospital was discouraging. It spoke in general terms of strengthening supports for individuals like John, of new funding for the developmental services sector, and working “diligently towards an equitable and sustainable system of services,” while knowing that even increased funding would “not fully meet the growing demand.” In John’s specific case, the program supervisor noted that some supports had been provided and that his case was under consideration by various community tables. But the bottom line was that for the foreseeable future, John was still the hospital’s problem.
189 Ministry records indicate that the hospital’s Chief Executive Officer phoned the program supervisor on November 29, again expressing concerns and apparently signalling that if John’s housing situation remained unresolved, his family would be billed for food and lodging – or he would be discharged “to the community.” From the Ministry’s perspective, not much could be done. The proper procedures had been followed. John was in the queue with others for services, and he was ineligible for urgent response funding because he required a permanent solution, not a short-term one.
190 On December 2, 2013, the regional office notified the Assistant Deputy Minister of Community and Developmental Services Division of the situation involving John’s extended hospitalization.
191 On January 17, 2014, the hospital Chief Executive Officer made another pitch to the Ministry. He called the program supervisor, noting that John would cost the facility about $230,000 annually for staffing and food, and he was involved in up to eight violent incidents a month. He requested additional supports to assist with John while he was in hospital.
192 Our Office had also been following up with the Ministry on John’s case, and we sought regular updates from senior Ministry officials – including the Assistant Deputy Minister – about the status of efforts to find him a community placement. In February 2014, the Assistant Deputy Minister told us that $25,000 had finally been approved to provide support workers for 16 hours a day during John’s hospital stay. Annualized funding had also been approved of $200,000 for a community placement. By this point, internal Ministry records suggest that given the abject failure of the system to provide a remedy, it was working around the normal procedure for filling residential vacancies. Instead of awaiting a determination that John was the most in need of an identified placement, an upcoming vacancy was specifically earmarked for John, and efforts were directed to ensure that it was renovated to match his needs.
193 In July 2014, after nearly a year in hospital, John was discharged to a group residential setting in the community, where the Ministry told us he continues to thrive.
No place for him: Tommy’s story (Toronto Region)
194 At 23 years of age, Tommy is 6’2” tall and weighs 200 pounds. He has diagnoses of autism and developmental delay, is non-verbal, incontinent and needs assistance with daily activities. He has lived most of his life with his parents, who are newcomers to Canada, his younger sister (now 16), and grandmother (now 84).
195 Tommy has a history of assaulting and injuring others. He will hit, scratch, bite, and pull hair. He has also destroyed property, stolen food from others, and engaged in inappropriate touching, as well as episodic tantrums and outbursts. Sometimes he does not sleep for days and becomes very destructive. His behaviour is unpredictable and he requires extensive support. He dislikes respite group homes and the primary responsibility for his care has rested with his family.
196 Tommy, like many young men with developmental disabilities, experienced an escalation in violent episodes as he entered his late teens. In March 2012, his severe aggression in the home led to a 10-day hospital stay in a psychiatric intensive care unit (PICU). After he was released, the local Community Care Access Centre[30] provided him with one hour per day of personal support, Monday to Friday, and he was assigned a case manager through a local agency. However, Tommy continued to present a challenge for his family and in September, the Community Care Access Centre increased in-home supports to two hours a day. He was also waitlisted in October for a treatment bed. Unfortunately, by then, Tommy had already experienced repeated hospitalizations as a result of severe aggression.
197 On October 16, 2012, a psychiatrist wrote to Tommy’s case manager concerned about his recurrent hospital admissions (73 days in total for 2012 at a cost of $2,000 a day):
This is his sixth admission to this unit, totalling 8 visits to the hospital between the period for March 12 this year and today. It is quite disheartening to see this young man is frequently admitted to the PICU with seriously mentally ill adult patients although he has not been diagnosed with any type of mental illness other than autism. As we have told you in the past admissions, this is not the place for him. We are forced to admit him as there is no other place in the hospital we can “hold and house him” when the paramedics drop him off.
We have discussed several times that what [Tommy] needs is proper housing where there are trained staff who are able to understand him and deal with his behaviour. We do not have training and expertise to deal with him. If properly housed, he does not have to be locked up with a group of unpredictable, psychotic patients….
198 By January 2013, Tommy had been suspended from school for hurting a staff member and two students. His parents wrote the Ministry and others, including our Office, explaining their lack of success in obtaining residential care for their son. In February, Tommy was admitted to hospital after injuring treatment workers and his father.
199 By March, arrangements had been made for Tommy to receive 2:1 supports on a 24-hour-a-day basis while in hospital, because of his aggression towards staff and other patients. Officials also began to actively discuss discharging him back to his family’s care, and by March 8, he was back home with 2:1 support workers for 12 hours a day “to keep his family safe,” along with a behavioural therapist for 12 hours a day. Tommy only required one 24-hour hospital visit due to aggressive behaviour while these supports were in place.
200 Our inquiries with various officials revealed that while efforts had been made to find Tommy a treatment bed, he had not been presented to the local community service planning table to access other resources, such as residential placements. There appeared to be some confusion between the Ministry and service agencies as to the proper process to follow in these circumstances. In the end, the planning table did not consider Tommy’s case until March 25, 2013. Tommy was waitlisted that month for group home placements, treatment and day supports. Efforts also continued to find him a treatment bed. However, Tommy’s family was baffled and frustrated by some of the placement suggestions put forward. For instance in April 2013, despite Tommy’s high-level needs, a vacancy was considered at a home for youths involved with the criminal justice system who could independently use public transportation. It is hardly surprising that in May, the family was informed that Tommy had been rejected for the vacancy.
201 On June 17, 2013, Tommy finished high school. Without school to attend, Tommy became progressively restless and his behaviour declined. Despite this, support services in the home were reduced. On June 19, the family told us that only one worker was present in the home to assist and Tommy was becoming agitated. Apparently, instead of providing a second worker for support, the agency suggested calling the police if the situation escalated. By July 12, a support worker from the Community Care Access Centre was providing two hours of physical support a day, one treatment staff member was attending four hours a day, and a behavioural therapist continued to attend daily.
202 By August 2013, Tommy was attending a three-hour-a-day community program paid for by the family. There were no longer any workers assisting in the home. On August 20, police intervened after Tommy grabbed his mother’s hair and arm and refused to let go. He was admitted to hospital, where external support workers were brought in to manage him on a 9-to-5 basis. Finally, on September 3, Tommy was discharged home, on the understanding that he would enter a treatment program in October. He was provided with workers in the home, however, this time only from 1 to 5 p.m. On September 23, Tommy’s aggression once again landed him back in hospital, where he remained until he was transferred to a temporary treatment bed on October 28. The Ministry told us that Tommy has benefitted from the treatment and services in this placement, including a day program. However, he is still waiting for a permanent home in the community.
A hospital is not a home: Riley’s story (East Region)
203 At the age of three, Riley’s single mother left him in the care of his grandparents. Riley has a number of diagnoses including autism, obsessive compulsive disorder, schizophrenia and epilepsy. For many years, Riley’s grandparents managed his needs effectively. However, during adolescence he became increasingly unpredictable and destructive. By the age of 18, his aggressive episodes often led to him choking his grandmother. The family was able to obtain some respite services, but the situation declined further when his grandfather died in 2007.
204 Riley had some access to respite services, but his aggression limited his ability to participate in day programs. By mid-2011, he was attending a program only once a week. In the summer of 2011, Riley’s grandmother, who was grappling with her own health problems, was unable to cope with Riley’s impulsive and violent attacks. In desperation, she contacted the local Developmental Services Ontario office, asking that Riley be put on the crisis list for immediate residential placement. In response, Riley was assessed as a high priority and his name went on the waiting list for the next suitable vacancy. Months passed without any relief and in May 2012, Riley’s grandmother tried again to access emergency residential supports to deal with Riley’s increasingly uncontrollable behaviour. She was again unsuccessful. Finally, in September 2012, during a visit to his psychiatrist, Riley’s violent conduct – including trying to strangle his grandmother, hitting a worker, and running around the office spitting and hitting walls and windows – earned him an admission to the psychiatric ward of the local hospital.
205 Riley’s grandmother resisted early attempts by hospital administrators to discharge him to her care and he remained in a secure ward under guard. In October 2012, we contacted the Ministry for an update on efforts to find Riley a residential placement in the community. Ministry officials told us that matching Riley with a vacancy would be difficult without the proper assessments. They observed that he was now stable and explained that he had been one of nine candidates considered for a vacancy, and even made the list of the final three contenders, but was ultimately rejected because he was not considered homeless.
206 It was clear that a hospital ward was not a suitable home for Riley. He was disruptive and on occasion assaulted others. He spent considerable time locked in his room, restrained and sedated. A hospital social worker expressed the view that Riley was at risk, as he was exposed to others who were extremely unwell and potentially dangerous.
207 The local case resolution committee eventually approved funding for behavioural assessment and additional support workers during Riley’s hospital stay. However, a worker from a local service agency told us that Riley spent considerable time walking around in a hospital gown and was often locked in the bathroom, where he played with his own excrement.
208 By December, the Ministry told us that hospital officials were anxious to discharge Riley into the community. His grandmother also said they were exerting considerable pressure on her to send Riley to a private group home for psychiatric patients. She did not agree to this option, as the home was not equipped to deal with the needs of adults with developmental disabilities. She also expressed concern that hospital staff were not following the behaviour plan that had been developed for Riley.
209 Around this time, we contacted the local health integration network (LHIN) and raised the Joint Policy Guideline for the Provision of Community Mental Health and Developmental Services for Adults with a Dual Diagnosis, which encourages co-operation and co-ordination between the ministries responsible for individuals who have both psychiatric and developmental diagnoses. The LHIN later confirmed it had reminded the hospital to follow the guidelines. Riley’s conduct reportedly improved once the hospital complied with the behaviour plan.
210 Despite Riley’s compelling situation, during one of our Office’s requests for an update, a Ministry official responded that she was not a “case manager,” and was unfamiliar with the details of individual cases. However, after we raised Riley’s circumstances with more senior officials, we were told that he would be considered for three residential vacancies. By January 2013, Riley’s Passport funds were depleted and he was in danger of losing the support workers who had been working with him in hospital. That same month, the hospital placed Riley under the supervision of two security guards, as he was apparently biting nurses. Unfortunately, because of Riley’s high needs, he was rejected by the community agencies that had vacancies. The Ministry regional director explained:
It’s not because we don’t want to match, but we’d be having a different conversation if we matched and something happens to either the individual, another client or staff. So it’s not as easy as it sounds. “You have a space. Put them in.” So those are some of the challenges that we’re facing. Even though we may have a space, what’s the match?
211 Ministry officials were sympathetic to Riley’s circumstances, and acknowledged that his case was not flagged as urgent early enough, but they generally expressed that there was not much that could be done except to wait for a vacancy. They told us that the three group homes in the region that serve complex needs clients were full and there were no extra funds. Officials also explained that Riley was going through the standard matching process. When we asked the Ministry why Riley was being put forward for vacancies at agencies that later said that they could not support his needs, we were told that the agency with the vacancy must first interview the individual before deciding whether the placement was suitable.
212 In February 2013, Riley remained inside the hospital under guard. His grandmother told our Office that hospital administrators continued to pressure her to take him home with her. She described being bullied to have him admitted to a privately run care home and a retirement home (with no daytime support staff or activities). Neither of these option was suitable and she held her ground.
213 Then, on February 27, the Ministry prepared an internal decision note, posing two options for Riley’s care. The first option involved providing $320,000 for a vacancy that was not otherwise funded by the Ministry. The “cons” associated with this option included that this move might “be perceived as preferential treatment,” given there were 50 clients identified as in urgent need of a placement in the region because of challenging behaviours, homelessness or imminent homelessness. It was also noted that Riley was only one of three people in the region in a similar situation – an adult with a dual diagnosis in hospital pending an appropriate permanent placement. In addition, it was suggested that choosing this option would set a precedent and encourage other families to come to the Ombudsman’s Office “for desirable supports for their adult child.” The second alternative was for Riley to remain in hospital while “creative permanent placement options were explored in the funded system.” The cons associated with this option included the government appearing unresponsive to clients with urgent needs, and potential media interest. In the end, the Ministry chose the first option.
214 Riley’s grandmother was likely unaware of the Ministry’s internal deliberations about his fate when she penned a letter to the Premier on March 4, 2013. She carefully laid out the details of her three-year struggle to find Riley a home, and her heartbreak at witnessing him trapped in a locked hospital ward, routinely sedated, and forced to wear a hospital gown:
This whole scenario, since September 14, 2012, has completely exhausted me and as a resident of Ontario, I am appalled that such a vulnerable person can be treated in this manner.
In summary, I am asking you, as the Premier of Ontario, why have things come to this end? Here is a severely mentally challenged young man, who cannot find a secure and safe environment in which to spend the rest of his life. I keep asking the DSO people, “what will happen to him when I die?” One said, “We will then find a group home for him.” Others said, “we really don’t know” and I believe that the second answer is more truthful.
…trust me, there are hundreds, maybe thousands of other people, in the province, that are in similar situations to that of my grandson. Please take a look at the other psychiatric wards in local hospitals throughout the province, where parents and grandparents, who are aging or who are too ill to care for these very special adults … have no other solution but to abandon the person they love with all their heart.
215 Before the Ministry’s housing plan for Riley was put into action, another Ministry-funded placement materialized, projected to be vacant in May. Despite spending months responding to our Office that Riley had to wait for the routine matching process to run its course, Riley was fast-tracked for and guaranteed this vacancy. A revised internal Ministry decision note dated March 21 said:
Funding for [Riley] in this permanent placement will be determined pending assessment at that time. This placement overrides current … Region protocols regarding filling vacancies and matching clients to appropriate placements.
216 One of the many drawbacks of housing individuals with developmental disabilities who are otherwise stable and medically fit in hospitals is that they risk becoming ill through exposure to other patients. In Riley’s case, he suffered two bouts of pneumonia during his stay, and his transfer to the community was delayed after he developed a serious viral infection requiring medical isolation. Today, after more than seven months in hospital, Riley is living in a group home in the community where he receives behaviour management supports.
Hospital waiting room: Annette’s story (North Region)
217 Transition points, such as adolescence, can often trigger crisis for adults with developmental disabilities. The senior years can also lead to a negative shift in circumstances, leaving adults with developmental disabilities in crisis. Annette is a 66-year-old with a developmental disability and schizophrenia. She lived most of her life with her parents, but in 2002 moved to a community group home. Annette has a history of violence and can be a flight risk. Two support staff were required to supervise her while she was in a group home. As she aged, Annette developed additional medical complications, including dementia and a neurodegenerative disease. She required intermittent hospitalization when her condition became acute, but continued to live in a group home until December 2011, when the agency that supported her could no longer meet her increased needs and she was admitted to hospital.
218 Annette’s condition stabilized and she did not require hospitalization. However, there was no facility in her northern community capable of meeting her needs. She was rejected by at least five homes because of concerns about her behaviours. As a result, Annette spent three years in the sterile confines of a hospital. As one health centre official described the situation:
It’s a huge frustration in having to live in a highly restricted hospital environment with people who are really very ill and not having the opportunities for community integration and development and recreation and social … none of that.
219 In January 2015, after considerable efforts on the part of our Office, the Ministry approved funds to assist with Annette’s transition to the community. After more than three years in hospital, Annette moved to her new community home in April 2015 and is now receiving Passport funding for community participation.
When Health and Social Services Collide: Hospitalization of Adults with Developmental Disabilities
220 The worlds of health and developmental services frequently intersect – especially for those living with a dual diagnosis, who may find themselves hospitalized during crisis periods. When the need for acute medical intervention subsides, they often remain in hospital awaiting appropriate community placement. One developmental services case manager we interviewed told us that she has had clients who spent four or five years in hospital because there was simply no capacity in the developmental services sector to accommodate them. Sometimes they are discharged into long-term care facilities, even if they are young adults.
221 In hospital parlance, individuals who do not require acute or complex specialized hospital care but occupy beds for extended periods are referred to as “alternate level of care” patients. The hospital sector has a longstanding concern about such patients improperly diverting finite medical resources. Unnecessary hospitalization also affects specialized in-patient programs targeted for individuals with developmental disabilities. For instance, the Centre for Addiction and Mental Health in Toronto operates a Dual Diagnosis Program, which is in high demand. The Centre’s in-patient program is intended for short-term stays, averaging four months, and is focused on providing differential diagnosis, medication review and stabilization of clients to allow them to safely return to the community. However, the in-patient unit only has 10 beds, and in April 2013, the program’s Director told us that about eight of the existing beds were “blocked” by clients with complex needs – because they could not be discharged to their families and there were no appropriate high-support housing alternatives in the community. Prolonged hospitalization of individuals in this program has undermined its intent and individual patient progress. A Centre official told us:
… we watch them improve and do really well and there’s kind of an optimum point for discharge but they can’t and then they go through cycling, up and down, while they’re awaiting discharge. And they themselves become depressed and withdrawn. So it becomes quite problematic. And to sustain the changes and the effects (of treatment) is very difficult in a hospital environment…. And what we have is our most expensive resource serving the smallest number of people, and it should be exactly the opposite kind of scenario and model – that was the original intent.
222 Another Centre official observed: “It means that we have to, for example, bring in extra staff. We’re spending a lot of money on a very small population. And we’re not treating them. We’re not making their problem better. We’re putting them in the wrong environment, and just paying to keep them safe here, because we can’t put them in the right environment.”
223 A 2006 study found that one in eight patients in hospitals providing specialized care have a dual diagnosis. However, 80% were not receiving treatment in programs designed for individuals with dual diagnosis.[31] The study also noted that about 37% of those diagnosed with developmental, mental health and/or behavioural issues were in hospital for over five years. In addition, it determined that only 4% of these adults living in psychiatric hospitals required this level of service and that most would be better served by living in supportive community environments.
224 In September 2009, the Centre for Addiction and Mental Health released a report, commissioned by the Ministry of Health and Long-Term Care,[32] about alternate level care clients, which found that in 2007-2008, there were 570 individuals with dual diagnosis designated in this category. This group had a total of 625 stays in Ontario hospitals that year, for purposes unrelated to typical hospital services. The report also observed that some of the problems relating to serving this population arose from shortage of high-support housing, the need for improvements in assessment, discharge planning and referral processes, and co-ordination challenges. The report recommended an integrated, whole system approach, including a strategy for proper community housing and individualized flexible funding for clients. It urged the Ministry of Health and Long-Term Care’s LHINs and the Ministry of Community and Social Services to continue to work together to develop appropriate residential placements for people with dual diagnosis and for community and hospital teams to be able to provide the necessary supports for this population.[33]
225 Individuals with dual diagnosis are more likely to visit emergency departments than those with mental illness alone. A study in 2011 found that such visits were often strongly linked to major life events such as a change in primary staff, problems with friends or caregivers, or illness or death of a caregiver.[34] The study suggested that one solution would be to focus on the caregiver and provide support and treatment to assist individuals to care for themselves, connect with others, and cut back on the red tape of navigating services. Another study found that adults with developmental disabilities are more likely to present to emergency departments with psycho-behavioural emergencies (usually aggression) than with physical complaints.[35]
226 In 2012, six Ontario psychiatric hospitals, concerned about the rising costs of specialized care, commissioned a review of specialized services for patients with dual diagnosis.[36] On March 31, 2012, all six hospitals had beds occupied by alternate level care patients with dual diagnosis, accounting for 37% of the patients in this category. The report noted that the hospitals needed to find new and innovative ways to address and manage the complexities of these clients with existing resources, transition them back to the community, and utilize outpatient services to prevent hospitalization. It found that there was a shortage of specialized hospital beds and an unequal distribution of beds across the province to serve the needs of this population. The report summarized a number of key stakeholder issues, including:
- Existing education and training for hospital and community staff does not adequately prepare them to meet the complex needs of these patients;
- Pathways are poorly defined for the dual diagnosis population;
- There is limited access to supportive housing with adequate staffing levels;
- There are limited specialized resources and services in hospitals and the community, including proper training; and
- Hospital and community programs are not prepared for new client populations such as the rise in clients presenting with autism.
227 Among its recommendations, the report called for better co-ordination across the province, expansion of collaborative models, and development of a population-specific data collection tool to obtain accurate data to inform decision-making and research.
228 In February 2013, we received a letter signed by the presidents and chief executive officers of the six psychiatric hospitals that had commissioned the 2012 report, expressing concern about the situation and citing relevant research. They observed that:
Patients are most commonly referred to our programs because of aggressive behaviours including self-injury and serial failures in school, home or community environments. These crises occur repeatedly and may involve police and emergency departments. They occur despite multiple and repeated evidence based interventions.
229 They noted that up to 50% of beds in psychiatric hospitals are occupied by individuals who cannot be discharged because of inadequate community supports.
230 Hospitals are intended for acute and specialized complex care not as repositories for individuals with developmental disabilities with nowhere else to go. It places unreasonable pressure on the health system to use hospitals as hostels for adults with developmental disabilities. As the stories of Peter, John, Tommy and Riley illustrate, inappropriate and extended hospitalization can also place individuals at risk of psychological and/or physical harm. Hospital programs are not generally designed – nor are hospital staff normally trained – to address the needs of individuals with developmental disabilities and dual diagnosis. Dr. Susan Farrell of the Royal Ottawa Mental Health Centre told us:
Most providers in hospital settings, unless it’s a specialized unit, feel fairly ill equipped to deal with the needs of the dual diagnosis population. We just don’t have enough education and training for hospital staff to meet their complex needs …
231 As Dr. Farrell also observed, a homeless individual with a developmental disability who ends up in hospital can lose priority for community placements, as local planning tables may consider a hospital bed adequate shelter. This reality is aptly demonstrated in the case of Peter, who floundered for over a decade within the hospital system. Dr. Farrell suggested that the opposite should apply. She believes these individuals should be treated as a priority for community placements because they are occupying a bed that was not planned for that purpose and may be needed by someone else.
232 In its July 2014 report, the Select Committee on Developmental Services expressed frustration about the “lack of available, reliable data in almost every area of the developmental services sector.” One of the recommendations it made was that the Ministry collect information about the number of people with developmental disabilities who are inappropriately housed in hospitals and other locations. The Ministry responded that it was gathering information through various means. For instance, several ministries have supported an interdisciplinary research study on health care use and outcomes of over 66,000 adults with developmental disabilities. Data is being collected on prevalence and health care use patterns of adults with dual diagnosis that may be used by the ministries for planning purposes.
233 Additional information about the frequency of hospital emergency room visits, admissions, and their outcomes would further assist in planning for developmental services. However, the Ministry should also ensure that service agencies, Developmental Services Ontario offices and hospitals regularly report on individual instances of improper hospitalization because of existing gaps in developmental services. The Ministry should communicate directly with developmental services stakeholders to send a strong message that adults with developmental disabilities should not be relegated to hospitals as an alternative to appropriate community settings. It should also work diligently to facilitate community placements on a priority basis for individuals hospitalized in these circumstances. Hospitals should not be seen as a safety net when residential placements in the developmental services sector are unavailable. The Ministry of Community and Social Services should work co-operatively with the Ministry of Health and Long-Term Care and the hospital sector to resolve these situations expeditiously.
Recommendation 15
The Ministry of Community and Social Services should obtain regular information from hospitals across the province concerning emergency visits and admissions of adults with developmental disabilities, including details about hospital stays, their length, and their outcomes, in order to plan for appropriate developmental supports and services.
Recommendation 16
The Ministry of Community and Social Services should send a direct message to Developmental Services Ontario and community service agencies that adults with developmental disabilities should not be left in hospitals where there is no medical need.
Recommendation 17
The Ministry of Community and Social Services should require service agencies, Developmental Services Ontario offices and hospitals to provide regular reports about adults with developmental disabilities who are hospitalized but no longer require hospital care, and maintain an active record of such cases.
Recommendation 18
The Ministry of Community and Social Services and Developmental Services Ontario offices should ensure that individuals identified on its record of alternative level of care hospital patients are prioritized as urgent for community placements.
Inter-ministerial co-ordination and collaboration
234 When we began this investigation in late 2012, there was recognition that more inter-ministerial collaboration and co-ordination was necessary to avoid unnecessary hospitalization of adults with developmental disabilities in crisis. As an Assistant Deputy Minister from the Ministry of Community and Social Services told us then:
Even being in a forensic bed in a hospital is sometimes a form of incarceration, because you can’t get out of there. And there are circumstances where people have been in those beds for long periods of time. Multiple years with really no due process in terms of justice or in terms of alternative service or support. So that will be part of our conversation, about how do we support that.
235 However, the conversations with health system partners were then just starting. There were no protocols in place or clear system accountability. Several health sector agency representatives we spoke to were also critical of the Ministry of Community and Social Services’ approach at the time. One individual told us that she took part in a multi-sector meeting called by the Ministry to address the needs of one individual, which resulted in a plan involving annualized funding of $600,000. She observed that at the meeting, health sector officials told the Ministry that there were 25 or 30 similar cases and called for a more systemic approach.
236 There are now several inter-ministerial committees addressing co-ordination and integration of various health and developmental services supports for individuals with developmental disabilities. These groups include an assistant deputy ministers’ committee representing 14 ministries, which considers social policy development, as well as committees responsible for the implementation of a dual diagnosis framework, addressing issues around transitional housing, considering social policy development relating to health care, and promotion of an integrated lifespan approach for supporting people with complex care needs.
237 There is continued public interest in ensuring that effective results are achieved through inter-ministerial collaboration. In order to keep a spotlight on the work of these committees, and ensure they maintain a steady momentum, there should be regular public reporting through the Ministry of Community and Social Services on initiatives under discussion, timelines for completion, and results.
Recommendation 19
The Ministry of Community and Social Services should report publicly on a regular basis about the work of the various inter-ministerial committees relating to developmental services and the health care system, as well as on the status of initiatives under discussion.
Long-term care: Short-sighted solution
238 We received 14 complaints about adults with developmental disabilities – some quite young – who were left with nowhere to live but long-term care homes. These homes are primarily for the care of seniors, many of whom are frail and suffer from various conditions, including cognitive impairments associated with aging. They were not developed with the needs of those with developmental disabilities in mind, and are another form of institutionalized care often used as a stopgap solution when more appropriate residential placements are unavailable.
Young man, old problem: Patrick’s story (East Region)
239 Patrick was 24 years old when we first learned about his situation. He has cerebral palsy and is non-verbal. He uses his own version of sign language to communicate and occasionally relies on a communicating device attached to his electric wheelchair. When he is not using his electric wheelchair, he tends to propel himself by crawling along the floor. Patrick is dependent on others for much of his care, including feeding.
240 Patrick lived at home with his family for many years. After he turned 18 in 2007, the family received developmental services and disability funding, which went towards respite, day programs, and some home supports. Patrick also qualified for some services through the local Community Care Access Centre, although it was often hard to get personal support workers to come out to the rural family home.
241 As time passed and Patrick watched his brother and friends moving away and on with their lives, he became increasingly frustrated. This manifested itself in aggression, focused largely towards his mother, who was his primary caregiver. As she aged, Patrick’s mother also struggled with the physical demands such as heavy lifting associated with Patrick’s care. By 2011, it was clear to her that Patrick needed to live outside of the family home, and he was placed on waiting lists for residential and respite supports.
242 After months of waiting without any vacancies materializing in the developmental services sector, in November 2012, Patrick moved to the only accommodation available in the community, a local nursing home, funded by the Ministry of Health and Long-Term Care. It was a difficult transition and the home called the police a few times to deal with Patrick’s violent outbursts.
243 Patrick’s mother told us that she was concerned about the suitability of this setting, but she could no longer cope with him at home. She explained:
I want him to be able to go out and do things. To have his day occupied. A young guy, 24 years old – his mind is fine. It’s just his body isn’t working and he’s around all these [elderly, ill people]…. I’m not saying nobody does [spend time with Patrick], but they’re all seniors and some of them have got dementia and that’s the place they should be, not my kid….. Somebody that young should never be in a place like that. But if that’s all you got, that’s what you’re going to do.
244 In early December, Patrick accidentally broke the ankle of a female resident with his wheelchair when he was lashing out in frustration. The nursing home denied him access to his electric wheelchair because of this incident. The next day, he destroyed property on his roommate’s side of the room in a fit of rage and was hospitalized for a few days. Back in the nursing home without use of his electric wheelchair, Patrick resorted to crawling on the floor. He was not allowed use of this wheelchair again for about four months. In late April, he was permitted to use his chair, but only for limited periods and with the speed reduced to the lowest level.
245 Patrick’s rocky adjustment to life in a nursing home was further complicated by the fact that he shared a room with a 75-year-old man with frontal lobe damage resulting from a stroke. This pairing was particularly problematic, given that Patrick’s roommate had a history of being cautioned for inappropriate sexual activity. In 2011, the police had been called after this individual was accused of sexually touching a female resident who has cognitive impairment. In Patrick’s case, nursing home staff had to warn the roommate to leave him alone when they discovered the roommate touching Patrick’s face and neck.
246 Then, in January 2013, in a state of emotional distress, Patrick revealed to his support worker that his roommate had repeatedly touched his groin area at night when Patrick was in bed – sedated and unable to protect himself. The matter was reported to the police, who were familiar with Patrick’s roommate from the earlier incident. Police did not pursue charges in either case. However, a police supplementary occurrence report dated February 12, 2013, noted that the Crown strongly recommended that in order for the nursing home to protect other residents, it needed to keep the alleged abuser in his room, under constant supervision, and away from Patrick and other vulnerable persons. Police also cautioned the roommate and told him not to have any contact with Patrick.
247 The Ministry of Health and Long-Term Care investigated the incident and identified several concerns with the home’s practices. Patrick’s roommate was moved to a private room on another floor and increased security measures were implemented for Patrick’s protection and that of other residents. However, this incident underscored how inappropriate living in the nursing home was for someone in Patrick’s situation.
248 When Ombudsman staff contacted the local Developmental Services Ontario office in March 2013 to discuss Patrick’s housing needs, we were told it had no idea Patrick had been moved to a long-term care home or that he had reportedly been the victim of sexual assault. Soon after, Patrick was placed on another waitlist for community participation supports, and referred to a community planning table for behavioural supports. He was also transferred to a private room in the home. By June, he was granted temporary urgent funding, which enabled him to participate in community activities three days a week.
249 In spring 2014, we learned that a group home was being renovated to create a space for Patrick, and that programming was also being planned, which would allow him an opportunity to participate in community activities five days a week. The Ministry later confirmed that finally, in February 2015, Patrick made a successful transition into the group home, where we understand he is still doing well.
250 Although in certain circumstances a long-term care home might suit the needs of aging adults with developmental disabilities, housing young adults in long-term care homes should be avoided. The Ministry of Community and Social Services should take steps, including consulting with the Ministry of Health and Long-Term Care’s Local Health Integration Networks, Community Care Access Centres, Developmental Services Ontario Offices and service agencies, to ensure that it is notified whenever it is proposed that an adult with developmental disabilities be placed in a long-term care home. If it is clear that this arrangement is inappropriate – particularly given the individual’s age – the Ministry should actively work with relevant organizations to find alternative solutions.
251 Consistent with the recommendation made by the Select Committee that the Ministry collect additional statistics regarding the placement of adults with developmental disabilities, the Ministry should also conduct research and compile statistics on the number, ages, and conditions of adults with developmental disabilities who are housed within the long-term care system. This data should be used to assist with individual and systemic planning for developmental supports, including transitioning younger adults and others, if appropriate, to more suitable community placements within the developmental services sector.
252 The Ministry of Community and Social Services should also regularly monitor adults with developmental disabilities who are housed in long-term care homes. It should enter into a protocol with the Ministry of Health and Long-Term Care to require that it be notified of serious incidents within the long-term care sector involving adults with developmental disabilities, as well as to allow for sharing of complaint and investigative information about such occurrences. This information should be used to assist in planning for better behavioural programs and residential supports for individuals with developmental disabilities.
Recommendation 20
The Ministry of Community and Social Services should take steps to ensure that it is notified when it is proposed that an adult with a developmental disability be placed in a long-term care home.
Recommendation 21
The Ministry of Community and Social Services should actively work with local agencies to ensure that placement of young adults with developmental disabilities in long-term care homes is considered a last resort and that alternative solutions are vigorously pursued.
Recommendation 22
The Ministry of Community and Social Services should engage in ongoing research on how many adults with developmental disabilities are housed within the long-term care system and compile statistics, including age and nature of condition, for use in system planning.
Recommendation 23
The Ministry of Community and Social Services should launch an immediate review of all placements of individuals with developmental disabilities in the long-term care sector, and ensure that any individuals who have been inappropriately placed are appropriately prioritized for transitioning to the developmental services sector.
Recommendation 24
The Ministry of Community and Social Services should review all placements of individuals with developmental disabilities in the long-term care sector on an ongoing basis to ensure that such placements meet individual needs.
Recommendation 25
The Ministry of Community and Social Services should enter into a protocol with the Ministry of Health and Long-Term Care to ensure that it is notified and provided with relevant information about complaints and investigations relating to serious occurrences involving adults with developmental disabilities within the long-term care system.
Duelling program priorities
253 Situations involving placement of adults with developmental disabilities in the long-term care sector are particularly challenging and often involve competing interests and ministerial programs, which have a tendency to operate in silos. For instance, we learned that a partnership involving ministerial and non-profit agency representatives considered a case in June 2012, involving a 26-year-old man diagnosed with autism spectrum disorder who was admitted to a long-term care home from a hospital. The group discussed that this individual was not a good fit for long-term care. The other residents identified that he did not belong there, and even uttered death threats against him. He was also physically strong and there was significant potential for a high-risk situation to develop. If he felt threatened, he could severely hurt an elderly resident. One situation had already occurred, in which he kicked down a door, had to be held down by four police officers, and later spent 72 hours in a mental health unit.
254 The long-term care home and a service agency were prepared to exchange residents to ensure a more appropriate fit. There was a senior in a developmental services placement who was suited to the long-term care home space. The Long-Term Care Home Act, 2007 also contemplates such exchanges. However, the organizations encountered a snag with the developmental services system. The young man was waitlisted with the local Developmental Services Ontario office, and that office believed that allowing him to transfer as proposed would result in unfair queue jumping. In that case, Ministry of Community and Social Services officials agreed to discuss the situation with the local Developmental Services Ontario office. However, the long-term care and developmental services systems must be better aligned to ensure appropriate residential placements. The Ministry of Community and Social Services should take steps to ensure that Developmental Services Ontario offices are educated about options for placements within the long-term care sector, collaborate with officials from the long-term care sector and actively consider creative solutions such as switching placements to better accommodate the needs of adults with developmental disabilities.
Recommendation 26
The Ministry of Community and Social Services should educate Developmental Services Ontario officials and other stakeholders about options for placements within the long-term care sector to encourage greater cross-sector collaboration and the potential for placements to be exchanged to accommodate the needs of adults with developmental disabilities.
It’s a Crime: Incarceration of Adults with Developmental Disabilities
255 After 200 years, it is shocking to learn that society continues to jail individuals with developmental disabilities, some assessed as functioning at the cognitive level of young children. Adults who find themselves in these circumstances frequently experience diminished impulse control and aggression, making it challenging to find appropriate supportive housing in the community. They often live with dual diagnosis. During this investigation, we heard about several cases where incarceration became the failsafe when the developmental services sector could not provide adequate supports. It is nothing short of shameful that we are still imprisoning some adults with developmental disabilities in these circumstances.
256 It has been reported that individuals with developmental disabilities are overrepresented in Canada’s correctional institutions and that this population is growing.[37] We received 27 complaints about adults with developmental disabilities who were charged criminally and another 19 complaints involving the issue of incarceration of adults in these circumstances as a result of insufficient supports and services. The following are some of their stories.
Jailhouse option: Joe’s story (Toronto Region)
257 Joe is 55 years old, with developmental and psychiatric disabilities. He functions at the cognitive level of a six-year-old. He is verbal, but unable to communicate in full sentences. Joe can become destructive when agitated and has a history of substance abuse. He also has a criminal record for various offences including break and enter, theft, and assault. For most of Joe’s life, he has lived at home with his mother, but he has also spent time in group homes, treatment centres and jail. As a result of his disruptive, combative and bizarre behaviour, as well as multiple suicide attempts, Joe typically ends up segregated and alone in protective custody while he is incarcerated.
258 In February 2013, while Joe was in a mental health treatment centre to learn life skills, he was arrested again, and landed back in the correctional system. When Joe received a conditional sentence and probation in late June 2013, requiring house arrest, there was nowhere for him to go. The treatment centre had officially discharged him, given his prolonged absence, and his mother – who was then 81 and suffering from dementia – was incapable of caring for him. Joe had no option but to remain in jail.
259 Some six months later, in January 2014, the Ministry of Community Safety and Correctional Services approved Joe’s release to a 30-day supervised safe bed, run by a community agency, on the understanding that the agency’s staff would work to find him housing and develop a support plan. Unfortunately, Joe’s history of criminal offences led to concerns about his suitability for placement with vulnerable residents, and he was rejected for two vacancies that came up in the winter of 2013. Joe’s stay in the safe bed was extended until March, when he was transferred to another temporary residence with a private agency. The treatment centre had provided 1:1 staffing during his stay, but a few weeks later, the Ministry of Community and Social Services told our Office that the residence found the extra support Joe was receiving disruptive and he would be leaving at the end of April.
260 In May, the agency that initially accepted Joe into a safe bed allowed him to return for another 30-day stay while he attended a day program at the treatment centre. Agency staff told our Office they were also considering accessing the Ministry of Community Safety and Correctional Services’ Special Needs Contingency Fund, which can be used to assist offenders under correctional supervision who have special needs and require specialized services not generally available in their community.
261 Our Office worked with senior government officials at the Ministry of Community and Social Services to facilitate a resolution to Joe’s housing situation. On June 16, 2014, the Ministry initially told our Office that everyone was doing everything they could to ensure that Joe was not returned home. However, it also noted that the agency providing him with the short-term safe bed was becoming progressively concerned about Joe’s extended stay. Later that day, the Ministry was surprised to learn that the agency planned to release Joe back home on June 20, an option that previously had been considered completely unacceptable.
262 While six agencies had refused to take Joe in, Joe’s mother still lacked the capacity to care for him and his brother was also at home undergoing cancer treatment. The agency’s plan was for Joe’s sisters to help care for him with the assistance of support staff for 10 hours a day. The only other choice considered was returning Joe to jail until his probationary period ended in June 2015.
263 Fortunately, with the Ministry’s intervention, the agency agreed to extend Joe’s stay in the safe bed into early July, when he was moved to the treatment centre. His space there was funded from the Special Needs Contingency Fund. In December 2014, Joe moved to an apartment in the community with 24-hour access to staff. He was arrested for assault in August 2015, jailed, and released on March 1, 2016. He is now in a residential placement with increased supports.
Criminalizing crisis: Christine’s story (North Region)
264 Christine, 24, has been diagnosed with a mild developmental disability, attachment disorder, anxiety and depression. She has been connected with developmental services through the local community living organization since she was three. However, Christine presents unique challenges for the developmental services system. She is quite high functioning and strives for independence, but she is also extremely impulsive, prone to engaging in risky behaviours, and capable of frequent violent outbursts. During her temper tantrums, Christine has been known to damage property, make threats and physically injure those around her. Her heightened fight-or-flight instinct also causes her to flee when she feels anxious, and when her behaviours escalate, she often finds herself in the local hospital emergency room.
265 Since she turned 18, Christine has spent little time in the family home, where she has been assaultive, particularly in connection with her mother. Multiple attempts were made to find her a suitable community placement. However, she was unsuccessfully matched with 20 different family home support providers, and even more structured residential living arrangements have failed to meet her needs. Christine’s assaultive conduct has posed a safety risk for developmental support staff and she has faced multiple criminal charges while in community living homes. Christine was initially considered a candidate for the court diversion program, but her history of breaching court-imposed conditions has led to dozens of arrests and numerous convictions and incarcerations.
266 Christine is a safety risk for developmental services system staff. She does not fit the existing system or any of the group homes operated by the local community living agency. By default, local health, police, justice and correctional officials have had to manage her dysfunctional behaviours.
267 In a January 23, 2014 business case in support of annualized funding of $390,000 for Christine, a community agency noted that it did not have the financial capacity to continue to provide the required 1:1 supports, without which she “would be spending most of her time within the police services and corrections system.”
268 Eventually, Christine was moved to a permanent residential placement with 1:1 supports. However, in fall 2014, she was arrested for assault and breach of probation. In February 2016, a service agency told us that Christine is living in an apartment in the community with access to staff supports, has been doing better, and has been out of jail since October 15, 2015.
269 The vicious cycle of incarceration that Christine experienced is a symptom of the inconsistent and unco-ordinated approach pursued by the developmental, health, justice and correctional services sectors towards adults with developmental disabilities in crisis. The resources expended by various provincial and local agencies to attempt to address Christine’s volatile conduct have been significant, but often ineffective.
Order in the courts: Andrew’s story (East Region)
270 Some officials in the justice system have expressed frustration with the lack of resources for adults with developmental disabilities who face criminal charges. Now 25, Andrew has presented significant challenges to both the developmental services and justice sectors and has endured a difficult life. He spent time in and out of the child protective system and was made a Crown ward at age nine. When not living with his mother or grandmother, he spent much of his childhood in group homes and foster care. Andrew has cognitive as well as developmental disabilities, and at age 12 underwent surgery and treatment for brain cancer.
271 Over the years Andrew developed a propensity for attracting negative attention by engaging in risky behaviour. He has been known to lie, set fires, pull fire alarms, make threats, damage property and occasionally become assaultive. He also developed the habit of placing fake 911 calls and making serious false allegations – typically of sexual assault – against his caregivers and others. Andrew’s conduct has repeatedly landed him in trouble with the police. He has been incarcerated several times, often for breaching probationary conditions.
272 Unlike some situations we encountered, Andrew’s criminal justice problems did not necessarily stem from lack of developmental services funding and supports. It was more a question of finding the right fit, rather than securing adequate funding. As a Crown ward, Andrew was allocated somewhere in the range of $180,000 annually for services, which followed him into the adult system. However, his behaviour was difficult to manage and his frequent false charges against service agency staff left him a pariah in the developmental services community. By spring 2013, the agency that had been providing Andrew with residential care declared that it could no longer serve him. It had had to double up on workers to support Andrew in order to ward off abuse allegations, and was no longer prepared to place its staff at risk of false charges. Other agencies similarly indicated that they were not in a position to meet Andrew’s unique needs. His probation officer worked diligently with Ministry officials to bring attention to Andrew’s plight, but there were simply no placements prepared to take him on.
273 Without developmental services supports, Andrew ended up back home with his mother, who has her own challenges and significant difficulty meeting his needs. The situation rapidly deteriorated and after a couple of weeks, Andrew was back in Quinte Regional Detention Centre. He was charged with assault for biting his mother after an argument over a lighter, as well as with breaching probation. During his stay in jail, Andrew was housed in isolation in a segregated cell for his own protection. Essentially, he was in solitary confinement for administrative reasons.
274 Cases like Andrew’s present a quandary to the justice system, which must balance safety considerations and the rights of accused. On July 25, 2013, a Justice of the Ontario Court of Justice was faced with deciding whether to release Andrew into the community without adequate supports or keep him in jail. While recognizing that Andrew should not be locked up in a custodial environment, the presiding judge declined to release him back into the community without a satisfactory plan of care. After a prolonged case conference with various health, justice, and developmental services officials, to discuss Andrew’s future, the Justice observed in frustration:
We have met with various services representatives and just finished a two-hour session, in fact, with a number of people trying to determine what resources can service [Andrew]. There are none. No one is stepping forward to provide service to him. No one can offer any alternative but to lock him up or to send him to Motel 5 on a welfare chit where he would be totally un-serviced. That is totally unacceptable. He is not someone, in my view, who can survive independently without resources being made available on an intensive basis for him. There is no institutionalized or other facility other than a custodial environment by way of incarceration, which has been offered to service [Andrew’s] needs…. I need some answers as to why there’s no facility and why no one has stepped forward to provide resources for someone who is both entitled to receive them and in need of them.
275 In fact, the Justice took the exceptional step of issuing subpoenas for the Deputy Ministers of Health and Long-Term Care and Community and Social Services, so they could testify before him under oath at the next court date “as to why there’s no facility for [Andrew] to be released to.”
276 On August 12, 2013, the Justice relieved the deputy ministers from their subpoenas, after Ministry officials explained that because of the risk of false allegations, no service provider was prepared to take Andrew. Faced with the prospect of Andrew continuing to live indefinitely in a jail cell or return to the community without suitable developmental services supports, the judge reluctantly released him to his mother’s care. All those engaged in looking for a placement for Andrew agreed the situation was untenable in the long term. At one point in September 2013, Andrew ended up at a motel after he started a fire while cooking at home alone. His probation officer maintained regular contact with Andrew, trying to keep him from reoffending. However, police officials began expressing increasing concern that his behaviour at home was deteriorating. By October, Andrew was again incarcerated after fighting with his mother. However, this time some progress was finally made in securing him a residential placement.
277 While no local agency was prepared to help Andrew, an agency from another area of the region agreed to provide services based on a projected budget of about $300,000, in annualized funding. Andrew moved to this new residence after he was released from jail. Although this was a positive development, caring for Andrew continues to present its challenges. In 2014, there were frequent incidents requiring police attendance to deal with Andrew, and local officials raised concerns about the drain on municipal resources. Andrew is still subject to a probation order. However, at least some progress appears to have been made in finding him a home outside of the correctional system. He is living in his own apartment with staff supports.
Redirecting justice
278 Individuals like Andrew, Joe and Christine, who through a confluence of circumstances present unique challenges to service providers, should not be left adrift. The criminal justice system is not an answer. The correctional system is ill-equipped to deal with these individuals. Correctional officials typically resort to keeping them in isolated segregation cells, a practice that has been labelled cruel, inhuman and degrading by the United Nations and has been publicly criticized by the Federal Correctional Investigator, Ontario’s Human Rights Commissioner and my Office.[38] Jail should not be used as a last-ditch recourse because there are insufficient supportive placements in the community.
279 Legal concepts can be particularly mystifying for individuals with developmental disabilities and lack of understanding of key requirements can lead to recurring run-ins with the criminal justice system. An executive director of a service agency told us about one young man with developmental disabilities in his twenties, who was brought before the courts to address breaching a restraining order obtained by his former girlfriend. However, he had difficulty grasping the legal implications of the order. The executive director described the following exchange with a judge:
Judge: You broke the restraining order. You can’t go back to your girlfriend’s house. What are you going to do?
Accused: Go back to see my girlfriend.
Judge: Okay, you can’t go back to see your girlfriend. She has a restraining order. She doesn’t want to see you. Where are you going?
Accused: Yeah, I’m going to see my girlfriend.
280 This particular accused had been repeatedly ejected from residential placements because of his conduct, and ended up in a boarding house without developmental supports. Eventually, he was admitted to hospital while waiting for a proper community placement.
281 There are court diversion programs in the province. However, traditionally their focus has been on meeting the needs of those with mental health issues.
Mental health courts and diversion
282 In Ontario, mental health courts accommodate the special needs of mentally ill persons who are often repeatedly charged with minor criminal offences. These courts routinely divert individuals away from the criminal justice system – for example, staying charges for those who agree to treatment, monitoring compliance with conditions and sanctioning non-compliance. Various mental health and legal professionals are involved in these courts, including social workers, psychiatrists, and duty counsel.
283 The Ministry of Health and Long-Term Care funds mental health diversion and court support services for those charged with low-risk offences whose mental health needs can be met through services based in the community. Diversion services may be available before or after a conviction to link individuals to community or institutional mental health services. Court support services are provided to assist judges and support individuals with mental health needs and their families with the legal process, and with referrals to required services. Court support workers link accused individuals to community and mental health supports and services, and may work with the Crown and others to put together community-based diversion plans. They also educate accused individuals and their families on court procedures and provide advice to the courts on treatment-oriented disposition options.
Dual diagnosis justice case managers
284 Since 2006, the Ministry of Health and Long-Term Care has provided funding for dual diagnosis justice case managers, administered through the Ministry of Community and Social Services. In 2013, this represented $1 million in annualized funding for 23 case managers across the province, most of whom work part-time. These case managers are accessed through Developmental Services Ontario offices and assist individuals with dual diagnosis. Their primary goal is to reduce the number of these individuals who enter the criminal justice system, and/or decrease their time in the system. They create a support plan in collaboration with the Crown and defence counsel. While they advocate for non-custodial disposition, when this is not an option, they will call for shorter sentences, or even, at times, longer sentences so individuals can access jail-based treatment programs. These case managers also assist in institutional discharge planning for adults with a dual diagnosis and help educate correctional officers about working with this population.
285 Currently, justice case management services are reserved for those with dual diagnosis or with serious behaviour or anger management issues, and as the cases we reviewed demonstrate, not all individuals with developmental disabilities have access to a case manager who can facilitate non-custodial resolution of criminal matters. Many fall through the system cracks. There are insufficient supports to ensure that adults with developmental disabilities, as opposed to those with mental health challenges, are safeguarded within and diverted from the criminal justice and correctional systems.
286 Even when justice case managers are involved, this does not necessarily result in successful court diversion for those with dual diagnosis. According to 2012 statistics compiled by the Southern Network of Specialized Care, of the 38 clients served that year, only three entered into court diversion programs. While some were never incarcerated, this group served a total of 191 days in jail in 2012.[39]
Improving justice alternatives
287 In its July 2014 report, the Select Committee encouraged the use of mental health courts and other alternative diversion mechanisms for individuals with a dual diagnosis in the justice system. However, existing court diversion programs, while an extremely positive development in the justice system, may not be particularly effective in dealing with complex behavioural issues relating to developmental and cognitive disabilities. For instance, both Christine and Andrew regularly breached conditions established through diversion programs to the point where they were no longer eligible and landed in jail.
288 In Andrew’s case, officials from different sectors began to discuss his situation and seek solutions through necessity. However, this communication was ad hoc and largely dependent on the efforts of people like his probation officer and a concerned judge. At present, there is no easily accessible, co-ordinated and organized inter-ministerial response to address hard-to serve-adults with developmental disabilities who are at risk of incarceration.
289 In recognition of the unique vulnerability of adults with developmental disabilities within the justice and correctional systems, the Ministry of Community and Social Services should ensure that there are adequate case management and court support services available to co-ordinate an urgent response in cases where any individual with a developmental disability is charged with a criminal offence, arrested and/or incarcerated. Such services should not be limited to individuals with a dual diagnosis. There should be support workers available to liaise with families, service agencies, and justice and correctional officials to minimize the negative impacts on adults with developmental disabilities and assist in finding supportive resources, including supervised residential placements, in order to avoid or reduce any period of incarceration.
290 The Ministry should also undertake research and consult other relevant ministries and stakeholders with a view to promoting development of specialized court and diversion programs tailored specifically to the needs of individuals with developmental disabilities. Unlike many living with mental illness, individuals with developmental disabilities are not necessarily in need of medical treatment to control their behaviours, and may be incapable of meeting standard conditions imposed by the courts as an alternative to incarceration. They do not fit the typical profile of persons whom the mental health courts and diversion programs were designed to serve.
Recommendation 27
The Ministry of Community and Social Services should ensure that there are specialized case management and court support services available for all individuals with developmental disabilities involved with the criminal justice and correctional system.
Recommendation 28
The Ministry of Community and Social Services should create positions or retain service providers to be responsible for co-ordinating an urgent response in cases where adults with developmental disabilities are or are at risk of being charged with criminal offences, arrested and/or incarcerated, including liaising with families and relevant officials and securing supportive resources and services, such as residential placements.
Recommendation 29
The Ministry of Community and Social Services should undertake research and conduct consultation with subject specialists concerning the creation of specialized court diversion programs addressed specifically to the needs of adults with developmental disabilities.
Recommendation 30
The Ministry of Community and Social Services should work with the Ministry of the Attorney General and the Ministry of Community Safety and Correctional Services to support specialized diversion programs for individuals with developmental disabilities who are charged with criminal offences.
Building Community Capacity
291 The continuing lack of suitable community placements for individuals like Joe, Christine and Andrew within the existing developmental services system is extremely troubling. In Andrew’s case, despite general acknowledgement that he required significant supports, and the fact that funds existed to pay for them, service agencies were at liberty to refuse to help him.
292 Rather than depend on community organizations to fill the void, the Ministry should take ownership of this issue and invest time and effort on developing a system of secure residential supports, designed to assist in diverting adults with developmental disabilities who may suffer from uncontrollable, impulsive and/or violent behaviour, away from the criminal justice and correctional systems. If the Ministry has difficulty incenting private service providers to take on this task, it should consider a direct service model. It is unconscionable to saddle the courts and correctional services with the task of jailing adults with developmental disabilities and dual diagnosis because appropriate supports are unavailable in the community.
293 We understand that in late 2015, the Ministry of Community and Social Services entered into a Dual Diagnosis Transitional Rehabilitation Housing Program, together with the Ministry of Health and Long-Term Care. The program will provide transitional community housing for eight individuals who are in a forensic hospital as a result of coming into contact with the law and have been found unfit for trial or not criminally responsible. While this is a positive step, others like Joe, Christine and Andrew, who would not qualify under this program, still require sufficient supports to break the cycle of incarceration.
294 The Ministry should work with the Ministries of Health and Long-Term Care, Attorney General and Community Safety and Correctional Services, and consult with subject experts, to create a responsive and proactive approach to managing these individuals who repeatedly find themselves in crisis with the law.
Recommendation 31
The Ministry of Community and Social Services should take the lead and work with other ministry partners to develop a responsive and proactive system of residential supports to divert adults with developmental disabilities away from the criminal justice and correctional systems.
Collaborative solutions
295 In its October 2014 response to the Select Committee’s recommendation that a ministerial committee be established to consider services and supports for children and adults with developmental disabilities, the Ministry of Community and Social Services described its participation in a multi-ministry initiative with the Ministries of Health and Long-Term Care and the Attorney General, aimed at keeping people with mental illness and dual diagnosis out of the criminal justice system. A parliamentary assistant to the Minister of Community and Social Services has also been tasked with guiding and helping align the inter-ministerial work needed to implement the committee’s recommendations. In addition, the Ministry observed that, in collaboration with other ministries, it is leading a developmental disabilities education initiative for the justice sector, targeted for full implementation by fall 2016.[40] The objects of this project include:
- Identifying knowledge gaps regarding the intersections between developmental services and the justice system.
- Developing relevant strategies and providing information about existing resources to assist in diverting adults with developmental disabilities away from the justice system.
- Creating and implementing educational material to be shared with identified justice partners.
296 While these are positive developments, historically the Ministry’s participation in collaborative initiatives in the justice area has been remarkably lackluster. During our investigation, we reviewed the participation of Ministry representatives on various inter-ministerial committees. We discovered that committee involvement was often sporadic and generally did not result in any concrete action.
297 For instance, the Ministry takes part in the Provincial Human Services and Justice Coordinating Committee, formed in 1997. This committee is part of a provincial government strategy to co-ordinate services in the criminal justice system and gives priority consideration to people with a serious mental illness, developmental disability, acquired brain injury, drug and alcohol addiction, and/or fetal alcohol spectrum disorder. The Ministry of Health and Long-Term Care leads and funds the committee. There are 42 members, including representatives from the ministries of the Attorney General, Community and Social Services, Community Safety and Correctional Services, Children and Youth Services as well as Correctional Services Canada. There are also non-governmental stakeholder members – for instance, the Canadian Mental Health Association, which has 13 representatives. In addition, there are 14 regional committees and 37 local committees involved in this initiative. The main purpose of the regional and local committees is to provide a planning table to bring together service providers to find solutions to the problem of criminalization of people with defined unique needs and to develop a model of shared responsibility and accountability in dealing with this group of individuals at points of intersection with the justice system. The provincial committee’s objectives include supporting the regional and local efforts, issuing recommendations to address service and policy problems, and promoting consistency and sharing information across the province.
298 There is only one Ministry of Community and Social Services representative on the provincial committee – a senior policy analyst tasked with overseeing joint projects with the Ministry of Health and Long-Term Care. Ministry representation on regional and local committees is also limited. Over an 18-month period from February 2012 to September 2013, the provincial committee met nine times. A review of the minutes revealed that members discussed several key issues affecting individuals with developmental disabilities, including concerns that some who should have gone through court diversion were put through other streams. However, the Ministry of Community and Social Services representative was absent for five of the nine committee meetings, including ones where issues relating to adults with developmental disabilities within the criminal justice system were discussed.
299 Then there is the inter-ministerial mental health and justice directors’ working group, composed of representatives from the ministries of Health and Long-Term Care, Attorney General, Community Safety and Correctional Services, Children and Youth Services and Community and Social Services. This group held its first meeting on March 1, 2012. Its purpose is to identify and address current and emerging operational challenges in the interface of the mental health and justice systems involving persons with mental illness, who may have other co-occurring disorders, and are involved in the justice system. The group is intended to engage in co-operative problem solving and information sharing. The group develops annual work plans of initiatives to further its mandate. There are two director-level representatives from the Ministry of Community and Social Services in the group. However, only one of them attended two of the three meetings that took place in 2012.
300 In order to be effective, collaboration must be consistent and persistent. The Ministry should ensure that senior officials are assigned responsibility for leading discussions relating to the criminalization of individuals with developmental disabilities and that they take a proactive and robust approach to promoting reform in this area through inter-ministerial collaboration.
Recommendation 32
The Ministry of Community and Social Services should ensure that senior officials take a proactive and robust approach to inter-ministerial initiatives aimed at reducing potential for the criminalization of individuals with developmental disabilities and dual diagnosis.
Justice seen to be done
301 To bring greater transparency and accountability to inter-ministerial undertakings affecting the developmental services sector, the Ministry should post information publicly about details and results of its collaborative efforts to divert adults with developmental disabilities away from the justice system.
Recommendation 33
The Ministry of Community and Social Services should publicly post progress updates on initiatives and collaborative efforts relating to diverting adults with developmental disabilities from – and protecting them within – the justice system.
302 The Ministry has indicated that it is developing education materials for use in the justice sector. However, the Ministry should also engage in targeted outreach and education of officials in the justice and correctional systems to improve understanding of the nature of developmental disabilities and the developmental services system, and to encourage implementation of best practices for responding to individuals with developmental disabilities, based on the advice of subject experts.
Recommendation 34
The Ministry of Community and Social Services should engage in targeted outreach and education of officials in the justice and correctional systems to improve understanding of the nature of developmental disabilities and the developmental services system, and to encourage implementation of best practices for responding to individuals with developmental disabilities, based on the advice of subject experts.
Incarceration by the numbers
303 In 2014, the Select Committee recommended that data be obtained on the number of individuals with developmental disabilities or dual diagnosis who are incarcerated. The Ministry responded, noting that the Ministry of Children and Youth Services has an electronic system for case management for youth in conflict with the law and suggesting that it might be modified to record this specific information. The Ministry explained that in the interim, if information on developmental disabilities is requested, it could conduct a snapshot survey of the clients served through the youth justice services sector.
304 While these measures may help to provide improved information about the number of youths in the developmental sector in conflict with the law, aside from statistics, the Ministry should obtain details of individual cases to allow for co-ordinated planning for supports and services as youths transition into the adult system. The Ministry should consult with the Ministry of Children and Youth Services to ensure that individual cases are tracked and the outcomes identified and shared with it.
305 The Ministry should also expeditiously pursue system improvements that will enable it to gather more accurate and comprehensive statistical information on the number of adults with developmental disabilities who enter the criminal justice system – charged and/or incarcerated. This information should be used to plan for adequate services, including supervised residential placements within the community to act as safe havens for individuals with developmental disabilities when their only alternative is to languish in jail.
306 The Ministry should also actively consult with service providers, community groups and other relevant ministries such as the Ministries of the Attorney General, Children and Youth Services, Community Safety and Correctional Services, Education, and Health and Long-Term Care with a view to developing a co-ordinated system for gathering statistical and qualitative information to identify the number of individuals, and types of situations, which may require exceptional supports to minimize the risk of individuals requiring developmental services defaulting to the criminal justice system.
307 In addition to reviewing data about the rate of incarceration, the Ministry should pursue measures to promote information sharing across involved ministries. At present, while the criminal justice, corrections and developmental services sectors intersect there are no inter-ministerial protocols for information sharing. The Ministry should work with its ministerial partners to develop a fluid process for sharing information and facilitating resolutions of individual cases.
Recommendation 35
The Ministry of Community and Social Services should work with the Ministry of Children and Youth Services to ensure that it provides detailed case information about youths with developmental disabilities and dual diagnosis transitioning to the adult system, who have been involved with the youth justice system.
Recommendation 36
The Ministry of Community and Social Services should gather statistical information on the number of adults with developmental disabilities who enter the criminal justice and correctional systems, to help with planning to ensure there are adequate resources including supervised residential placements within the community as an alternative to incarceration.
Recommendation 37
The Ministry of Community and Social Services should consult with service providers, community groups and other relevant ministries – such as the Ministries of the Attorney General, Children and Youth Services, Community Safety and Correctional Services, Education, and Health and Long-Term Care – with a view to developing a co-ordinated system for gathering statistical and qualitative information to identify the number of individuals and types of situations that may require exceptional supports to minimize the risk of individuals who require developmental services defaulting to the criminal justice system.
Recommendation 38
The Ministry of Community and Social Services should work with the Ministries of the Attorney General and Community Safety and Correctional Services to develop an effective process for sharing information and facilitating resolutions of cases involving adults with developmental disabilities within the criminal justice and correctional systems.
Early identification and response
308 As the cases we reviewed illustrate, sometimes there are early indicators that an individual may be at risk of becoming embroiled in the criminal justice system. Impulse control issues and aggressive behaviours may escalate during life transitions or personal crisis points, but certain tendencies may be apparent long before an adult with developmental disabilities comes into contact with justice officials. There should be capacity in the developmental services system for early identification of and support for individuals at risk of becoming involved in the criminal justice system. The Ministry of Community and Social Services should work with the Ministries of Children and Youth Services, Education and Health and Long-Term Care to identify these individuals and develop intervention strategies to minimize their potential for incarceration. The Ministry should ensure these individuals have access to preventative programs and supports, including supervised residential placements, focused at avoiding entry into the criminal justice system.
Recommendation 39
The Ministry of Community and Social Services should work with other relevant ministries on a process for identifying and providing preventative supports for individuals at risk of becoming involved in the criminal justice system.
Registering awareness
309 Some police services have registries with information about vulnerable individuals, to ensure appropriate response in the event police intervention is required. However, this is not a universal practice. There is no consistency in how police services and justice officials respond to cases involving adults with developmental disabilities. In some situations, these individuals may be charged and incarcerated; in others, non-custodial and non-criminal alternatives may be pursued. The more information justice officials have about the individual circumstances and needs of adults with developmental disabilities, the less likelihood that the behaviours associated with their disabilities will lead to their incarceration. The Ministry should undertake research and consultation on development of a provincewide registry of vulnerable persons to assist police and other justice officials in responding appropriately to cases involving adults with developmental disabilities in crisis.
Recommendation 40
The Ministry of Community and Social Services should consult relevant stakeholders with a view to encouraging Developmental Services Ontario offices, service agencies and police services to work together to develop a provincewide vulnerable person registry to assist police and justice officials in responding to crisis involving adults with developmental disabilities.
Decriminalizing conduct
310 One of the reasons why some adults with developmental disabilities become homeless and at risk of incarceration is because their aggressive and threatening conduct is difficult for service providers to manage. Of the families who contacted us, 179 were living with violence in the home at the hands of their adult children with developmental disabilities, and 172 described that their loved ones displayed aggressive contact towards others. In 81 cases, self-harming conduct was a significant concern. According to the Ministry’s December 2014 survey results, of those receiving residential supports, up to 30% demonstrated aggression towards others, property and/or self.
311 Individuals with a history of aggressive behaviour are often repeatedly rejected for residential vacancies in favour of those who present fewer behavioural challenges and safety risks. In several cases we reviewed, crisis situations escalated and adults with developmental disabilities and dual diagnosis found themselves diverted to the justice system when service agencies could not cope with their conduct. We learned that some agencies routinely require their support workers to call 911 when an adult with a developmental disability becomes aggressive, threatening or assaultive with staff, although police and local hospitals are themselves ill-equipped to deal with these behaviours. According to a 2013 study, some 10% of crisis episodes involving police contact with individuals with developmental disabilities result in arrest. Arrests are more likely to occur when the individual has had prior interaction with police.[41]
312 The developmental services system should not be relying on police, who do not have any mandatory or consistent training on how to deal with individuals with developmental disabilities, to deal with behavioural crises. Calling the police should be a recourse of last resort, not an alternative to providing adequate supports to manage difficult behaviours.
313 In one case my staff helped resolve, a 63-year-old woman with developmental disabilities – who had previously been sent to a hospital psychiatric unit and specialized treatment centre because of her violent behaviour – was residing in a group home. Her family contacted our Office concerned because she was not receiving adequate supervision. She was frequently left alone in a basement apartment in her group home for several hours each day. In addition, she was sent home two weekends a month to be with her 90-year-old mother, who was partially blind. At one point, she was arrested and handcuffed by police for slapping the home’s executive director when she became agitated. Working with senior Ministry officials, we were able to facilitate additional resources being allocated to increase support for her, and her behaviour and well-being improved.
314 The reluctance of some service providers to support individuals with extreme behaviours is understandable, given legitimate concerns about the safety of staff and other residents. However, failure to provide sufficient care for this population increases the risk of criminalization of conduct that may be associated with some developmental disabilities and dual diagnosis.
315 There are four Community Networks of Specialized Care in Ontario. They are responsible for linking specialized services and professionals, to pool their expertise to treat and support adults who have developmental disabilities, mental health needs and/or challenging behaviours, in the communities where they live. The networks are led by transfer payment agencies under contract with the Ministry. They do not provide direct services but bring together people from a variety of sectors, including developmental services, health, research, education and justice – with the common goal of improving the co-ordination, access and quality of services for individuals who have complex needs. They also collaborate with Developmental Services Ontario offices in their catchment area on referrals, case resolution, crisis intervention and information sharing.
316 The Community Networks of Specialized Care have observed that without proper care, individuals with challenging behaviours “will increasingly be incarcerated, in shelters, or in forensic psychiatric facilities.”[42] In 2014-2015, the networks developed provincewide Guidelines for the Care, Support and Treatment of People with Developmental Disabilities and Challenging Behaviours, which were presented to the Ministry in May 2015. The networks have begun to engage agencies and implement the guidelines. These are intended to act as a resource manual, which will be followed by a training curriculum, tip sheets and best practice protocols for developmental service agencies to assist in supporting people with developmental disabilities and challenging behaviours.
317 The Southern Network of Specialized Care issued a document in June 2013 entitled Understanding Special Needs Offenders who have a Dual Diagnosis, including tips for correctional officers on serving the dual diagnosis population. However, there are no similar provincial educational resources for correctional and justice officials on dealing with adults with developmental disabilities and dual diagnosis.
318 This work towards developing standards of care based on best practices is a positive initiative. However, the Ministry should ensure that clear, consistent guidance and protocols are developed around the appropriate response to physical aggression by adults with developmental disabilities, which serve to balance the need to protect developmental services staff from harm, but avoid criminalizing behaviours of individuals whose ability to curb aggressive or maladaptive impulses may be severely compromised as a result of their disabilities.
319 The Ministry should also continue to support development and implementation of best practice standards. In addition, it should ensure that correctional and justice sector partners are included in consultation and training relating to these standards.
Recommendation 41
The Ministry of Community and Social Services should continue to support the development, based on best practices, of guidelines and protocols for responding to physical aggression by adults with developmental disabilities, balancing the need to protect clients and staff with the goal of avoiding criminalization of those with developmental disabilities.
Recommendation 42
The Ministry of Community and Social Services should engage in consultation and outreach with justice officials, including police services, correctional officials, Crown prosecutors and the judiciary, relating to best practices for addressing the needs of individuals with challenging behaviours.
The More We Get Together: Lack of Co-ordination in Medically Fragile Cases
320 We received 148 complaints about situations involving individuals with developmental disabilities who were also coping with a host of complex medical conditions. These “medically fragile” cases present one of the greatest challenges for the developmental services sector, and require creative and inter-ministerial solutions. Historically, there have been few signs that the Ministries of Health and Long-Term Care and Community and Social Services were prepared to invest the time and energy to co-ordinate resolutions in such cases.
321 Developmental services agencies have typically avoided taking on these high-needs cases, as they do not have the medical expertise, training and resources to handle them. On the other hand, long-term care homes may be able to meet the medical requirements in some cases, but they do not have the staffing, programing and supports required to address developmental needs.
Finding a proper fit: Stella’s story (West Region)
322 Stella is 20 years old. Since birth, she has had a brain stem dysfunction, which has significantly affected all aspects of her life. She is non-verbal, incontinent, and unable to move her limbs. She has many medical conditions, including spastic quadriplegia, epilepsy, and compromised vision and hearing. She uses a wheelchair and is dependent on a G-tube for feeding and tracheostomy tube for breathing. Stella requires one-to-one supervision on a 24-7 basis, as her mouth must be constantly suctioned or she risks sudden death. Stella communicates using a device attached to her head that she uses to push buttons to indicate what she wants; for instance, to listen to music. Stella lives with her mother, father and older twin brothers on their farm in rural southwestern Ontario.
323 Stella’s parents have devoted their lives to caring for her and meeting her complex needs in the home. However, as they aged and her mother faced her own health problems, they realized they could no longer satisfy the significant demands of Stella’s multiple disabilities in their home. In 2007, her parents requested individualized funding to allow Stella to move to a residential facility. The funds did not materialize and her name was placed on a waitlist for a group home. Two years later, Stella’s parents tried another approach. They requested funding from the Ministries of Children and Youth Services, Community and Social Services, and Health and Long-Term Care for additional supports to enable Stella to continue to live at home. After this too failed, in 2010, Stella’s family submitted a planning proposal, which would involve purchasing a home for Stella. Nothing came of this attempt and Stella’s parents were forced to look to local service agencies in the hope of finding her a permanent home in the community.
324 Unfortunately, there is no integrated system of residential supports for adults with developmental disabilities and complex medical problems. Finding an existing community placement for medically fragile individuals within the developmental services sector is extremely challenging. In Stella’s case, the situation is complicated by the fact her family lives in a rural setting. One vacancy did come up in 2011 with a local service provider, but it was unsuitable because Stella’s specialized medical equipment would not even fit into the room.
325 Before Stella turned 18, her family services case worker applied to the Ministry requesting $47,000 in annualized transitional funding to ease her move to the adult system. The Ministry responded that there was no funding available. Concerned about diminishing resources and the uncertainty surrounding Stella’s future care, her family contacted our Office in May 2013. We made inquiries to determine the status of attempts to find Stella a home in the community. It was apparent that the developmental services sector was having difficulty meeting Stella’s needs. In August 2013, we learned that another community placement had been assessed as inappropriate to accommodate Stella’s specialized equipment.
326 Once Stella turned 18 in August 2013, her access to children’s respite services ended. Previously, Stella received one week of respite services every month during the school year. As an adult, she was initially provided with six hours a week of respite by a local agency, but this was later reduced to three hours a week. She also received daily nursing assistance through the Community Care Access Centre. However, Stella’s family was stretched to the limit to provide the 24-hour care she required. Although they received three months of flex funding in August 2013 and in January 2014, and the Ministry approved some additional funds, there was no predictable and stable funding to purchase supports. The situation continued to take its toll on Stella’s parents, who had to fill in the gaps in the schedule of care. Given the lack of success in finding Stella a placement in the developmental services sector, her name was also placed on a waitlist for a respite bed at a facility funded by the Ministry of Health and Long-Term Care.
327 By February 2014, Stella was the top priority in the region for residential services and Ministry officials considered approaching the Ministry of Health and Long-Term Care to work out a joint solution. One developmental services agency had a vacancy, but indicated that it would require additional funding to meet Stella’s high medical needs. In April, the Ministry began discussions with the local Community Care Access Centre, which was prepared to commit to seven hours of nursing a day, to assist the agency in caring for Stella. However, the agency’s proposal was rejected. A local Community Care Access Centre official, upon learning this news, observed dejectedly:
This is unbelievably disappointing and heartbreaking as I am witnessing a family that is eventually going to collapse under this pressure.
328 As far as the Ministry of Community and Social Services officials were concerned, they had done what they could, and it was up to the health care system to resolve the situation. As one official noted in an email on May 30, 2014, “At this time more steps need to be taken to push the health system.”
329 Stella remained at home for many months, receiving seven hours a day of Community Care Access Centre nursing care, as well as some respite nursing care from a local respite network. In July 2014, a vacancy was identified and on December 30, 2014, she finally moved into a residence with medical and developmental services supports, where we understand she continues to do well.
Fragmented funding: Steven’s story (North Region)
330 Steven is 25 and lives in Northern Ontario with his family. He has a severe developmental disability, epilepsy, cerebral palsy and cortical blindness. He understands words, but is non-verbal. He requires a G-tube for feeding, is incontinent and uses a wheelchair. Steven cannot swallow properly and requires suctioning. His head must remain elevated throughout the day and night. He takes multiple medications and is dependent on others for all aspects of his care.
331 Steven’s family is devoted to caring for him at home, where they believe he is happiest and healthiest. They are concerned that a residential placement would not be able to handle his high needs. However, there are insufficient supports in the north to accommodate Steven’s medical fragility and adequately support him in the home. Unlike large urban centres, the area where Steven lives has no agencies funded by both the Ministries of Community and Social Services and Health and Long-Term Care to serve the complex needs of individuals with both developmental and medical disabilities. Since he became an adult, Steven’s family has been left to rely on short-term solutions and temporary funding. Steven’s name was placed on waitlists for longer-term supports, but in the meantime his family has been forced to deplete their limited financial resources to supplement his care.
332 The funding rules within the developmental services sector have restricted Steven’s ability to access resources. In October 2012, the local case resolution committee granted some flex funding to his family, but by December the money was gone and a second request was denied on the basis that what he required was a long-term funding solution, outside of the committee’s mandate to grant. On December 14, 2012, Steven’s adult protective support worker, concerned about the impact of the denial on his family, appealed the decision, noting:
Clearly, the community supports in place to date have been insufficient to prevent the imminent family breakdown that results in safety concerns for both [Steven] and his family. The family is acutely aware of [his] intense complex needs and have been advocating within all ministries to provide a stable future for their son. …
[Steven’s] continuous reliance on temporary crisis funds to remain in his family home with limited access to the community is burning out his parents. … There have been cost comparisons completed to determine what someone with [his] needs would cost an agency-funded residential placement and as a community we will never find a better bargain.
333 The committee responded to the appeal on January 4, 2013 with a familiar refrain:
… the committee determined the needs of this family are for a long-term solution that falls outside the mandate of Case Resolution. Our committee understands that long-term resources do not exist for all the needs of all adults who are eligible for Developmental Services. However, the committee is not able to approve funding from Case Resolution to meet the needs of families who are waiting on waitlists.
334 In June 2013, when another funding proposal was made to the case resolution committee, Steven’s case managers stated:
His parents have exhausted all funding, due to not enough funding to accommodate his needs. Family breakdown will be imminent. Emotional stress is a concern. Again all the planning and assessing seem to be completed, the lack of resources are the obstacle in this case.
335 This request was also denied because it was seen as an attempt to use emergency funding to circumvent the waitlist for other supports. In February 2013, an agency suggested an innovative residential model for Steven’s care, but this proposal also languished.
336 Steven’s family received fragmented funding and supports from different sources, until August 2013, when he was granted Passport funding. He continues to live at home with his family, waiting for a residential placement.
Finding practical solutions to complex cases
337 Adults with a combination of developmental disabilities and complex medical conditions require intense and specialized services and supports across various sectors, including the health care and developmental services systems. The transition into adulthood is particularly difficult for these individuals, as children’s services disappear, and their caregivers are progressively challenged to meet their medical and developmental needs as they themselves age. When it comes to the quality of everyday living experienced by these individuals as adults, the Ministry of Community and Social Services should take the lead in ensuring there are adequate supports and services available.
338 As noted above, the Ministries of Children and Youth Services, Education and Community and Social Services now engage in planning for individuals with developmental disabilities to transition from the child to adult services system. However, in the case of those with medically fragile conditions, the Ministry of Health and Long-Term Care needs to be a partner at the planning table. The Ministry should ensure that the Ministry of Health and Long-Term Care is involved in transition planning for these individuals, and that adequate resources are secured to ensure a suitable medical and community supports are organized well in advance.
Recommendation 43
The Ministry of Community and Social Services should engage the Ministry of Health and Long-Term Care in the multi-ministry planning process in medically complex cases to ensure appropriate specialized medical and community resources are available as they transition into the adult system.
Remote problems
339 In its July 2014 report, the Select Committee made some recommendations addressed at remote and northern communities, which historically have had fewer day, respite and residential programs. Some of the critical cases that we reviewed, including those of Steven and Stella, involved individuals living in rural or northern communities where often, even with funding, there are simply no services or supports available. The Ministry does permit individuals to request services in multiple regions through their local Developmental Services Ontario office, although it acknowledges that this rarely occurs. Typically, regions prioritize their resources for those who reside there. While this generally makes sense, sharing of resources with those in rural and remote communities is a practical option. The Ministry should ensure that Developmental Services Ontario offices in remote and underserviced areas actively initiate consultations with other regions when a lack of supports and services is contributing to crisis situations.
Recommendation 44
The Ministry of Community and Social Services should ensure that Developmental Services Ontario offices actively pursue opportunities for sharing of resources across geographical boundaries to ensure that the urgent needs of individuals in underserviced areas are adequately met.
The Last Resort: Family Abandonment
340 Several families have become so desperate waiting for services for their adult children with developmental disabilities that they have relinquished responsibility for them to the community. They have typically done so by refusing to take them home from respite placements, day programs, hospitals – and, in at least one case, parents dropped their son off at the local Developmental Services Ontario office. Nine families told us they left their adult children in the care of agencies, and 21 others told us they left them in hospital, because they could no longer care for them without adequate services and supports.
341 On January 31, 2014, the Ministry’s regional office in Ottawa observed in an information note that between February 2013 and January 2014, there were eight cases where families relinquished care of their adult relatives with developmental disabilities and two cases where families indicated that they were seriously considering this step.
342 We were also contacted about 122 individuals whose caregivers were aged, sick or had recently died, leaving many facing homelessness. A few of these families went to the media with their stories. When Cindy Gibson made her case in the media in 2014, she was dying of cancer and frantic to find a stable home for her 26-year-old daughter Sherisse, who is developmentally disabled and functions at about the level of a five-year-old. While Cindy lay on her deathbed, friends and respite workers cared for Sherisse until a placement was finally found for her in a group home. Family friends later attributed the success in finding a home for Sherisse to the publicity focused on her plight.[43]
343 Local urgent response processes are unable to consistently meet the needs of individuals in crisis, including those on the brink of abandoning their adult children with developmental disabilities. The sheer volume of demand for developmental services is beyond the system’s ability to cope. For instance, the Ministry told us that in the Eastern region as of April 2013, there were 103 individuals classified at the highest priority level who were waiting for services and supports – and at least 30 of those were “urgent-urgent” cases. In total, there were 1,117 individuals waiting for a residential placement in that region. In July 2015, we learned that the Central East region was seeking placements for nine adults with developmental disabilities who no longer had caregivers able to support them at home and were effectively homeless.
A desperate choice: Serge’s story (East Region)
344 Serge’s parents are quite open about the heart-wrenching decision they made to leave their then 19-year-old son at the Developmental Services Ontario office in Ottawa on April 30, 2013. At over six feet tall and 215 pounds, Serge has multiple diagnoses, including autism and profound developmental delay. He is non-verbal, with cognitive functioning at the level of a two-year-old. Serge’s care is further complicated by the fact that he lives with diabetes and requires insulin.
345 Serge displays self-injuring behaviours and he has a history of causing significant property damage. He can also be intimidating. He will threaten to hit people, although he rarely follows through. When he became an adult, Serge’s parents experienced greater difficulty managing his behaviour, particularly since Serge is a “runner.” He fled his parents’ home multiple times, necessitating police assistance.
346 Caring for Serge has taken immense toll on the family. His parents and younger sister have all suffered health problems as a result. In May 2011, a Dual Diagnosis Consultation Outreach Team assessment noted, “the family’s score on the Family Burden Assessment Scale was one of the highest we have seen.” In August 2011, the family connected with the local Developmental Services Ontario office, looking for additional supports. They were particularly concerned about decreasing access to respite services because of Serge’s diabetes. Several service agencies refused to provide respite because their staff were not trained to administer insulin. During a nine-month period, the family only obtained four days of respite relief. In December 2012, a hospital initially indicated it could take Serge for 10 days, but then reneged. Later, another respite placement called his parents after only four hours to come pick him up when staff found they could not handle his behaviour.
347 Serge’s mother spent considerable time contacting officials in search of help and became increasingly frustrated by the lack of response. By January 2013, she told us she was encouraged to learn that Serge was assessed as a level 1 priority for residential and other supports. But her hope was short-lived, as the months went by without a placement.
348 In the meantime, the home situation became progressively more desperate. In March 2013, Serge’s mother was terrified when, as she was driving on the highway at 100 kilometres an hour, Serge impulsively opened a car door, took his seatbelt off, and reached out to shut it. Serge’s aggression was also escalating. On April 12, 2013, his mother wrote to the Ministry, urging officials to assist in finding Serge a group home placement:
We have been following the rules for years. We need a placement now, or else our son will end up homeless in a crisis. We are not able to care for him any longer. I am on sick leave from work as I am unable to function anymore. PLEASE HELP.
349 Some two weeks later, Serge wandered from home and crossed a busy intersection. Two days after that, he required hospital care after swallowing prescription medication. When he came home, he bolted from the car, leading to a 911 call for assistance. This series of events left the family at the end of their endurance. They realized they could no longer keep Serge safe at home. He had been on a waiting list for a residential placement for over a year, and the family felt they had run out of options.
350 On April 30 at 8:40 a.m., Serge’s mother left him at the local Developmental Services Ontario office with a two-page letter explaining the situation and asking that adequate housing be provided to him. She told us:
Truth be known, when I was on my way down there I really wasn’t sure if I was going to do it. Even when I was in the DSO office, I really wasn’t sure if I was going to do it… I just left him. I had eye contact with somebody at reception … and I didn’t say anything to her. I just told [Serge] I loved him, gave him a high five and told him that he was going to go to camp, because going to respite or group homes for him, he understands it’s like going to summer camp. And he was fine. He was happy.
351 The family’s decision to relinquish care of Serge set off a chain of events as the urgent response process was activated. The police became involved – helping to keep Serge safe, meeting with his mother to obtain information, and getting a prescription for his insulin from the family doctor. A serious occurrence report was sent to the Ministry by local developmental services officials and within a few hours, senior Ministry officials were alerted to the situation. A service provider was located that was prepared to provide temporary housing and the local Community Care Access Centre committed to providing nursing care to administer Serge’s insulin injections.
352 While the family obtained some relief through abandoning Serge to the system, the system was unable to easily accommodate his needs. Over the next 16 months, Serge was shuffled through a series of temporary placements within the region. In the absence of a provincewide mechanism to find alternatives, officials relied on the vacancies identified by local agencies. Contingency planning included options outside of the developmental services sector, such as domiciliary hostels, hospitals and emergency shelters, with additional staffing supports. Officials also tried to persuade the family at various points to take Serge home again with promises of funded supports and respite in the home. However, while the offer of additional assistance in the home might have worked in 2011, when the family first looked for help, they could no longer cope with the prospect of Serge returning to their care. They held out hope for a permanent housing solution for him. It was not until August 2014 that Serge finally moved to a permanent community placement with an annualized budget of $124,899. The Ministry told us Serge is now doing extremely well and participating in a community business and a recreational day program.
Life after death: Cindy’s story (East Region)
353 Cindy is 41, with a dual diagnosis of autism spectrum disorder and obsessive compulsive disorder. She functions at the cognitive level of a 5-7-year-old. Cindy’s mother cared for her at home for decades. However, her mother’s health began to decline and by 2004 she requested that Cindy be placed on the list for residential care. Cindy was still waiting for a community placement seven years later when she began the intake process for Developmental Services Ontario in 2011. In the fall of 2012, Cindy’s mother became progressively concerned about her ability to care for her, and began desperately calling around, searching out services for her daughter.
354 Tragically, on November 13, 2012, Cindy’s mother died, leaving Cindy facing the prospect of living in a homeless shelter. To avoid this fate, her aunt and uncle, both seniors, agreed to take Cindy in on the understanding that this was a temporary stopgap measure. The case had been flagged as urgent when Cindy’s mother died. Cindy was on the Developmental Services Ontario office’s registry as top priority for housing in a group home setting and considered most in need to access a funded vacancy. But three months later, when her aunt contacted our Office, Cindy was still awaiting a community placement. Cindy was able to attend some day programming, but she needed a permanent home.
355 On May 14, 2013, the situation declined rapidly when Cindy’s uncle was diagnosed with terminal cancer and hospitalized. When we contacted the Ministry the next day about the status of attempts to find Cindy a placement, we learned that despite being flagged as urgent months earlier, Cindy’s case had somehow been overlooked and had not been presented at the local prioritization table. Ministry records reflect that the same day, service agency officials alerted it to the possibility that Cindy’s aunt might abandon her, as she could not care for both her husband and her niece. A Ministry “contentious issues report” was issued to senior officials, who began to monitor the situation.
356 On May 25, Cindy’s uncle died. Despondent, her aunt inquired about the availability of respite through the Community Care Access Centre. She was told that this was not an option, since a caregiver must be hospitalized to qualify for this service. Throughout June 2013, Cindy’s aunt struggled with her grief, and worried that the stress of her circumstances would send her relapsing into depression. An attempt at out-of-home respite on June 25 was unsuccessful, as Cindy returned in the middle of the night after experiencing massive anxiety. Poor information management and communication amongst Developmental Services Ontario and service agency officials around what Cindy’s aunt was requesting for respite compounded the problem. Cindy’s aunt had difficulty understanding the system, the roles of different agencies, and what services were available, as well as communicating her needs effectively to appropriate officials. At times her voice simply went unheard. For instance, on June 28, Cindy’s aunt sent an email to a service agency renewing a request for respite to allow her a chance to visit her daughter in August. But an official later told our Office the agency had no respite request on file.
357 By July 2, bewildered and unable to cope, Cindy’s aunt wrote to the agency, copying our Office and Developmental Services Ontario, stating: “I give up. Make [Cindy] a ward of the state or something. Deal with it yourself. I will be leaving at the end of July.” She then dropped Cindy off at an elderly neighbour’s home, and went to the hospital, exhausted and desperate. She returned home later that evening.
358 After her aunt’s hospital visit and repeated attempts by Ombudsman staff to prompt the Ministry into action, Cindy received flex funding for in-home support for four days in early July. However, throughout that month, her aunt suffered periodic panic attacks. Eventually, an out-of-home respite placement was arranged for the month of August. The placement was in a “home share”, where Cindy could live with a family, while her aunt visited her own daughter in Quebec.
359 Finally, after more than eight months of dealing with her niece’s high needs, her husband’s illness and death, and her own medical problems, Cindy’s aunt could no longer care for her. On August 26, 2013, following her doctor’s and therapist’s advice, Cindy’s aunt wrote agency officials and explained that she would not be taking her back. She observed that in the respite placement Cindy had regained her cheerfulness and had blossomed “in a family atmosphere that I cannot provide her.” The next day, another Ministry contentious issues report flagged this and three other “abandonment” cases, noting:
The Case Management agency and participants in urgent response process are indicating that the ability of the region to deal with these cases is significantly compromised at this point by the number of recent abandonment cases in the Eastern Region.
360 Discussions amongst officials proceeded in September. Cindy was able to resume day programming and remain in the respite home on a temporary basis. On September 27, 2013, Developmental Services Ontario officials told our Office that the home share where Cindy was living had a vacancy, which was being put through the matching process. Cindy was accepted into the vacancy, and has since continued to benefit from the home-share arrangement.
A tale of two cities: Kyle’s story (Toronto and West Regions)
361 One factor that may contribute to situations involving abandonment is the transition to adulthood in the developmental services sector. At age 18, adults with developmental disabilities lose funding for and access to children’s services, and then at age 21, they are no longer eligible for publicly funded secondary school services. Financial and programming challenges during this period are often accompanied by marked behavioural changes. Some caregivers told us that their adult children experienced more aggression and impulsivity in late adolescence. In eight cases, parents told us that they had to give up their jobs to look after adult children who had finished school and had no day supports.
362 While multi-ministerial transition planning, which began in 2013, is a welcome development, the unfortunate reality is that planning is only effective if it leads to securing adequate supports and services. All too often, adults with developmental disabilities end up stuck on interminable waitlists. The gap between need and availability of resources is profound and a symptom of a system in crisis. This is all too clear in the case of families who, because of illness, death of a caregiver, age or exhaustion, are no longer able to cope with the demands of caring for an adult with developmental disabilities and feel they have no options other than abandonment. For instance, Kyle and his father were deeply impacted by his transition to the adult system.
363 Kyle lives with moderate to severe autism with developmental delay as well as mental health challenges. He is non-verbal, but can communicate using about 20 sign language signs. At times, Kyle can become extremely aggressive.
364 Kyle’s parents are divorced, and when he was 14 he moved in with his father, who works full-time outside of the home. Kyle’s father has exerted considerable effort to balance his work responsibilities with Kyle’s needs. For years he managed quite well with Kyle attending school full-time and receiving daily 1:1 support in the home after school. Kyle and his father lived in an apartment in Toronto during the week and spent weekends in St. Catharines at the family home. As a child, Kyle was able to access children’s services in the Niagara area while also receiving respite and other supports when resident in Toronto. However, soon after Kyle turned 18, difficulties in arranging adult services and a spike in his aggressive behaviour sent the family spiraling into crisis.
365 His father soon discovered that there was confusion about whether Kyle would be eligible for adult developmental services in two separate regions. In April 2012, he was told that he would have to look to the Toronto Developmental Services Ontario office for assistance. However, in October he was told that services across regions could be arranged. While this was welcome news, in reality it meant that Kyle’s name was simply added to waiting lists for respite services in both regions.
366 Although Kyle was still receiving some supports, soon these were insufficient to meet his escalating needs. In fall 2012, Kyle became increasingly aggressive, and in late December, he broke his father’s wrist and was suspended from school. On January 24, 2013, when Kyle was attending respite outside of the home, he became so uncontrollable that police were called, and it took eight officers to restrain him. After a brief admission to a mental health centre and an emergency treatment bed, Kyle was released home. He was provided with two workers to support him and later resumed school part-time. However, the situation continued to deteriorate, with Kyle having to be frequently medicated to control his behaviour and the school repeatedly calling police whenever he became aggressive. Eventually, Kyle was diagnosed as eligible for dual diagnosis resources and in-patient treatment and a medication review were recommended. His name was added to a waitlist for treatment beds.
367 In early March 2013, Kyle was formally suspended from school. Over the course of the next few months he was involved in a series of incidents involving injury to others and was hospitalized three times. Back at home in May, he was supported initially by two support workers, then later by one, as well as some respite services. The plan was for Kyle to attend some summer camps in July and August and go back to school in September.
368 Kyle’s behaviour worsened again when he was at camp in July and he was readmitted to the mental health centre. Frustrated by the roller coaster of violent outbursts and hospitalizations as well as inconsistent supports, Kyle’s father signalled to the local Developmental Services Ontario authorities that he would not pick his son up if the centre discharged him. Despite this pronouncement, Kyle’s father did take him home when he was released at the end of July, on the understanding that Kyle would attend summer camp in August. However, Kyle’s return to camp did not go well. He injured three other campers as well as a worker, and had to be frequently sedated and placed in seclusion. On August 15, he was readmitted to the mental health centre. The next day, he was moved to the centre’s dual diagnosis unit. During his stay at the centre, Kyle continued to engage in violent outbursts, requiring sedation and isolation.
369 By the summer of 2013, Kyle’s father had accepted the reality that he could no longer care for his son at home. Kyle was waitlisted for a permanent community placement and day program. His father also explained to hospital and Developmental Services Ontario officials that he would not take Kyle back home unless a satisfactory discharge plan was developed. Under the circumstances, the case was flagged as an abandonment situation and Kyle’s status changed to “homeless.” However, once again, in September, Kyle was discharged and returned home to live with his father. This time, he had a support worker with him in the home and the plan was for him to return to school (half days) in October. But the episodic cycle of aggressive behaviour continued and by October 21, another incident at the school led to further police intervention, followed by another suspension. At home all day in the apartment with two support workers, Kyle continued to act out, destroy property and engage in harmful conduct. On November 12, Kyle threw a tantrum, bit a worker, and did considerable damage to the apartment. He ended up at a hospital emergency department that day, and his father brought him to the mental health centre the next morning, declaring that after years of trying to care for his son without adequate supports, he would not be taking him back home. The community service agency that had supplied workers in the home also indicated that it would not provide services past November 30.
370 Given his homeless status and extreme behaviourial volatility, Kyle was identified as fourth in line for priority funding, made available through an additional provincewide investment of $42.5 million in developmental services. Initially, this priority funding was only allocated for three individuals in the region. Ombudsman staff alerted senior Ministry officials to this situation, and as a result, an additional three individuals, including Kyle, eventually received supports.
371 In mid-February 2014, Kyle finally moved to a group home placement in the community, with an annualized budget of $174,000. The staff working with Kyle received crisis prevention training to help prevent injury and burnout. Kyle continues to require significant staffing and behavioural supports.
372 Kyle’s father is left to wonder if the cycle of violence and repeated hospitalizations could have been averted had ready access been available to additional in-home, respite, treatment and residential supports.
Breaking the abandonment cycle
373 Cases of abandonment place extreme pressure on the already overburdened developmental services sector. When a family takes the exceptional step of relinquishing responsibility for a loved one’s care, it has a cascading affect throughout the system. Providing relief in relinquishment situations means further delaying placements for other individuals, who were prioritized for services. One case manager told us that while she understood that a particular abandonment situation was desperate and the individual would get the supports he needed, she had 12 people on her caseload with the same level of need and she knew colleagues who did as well.
374 Abandonment scenarios have sent the system scrambling to locate placements. For instance, the Ministry’s regional office in Ottawa relied on flexible funds, although these were not temporary or short-term situations. Several officials who spoke to us blamed families who abandoned their children for jumping the queue. A Ministry contentious issue report of November 4, 2013 warned:
As a result of abandonment cases, some individuals who were not considered to be the most in need are being prioritized as urgent. This has an impact on the perception that individuals who are abandoned will jump the queue for services.
375 Instead of casting aspersions on distraught parents who feel they have no recourse other than to relinquish custody and care of their loved ones, the Ministry should be engaging in more proactive and early intervention to prevent situations devolving into crisis. In addition to keeping track of abandonment cases as the Select Committee recommended, the Ministry should analyze the root causes of abandonment and establish procedures to mitigate the risk of similar situations arising in future.
Recommendation 45
The Ministry of Community and Social Services should analyze cases of abandonment to identify root causes and develop ameliorative measures to reduce the risk of abandonment in future.
Warning signs
376 In many of the cases we reviewed, abandonment and homelessness were not surprise events, but the predicable result of caregivers burning out because of chronic stress and lack of adequate resources. In some cases, multiple cries for help went unheeded as officials ignored the threat of homelessness. The Ministry does receive some serious occurrence and other reports highlighting abandonment cases. However, it should expand its occurrence reporting system to ensure that Developmental Services Ontario offices and service agencies warn it at the earliest opportunity of cases where there is a substantial risk of relinquishment or homelessness.
377 In some situations, providing additional supports in a timely manner can make all the difference and ward off homelessness and abandonment. In others, circumstances beyond the caregivers’ control may lead to an urgent and unexpected need for services. The Ministry should also ensure that adequate resources are available, both to minimize the chance that homelessness and abandonment will occur and to provide supports when they do.
Recommendation 46
The Ministry of Community and Social Services should add a requirement to its occurrence reporting system so that cases in which there is a substantial risk of abandonment or homelessness are reported to the Ministry and appropriately addressed.
Recommendation 47
The Ministry of Community and Social Services should ensure that sufficient resources are available to address situations or significant risks of abandonment or homelessness.
Regional co-ordination
378 In Kyle’s case, had there been greater co-ordination between the two regions involved, the risk of relinquishment might have been reduced. His situation illustrates the lack of clarity around the availability of developmental supports across regions. It took months for officials to sort out whether Kyle was eligible for services in two different jurisdictions. After our Office became involved, the Ministry clarified that Developmental Services Ontario offices can refer individuals for services in other regions. However, there is no specific or clear direction on co-ordinating services or resources amongst regions beyond the initial application process. The Ministry should provide concrete guidance for regional offices and Developmental Services Ontario officials concerning co-operating and co-ordinating services to meet the needs of clients who straddle different service areas.
Recommendation 48
The Ministry of Community and Social Services should provide clear direction to its regional offices and Developmental Services Ontario officials about co-ordinating services to meet the needs of clients who reside in and/or receive services from more than one jurisdiction.
Proper planning
379 Relinquishment situations commonly arise because of life events; an individual’s behaviour suddenly escalates with maturity; a caregiver becomes physically ill or dies. The developmental services system needs to be sufficiently nimble to effectively respond to these cases. Life is unpredictable, but a certain number of crises of this nature should be anticipated and factored into Ministry planning for the developmental services sector. Historically, the Ministry has had limited information about the profiles of those requiring developmental services and no practical ability to engage in proactive contingency planning. To remedy this situation, the Ministry should work closely with the Ministries of Children and Youth Services, Education and Health and Long-Term Care, as well as Developmental Services Ontario offices and service agencies, to obtain sufficient information about individual cases and crisis events to enable it to project future service needs. It should also engage subject experts to evaluate this information and generate statistical probabilities of crises arising as a result of aging, illness and death of caregivers, and other life events. These predictions should then be employed in system planning for developmental services.
Recommendation 49
The Ministry of Community and Social Services should work closely with the Ministry of Children and Youth Services, Ministry of Education, Ministry of Health and Long-Term Care, Developmental Services Ontario offices and service agencies to track individual cases and crisis events in the developmental services sector.
Recommendation 50
The Ministry of Community and Social Services should engage subject experts to advise on the likelihood and rate of life crises in the developmental services sector and use these projections in system planning.
For the record
380 We also discovered that in Cindy’s case, Developmental Services Ontario had not kept records of communications with her mother and later her aunt. This led to confusion as to what services they had requested and how they had responded to offers of resources. The Ministry should direct that Developmental Services Ontario officers and service agencies put record-keeping practices in place, requiring that all contacts be recorded.
Recommendation 51
The Ministry of Community and Social Services should direct Developmental Services Ontario, service co-ordination offices and agencies providing developmental services to adopt record-keeping practices requiring that contacts with families, the Ministry and other agencies be properly documented.
Mismatching Game
381 Many families expressed frustration to us about the process for matching individuals with residential resources. Some complained that adults with developmental disabilities were considered for residential vacancies that were clearly a mismatch. Although this step did not result in any lost opportunities for the families in question, it was a wasteful and unnecessary exercise that led in some instances to false hopes of securing a placement. While Tommy and Riley were hospitalized, they were both identified for placements in the community that were glaringly inappropriate. Kyle was referred twice to the same unsuitable placement within a five-month period. However, one of the most extreme examples of mismatching we came across involved a 21-year-old woman with a rare genetic syndrome who is four feet tall, non-verbal, totally dependent for her physical care, and functions at the cognitive level of a six-year-old. In February 2013, the local Developmental Services Ontario office matched her to a vacancy in a group home for elderly men, including one resident who was known to be aggressive. This was an absurd referral and predictably the service agency rejected her. She was eventually matched to a suitable vacancy in July 2013.
Going through the motions
382 One Developmental Services Ontario manager acknowledged to us that individuals are sometimes matched to inappropriate placements to demonstrate that attempts have been made to place them. As she put it: “We’re going through the motions to ensure that the highest priority person is considered.”
383 The Ministry recently told us that its Developmental Services Consolidated Information System (DSCIS) will soon require that service agencies declare vacancies using a shared online resource. Once a vacancy is identified, the local Developmental Services Ontario office will be responsible for matching candidates to the vacancy, based on detailed candidate information already stored in DSCIS.
384 It is ridiculous and adds insult to injury to refer individuals in desperate need of residential supports to vacancies that are obviously a poor fit. While improvements to the DSCIS may ensure that more standardized information is available and applied for the matching process, the Ministry should provide guidance to Developmental Services Ontario offices to ensure that they exercise common sense when matching individuals to vacancies, and only make referrals where there is a realistic prospect of a match with the individual in need – including with appropriate adaptations.
Recommendation 52
The Ministry of Community and Social Services should provide direction to Developmental Services Ontario offices to ensure that individuals are matched to vacancies only where there is a realistic prospect of an appropriate fit.
Reasons for rejection
385 We heard many complaints from families who were given no reasons to explain why a particular individual was rejected for a placement. Ultimately, service agencies have the final say on whether they will accept an applicant for a declared vacancy, as they own and operate the programs and facilities and are legally responsible to their clients and staff. For service agencies, “fit” with their existing clients and service structure is key to accepting applicants for placements.
386 Families are often left without any clear explanation for why their loved ones have been rejected. Although agencies are expected to provide a reason, many will simply respond, “not suitable.” There should be greater transparency and a consistent requirement that service agencies provide detailed reasons for rejecting applicants.
387 The Ministry told us that when the modifications to DSCIS relating to matching are complete, once a decision is made regarding the suitability of the vacancy for an individual, the service agency will be required to report back to the Developmental Services Ontario office using the shared online resource. The service agency must select a reason from a standard menu to explain why a service agency has declined a placement. These reasons may include age restrictions, environmental factors (physical space, allergies, safety issues), high behavioural and/or medical needs, and insufficient supports available to meet client needs. The Ministry advised that it would monitor this information for frequency of rejection of candidates and the types of reasons given for turning applicants down. There are no detailed reporting requirements yet, as the process is still in development and at the pilot phase.
388 At a minimum, the Ministry should ensure that service agencies provide a detailed explanation to the Developmental Services Ontario office, as well as the affected individual and family, of the reasons for rejecting applicants for placements who are in crisis situations and/or have complex needs.
Recommendation 53
The Ministry of Community and Social Services should ensure that service agencies provide detailed explanations for rejecting applicants for residential vacancies who are in crisis situations and/or have complex needs.
Finding a fit
389 In its July 2014 report, the Select Committee observed that housing for adults with developmental disabilities is one of the most critical issues it addressed. It made several recommendations to address this issue, including that the Ministry of Community and Social Services explore innovative, individualized, affordable and flexible family- and community-led housing solutions.
390 The government’s 2014 budget investment in developmental services is intended to provide residential support for approximately 1,400 people with urgent needs. In 2014, the Ministry also struck a Developmental Services Housing Task Force to find innovative housing solutions. It held its first meeting September 22, 2014. The task force brings together individuals and families, municipal and community partners, academics and social services and housing experts with support from provincial ministries to find innovative housing solutions. In addition to developing a framework for capacity-building projects and recommending funding of demonstration projects, the task force will create online resources to help individuals and families access information, network, collaborate and support each other in exploring and creating successful housing solutions.
391 The challenge with many of the crisis cases our investigation considered was that the individuals were hard to place. It wasn’t simply a question of finding a vacancy; it was a matter of finding a fit. Adults with high behavioural or medical needs were repeatedly rejected for residential placements. In her December 2014 Annual Report, the Auditor General also observed that people with the highest priority needs are not usually placed first. She noted that in one region, 33% of those placed in residences during 2013-2014 had a prioritization score below the average of others on the regional waitlist. In another, 18% of those who were placed had scores below the average on the waitlist.
392 The Ministry has traditionally adopted a detached role when it comes to the administration of developmental services. While it has a broad public policy development function, and is involved in funding supports and services, the Ministry is not intimately involved in the design and development of specific community services and supports. Service agencies are free to create their own programs and residential placements, reflecting their visions of the services they wish to provide. They also have control over who will fill any vacancies. This has resulted in a service gap for a core group of individuals who are traditionally difficult to place because of their extreme behavioural or medical needs.
393 Given the current process, agencies cannot necessarily be blamed. As one Developmental Services Ontario director observed to us, agencies often have limited resource flexibility to take on the risk of accepting someone with extraordinary requirements. Most service agencies are simply not equipped to address individuals who are violent and may present a risk of harm to other residents and staff, or who require specialized medical care. Some officials within this sector suggested to us that more specialized services are required to support these individuals. This makes sense. The Ministry should engage in research and consultation across the developmental services and health sectors with a view to developing residential resources that meet the exceptional needs of individuals whose extreme behaviourial challenges or medical complications present placement challenges. It is not enough to rely on disparate communities and diverse agencies to come up with solutions, and it is inhumane to place this responsibility on desperate families. The Ministry must take the initiative and the lead to create an inventory of placements suitable to these populations. The alternative is to perpetuate a system in which adults with developmental disabilities are underserved and all too often housed in hospitals, long-term care homes and even in jails.
Recommendation 54
The Ministry of Community and Social Services should conduct research and consultation aimed at developing an inventory of residential placements for adults with developmental disabilities whose extreme behavioural or medical needs are not currently adequately accommodated.
Vacancy notice
394 Service agencies are required to notify Developmental Services Ontario offices when they have residential vacancies. However, as the Auditor General observed in her December 2014 Annual Report, the Ministry did not have a policy on how soon service agencies must notify of vacancies. As a result, regional practices varied. For instance, some require immediate notification; others within five days. In some cases we reviewed, it actually took months for service agencies to notify the local Developmental Services Ontario office of vacancies. Officials also told us that permanent vacancies in residences where others were living could not be used as respite spaces on a temporary basis, pending permanent placement. This means that these spaces remain unused when they could be employed to address temporary crisis needs.
395 As part of its upgrades to DSCIS, the Ministry will be introducing measures to reduce the inconsistencies in vacancy reporting practices across the province. However, these do not include reference to standardizing the time frame in which vacancies should be reported. During our investigation, the Ministry told us it had conducted consultation and would be working on a standardized time frame.
396 The Ministry should ensure that there are uniform time requirements for notifying Developmental Services Ontario offices of vacancies and that measures are in place to ensure they are met. The Ministry told us in July 2016 that it released “Developmental Services Residential Resource Management: Interim Instructions” in May, requiring that vacancies be reported within two business days. The instructions include a flow chart of the residential resource management process, which refers to a target of two business days for service agencies to notify Developmental Services Ontario of a permanent vacancy. However, there is no further reference to or any discussion in the Instructions about a requirement that notifications of vacancies occur within two business days. The Ministry should take steps through clear direction and monitoring to ensure consistent and timely notification of residential vacancies. The Ministry should also review the practices preventing temporary use of permanent vacancies and encourage use of these placements to meet urgent residential needs.
Recommendation 55
The Ministry of Community and Social Services should ensure that there are consistent time requirements for notifying Developmental Services Ontario offices of residential vacancies.
Recommendation 56
The Ministry of Community and Social Services should review regional practices for using unfilled permanent residential vacancies with a view to encouraging temporary use of such vacancies for urgent cases.
Inconsistent Case Management and Supports
397 Case management is a critical function in the developmental services sector. Case managers can advocate for adults with developmental disabilities, connect them and their families to necessary resources and provide invaluable assistance in navigating the system. While case management services are available in most regions, many of the individuals we encountered were unable to access them. Sometimes other concerned professionals have stepped in to fill the void. We have seen cases where hospital social workers and even police officers have attempted to navigate the developmental services system on behalf of vulnerable adults. My Office has also assisted, providing referrals and engaging Ministry officials.
398 There is a significant demand for residential services, but many families told us that ideally they would prefer to care for their loved ones at home, as they believed it was the best environment for them. Their crisis points emerged not because of sudden and unexpected changes, but as a result of prolonged difficulty in accessing adequate respite and other supports. Many family members and service providers indicated that respite services can act as a safety valve and help reduce the likelihood of families descending into crisis because of caregiver burnout. One case manager noted that in about 70% of her files, parents had major health concerns like cancer and heart conditions, and needed some relief from the demands of caring for their adult children.
399 Case management services can provide vital assistance to those trying to cope with impending crisis. For instance, in the Eastern Region there are several case management agencies available to deal with urgent situations. However, the availability of case managers differs across the province. The problem is particularly acute in the Southwestern Region, where case management services are unavailable in most areas. Sara’s case is an illustration of what can happen when no one knowledgeable about system resources is there to help.
Crisis management: Sara’s story (West Region)
400 Sara, 22, lives with a developmental disability, epilepsy, metabolic syndrome, cerebral palsy, and anxiety and post- traumatic stress disorders. When we first learned about Sara, she was living at home with her mother, stepfather, and twin six-year-old half-sisters.
401 Like many others in her situation, Sara’s behaviour deteriorated significantly once she hit 18 years of age. She began to throw tantrums in which she would scream, yell and break things. Unfortunately, around this time her family also lost the help of the family support worker who had connected them with services in the children’s developmental support system. As an adult, Sara received some funding, but it was insufficient to pay for more than her living expenses and eight hours of in-home support twice a week.
402 Sara’s mother first contacted the local Developmental Services Ontario office in fall 2011, shortly after Sara turned 18. She was desperate for help with Sara’s escalating conduct, but she claims that officials told her at the time that the “DSO is not a crisis service.” By January 2013, the family was struggling to cope and Sara was threatening self-harm. In February, the situation declined further. Sara’s stepfather had an emotional collapse and her behaviour began to spike.
403 An infusion of temporary funding helped for a while and allowed the family to obtain 32 hours of additional support in the home and some respite services. Unfortunately, Sara’s mother misunderstood the nature of the funding. She thought it would continue indefinitely, and by the time she realized her mistake, she was running out of cash to pay for the level of support Sara required.
404 While Sara’s mother worried about her care and the health and safety of her young daughters, who were exposed to Sara’s tantrums, Sara’s name remained on various waiting lists for supports and mental health and behavioural consultations. In May, Sara was involuntarily admitted to hospital, as a result of her deteriorating situation. That same month, her mother underwent a series of surgeries. Back home in late May, Sara’s behaviour continued to present challenges as she engaged in aggressive episodes and screaming fits, including in front of her young twin sisters.
405 By the end of June, funding to pay for support workers in the home had again run out, and another request was made for emergency flex funding to pay for support workers through to the end of August. By this point, Sara’s family had grown increasingly concerned for the safety of the twins, and frantic to locate a residential placement for Sara in the community. However, there were no suitable vacancies in the area.
406 One local agency told our Office it had two vacancies in May 2013, but neither was appropriate for Sara. One was in a home for individuals with high physical and developmental needs. The other was in an apartment with an older male. The agency attempted to move around residents to make room for Sara, but no one agreed to switch placements, and the vacancies remained empty for months.
407 By fall 2013, Sara’s mother was stretched to the limit. Once again, emergency funds had run out and she was building up her credit card debts to fund a support worker for Sara on a part-time basis. Predictably, Sara’s problem behaviours had increased as her supports decreased. Finally, in November 2013, Sara was approved for $30,000 in annualized Passport funding. She was able to receive behavioural consultation services and continue with her schooling for a while. Unfortunately, while this support provided some funding stability, Sara’s family continued to struggle and was once more plunged into crisis when she suffered a seizure, which resulted in hallucinations as well as violent and aggressive behaviour. After a brief period of hospitalization, she was discharged home, but later entered an in-patient treatment program. She remains in treatment outside of the home.
408 In May 2015, the Ministry began a pilot project in four communities, involving the provision of specialized case management services to those with complex and urgent needs, including individuals at risk of harm to themselves or others. The case managers work in collaboration with local urgent response committees, and their responsibilities include helping individuals and their families connect with relevant service providers in multiple sectors, including the local community, health, justice and social services systems. The case managers are supervised and employed by a lead agency. The Ministry will be reviewing the results of the pilot project at the end of July 2016.
409 In Sara’s case, her family’s frustration and stress was exacerbated by the lack of understanding of the difference between permanent and temporary funding and the sporadic nature of financial relief available through the developmental sector. Having a case manager assigned to help navigate the system might well have provided some relief and assisted in obtaining resources sooner. While the recent initiative towards providing urgent case management services is a positive step, the Ministry should ensure that individuals generally have greater access to case management services, which may assist in deflecting crisis situations.
Recommendation 57
The Ministry of Community and Social Services should take steps to ensure that adults with developmental disabilities have access to case management services throughout Ontario.
Parents helping parents
410 Parents and other caregivers who have successfully navigated the system are often the most adept at providing practical guidance to others facing similar circumstances. The Ministry should consult system stakeholders with a view to developing an easily accessible online network to help caregivers learn from the experience of others.
Recommendation 58
The Ministry of Community and Social Services should consult relevant ministries and stakeholder groups with a view to developing an online resource to help caregivers connect and share their knowledge and experiences.
“We are NOT case managers”
411 In the fall of 2012, when this investigation began, our Office’s requests for information relating to specific individuals were repeatedly met with the refrain that Ministry officials were not case managers, but system managers focused on “the big picture.” Regularly, our efforts to obtain details about individual cases were met with resistance and the suggestion that we were interfering in the natural system order. On occasion, we were accused of helping individuals jump the queue for services.
412 As Ombudsman, I cannot ignore individual complaints or my duty to attempt to resolve them, but I am also acutely aware that discrete complaints are often harbingers of systemic malfunction. One of the reasons my Office commenced this investigation was to try to tackle the root causes leading to crisis in the developmental services sector and arrive at recommendations for improvements that will benefit all within it.Had the system been operating effectively, there would have been little need for our staff to intervene to help individuals in crisis.
413 By fall 2013, with the arrival of a new Assistant Deputy Minister, there was a palpable shift in the Ministry’s organizational culture. Senior Ministry officials began to work directly with us to resolve individual cases and proactively seek changes in policies and practices to benefit others. There has been a marked improvement in response to crisis and a recognition that the Ministry plays a vital role in resolving complex cases. In order to ensure that this momentum continues, the Ministry should formally recognize that it has a role in facilitating resolution of individual crisis situations.
Recommendation 59
The Ministry of Community and Social Services should formally recognize that it has an important role to play in facilitating the resolution of individual crisis cases.
Opinion
414 I recognize that ensuring adequate supports and services for adults with developmental disabilities has proven a challenge for successive governments. History has evidenced some dismal failures in serving this remarkably diverse and uniquely vulnerable population. Today, many adults with developmental disabilities and their careworn families remain voiceless, frustrated and confused by a developmental services system that is overwhelmed and unable to satisfy the sheer demand for services and supports.
415 In recent years, the Ministry has emphasized that developmental services have evolved beyond the days of isolation and institutionalization. The sector now promotes social inclusion, individual choice and independence. This reflects a positive system change. However, it is still an unfortunate reality that chronic gaps in supports and services have left many individuals living on the margins of society without viable options, and dependent on a system that continues to be unresponsive to their urgent circumstances.
416 My investigation focused on extreme and egregious cases that highlight a dire need for greater supports, services and more rigorous system monitoring. We heard about 23 individuals abused and neglected in their own homes and the scarcity of safe beds and crisis supports available to address these circumstances. We also discovered that an unintended and modern-day version of institutionalization persists, but in different forms.
417 The violent, impulsive and destructive behaviour of some individuals with developmental disabilities can besiege their caregivers. Without sufficient specialized community supports and services, many resort to hospitals or the police for help. We found that in 79 cases, otherwise healthy adults with developmental disabilities were hospitalized unnecessarily for prolonged periods. Many languished without access to trained staff, developmental programs or services and were subject to chemical and physical restraint. In another 14 cases, young adults with developmental disabilities were isolated from their peers, underserviced, and shunted off to live with the elderly in long-term care homes. Shockingly, we also learned of 46 individuals who were caught up and incarcerated within the criminal justice system, many as a result of limited community housing and supports.
418 Then there were 148 individuals and their families struggling with medically complex situations. Exhausted caregivers who were frantic to acquire services were left dependent on inter-ministerial co-ordination and specialized care and supports that too often simply did not materialize.
419 We also found that deficient transitional planning and services to support individuals through the life cycle have contributed to family collapse. We heard about 30 individuals who were abandoned by their beleaguered families, and another 122 whose caregivers were aged, sick or had recently died, leaving them facing homelessness.
420 The stories of hopelessness and despair canvassed in this report are compelling, tragic and, regrettably, just the tip of the iceberg. In addition to the 1,436 citizens who managed to make their way to my Office to complain, there are many thousands more in urgent circumstances and anxious for relief. Decades of inconsistent and incomplete record keeping have left even the Ministry ignorant of the full scope of the problem.
421 Our Office continues to receive requests for help from those in crisis. The Ministry can no longer deflect responsibility by referring to the fact that developmental services are discretionary, that families and communities bear primary accountability for providing care, and that the Ministry is only a detached system manager. Findings of the Select Committee on Developmental Services, the Auditor General and coroner’s inquests have all reinforced the need for a fundamental change in direction in planning for and administering the developmental services sector. The Ministry must make a genuine and concerted effort towards large-scale systemic renovation.
422 Since this investigation began in November 2012, the government has committed significant additional funding to the developmental services sector. The Ministry of Community and Social Services has made improvements in how it addresses situations of crisis involving adults with developmental disabilities, and in how it administers the process for urgent access to services. There has also been a marked attitudinal shift within the Ministry. Officials are no longer aloof and preoccupied with the bigger system picture. They are more willing to acknowledge system gaps and engage directly in resolution of individual crisis cases. These are all indicators of positive systemic change. However, the developmental services sector has deep and tangled historical roots, and the challenges facing individuals in crisis are far from solved. Transformation of the system has been slow and incremental.
423 Today, the processes for responding to crisis situations continue to be marred by complexity and fragmentation. Prioritization, matching and urgent response practices are inconsistent and unco-ordinated across the province. There are insufficient system safeguards to address cases of abandonment and homelessness, abuse, medical fragility, and institutionalization through unnecessary and inappropriate hospitalization, criminalization and incarceration, and unsuitable placements in long-term care homes. Negligible progress has also been made in inter-ministerial collaboration to resolve the needs of those in crisis. In addition, more research is required to effectively plan for services, and more education and outreach is necessary to facilitate access to supports and protect individuals with developmental disabilities and their families.
424 Accordingly, it is my opinion that the Ministry of Community and Social Services’ response to crisis and urgent situations involving adults with developmental disabilities – and its overall administration of developmental services sector programs in these circumstances – have been unreasonable and wrong under the Ombudsman Act.
425 I am committed to actively monitoring the Ministry’s efforts to address my concerns and to ensuring that concrete reparative action is taken.
Recommendation 60
The Ministry of Community and Social Services should report back to my Office in six months’ time on the progress in implementing my recommendations, and at six-month intervals thereafter until such time as I am satisfied that adequate steps have been taken to address them.
Recommendations
Given the results of this investigation, I am making the following recommendations:
Abuse and urgent access to residential resources
Recommendation 1
The Ministry of Community and Social Services should regularly monitor and audit agencies serving adults with developmental disabilities to ensure they are meeting their regulatory responsibilities to report abuse to police.
Recommendation 2
The Ministry of Community and Social Services should engage in education and outreach efforts with agencies serving adults with developmental disabilities concerning their legal obligation to report incidents of abuse to police, and include examples such as Adam’s story to emphasize the importance of early reporting.
Recommendation 3
The Ministry of Community and Social Services should direct Developmental Services Ontario offices, as well as service agencies responsible for placing and/or housing adults with developmental disabilities, that victims of abuse should be placed in safe and secure housing and not returned to the care of their abusers.
Recommendation 4
The Ministry of Community and Social Services should regularly gather statistical information from agencies, as well as police services across Ontario, to identify the number of situations in which adults with developmental disabilities have been the victims of abuse by caregivers.
Recommendation 5
The Ministry of Community and Social Services should make specific resources available to be used in urgent situations to provide safe housing and services where an adult with developmental disabilities is the victim of abuse and requires removal from their home for their protection.
Recommendation 6
The Ministry of Community and Social Services should consult with the Ministry of Community Safety and Correctional Services, as well as police services throughout the province, to promote the establishment of specialty police units able to address situations involving abuse of adults with developmental disabilities.
Recommendation 7
The Ministry of Community and Social Services should regularly collect statistical information about the use of community shelters by adults with developmental disabilities, which can be used for planning for crisis supports and services.
Recommendation 8
The Ministry of Community and Social Services should ensure that there are adequate crisis beds throughout the province to serve the urgent needs of adults with developmental disabilities.
Recommendation 9
The Ministry of Community and Social Services should create an online provincial inventory of crisis beds easily accessible to developmental services and police officials.
Recommendation 10
The Ministry of Community and Social Services should provide direction to service agencies that homeless shelters and similar temporary options are unsuitable for those with developmental disabilities and dual diagnosis.
Recommendation 11
The Ministry of Community and Social Services should develop an urgent response mechanism that is available and accessible province-wide on a 24-hour, seven-day-a-week basis.
Recommendation 12
The Ministry of Community and Social Services should ensure that crisis workers are available to assist adults with developmental disabilities who require urgent assistance to access temporary residential placements.
Recommendation 13
The Ministry of Community and Social Services should develop an expanded reporting system so that service agencies, Developmental Services Ontario offices, police or other officials can identify situations where there is potential for an abuse to develop, if adequate developmental services and supports are not provided on an urgent basis.
Recommendation 14
The Ministry of Community and Social Services should expand the definition of urgent circumstances in the Urgent Response Guidelines to address situations where a risk of abuse has been identified.
Inappropriate hospitalization
Recommendation 15
The Ministry of Community and Social Services should obtain regular information from hospitals across the province concerning emergency visits and admissions of adults with developmental disabilities, including details about hospital stays, their length, and their outcomes, in order to plan for appropriate developmental supports and services.
Recommendation 16
The Ministry of Community and Social Services should send a direct message to Developmental Services Ontario and community service agencies that adults with developmental disabilities should not be left in hospitals where there is no medical need.
Recommendation 17
The Ministry of Community and Social Services should require service agencies, Developmental Services Ontario offices and hospitals to provide regular reports about adults with developmental disabilities who are hospitalized but no longer require hospital care, and maintain an active record of such cases.
Recommendation 18
The Ministry of Community and Social Services and Developmental Services Ontario offices should ensure that individuals identified on its record of alternative level of care hospital patients are prioritized as urgent for community placements.
Recommendation 19
The Ministry of Community and Social Services should report publicly on a regular basis about the work of the various inter-ministerial committees relating to developmental services and the health care system, as well as on the status of initiatives under discussion.
Inappropriate admission to long-term care homes
Recommendation 20
The Ministry of Community and Social Services should take steps to ensure that it is notified when it is proposed that an adult with a developmental disability be placed in a long-term care home.
Recommendation 21
The Ministry of Community and Social Services should actively work with local agencies to ensure that placement of young adults with developmental disabilities in long-term care homes is considered a last resort and that alternative solutions are vigorously pursued.
Recommendation 22
The Ministry of Community and Social Services should engage in ongoing research on how many adults with developmental disabilities are housed within the long-term care system and compile statistics, including age and nature of condition, for use in system planning.
Recommendation 23
The Ministry of Community and Social Services should launch an immediate review of all placements of individuals with developmental disabilities in the long-term care sector, and ensure that any individuals who have been inappropriately placed are appropriately prioritized for transitioning to the developmental services sector.
Recommendation 24
The Ministry of Community and Social Services should review all placements of individuals with developmental disabilities in the long-term care sector on an ongoing basis to ensure that such placements meet individual needs.
Recommendation 25
The Ministry of Community and Social Services should enter into a protocol with the Ministry of Health and Long-Term Care to ensure that it is notified and provided with relevant information about complaints and investigations relating to serious occurrences involving adults with developmental disabilities within the long-term care system.
Recommendation 26
The Ministry of Community and Social Services should educate Developmental Services Ontario officials and other stakeholders about options for placements within the long-term care sector to encourage greater cross-sector collaboration and the potential for placements to be exchanged to accommodate the needs of adults with developmental disabilities.
Criminalization and incarceration
Recommendation 27
The Ministry of Community and Social Services should ensure that there are specialized case management and court support services available for all individuals with developmental disabilities involved with the criminal justice and correctional system.
Recommendation 28
The Ministry of Community and Social Services should create positions or retain service providers to be responsible for co-ordinating an urgent response in cases where adults with developmental disabilities are or are at risk of being charged with criminal offences, arrested and/or incarcerated, including liaising with families and relevant officials and securing supportive resources and services, such as residential placements.
Recommendation 29
The Ministry of Community and Social Services should undertake research and conduct consultation with subject specialists concerning the creation of specialized court diversion programs addressed specifically to the needs of adults with developmental disabilities.
Recommendation 30
The Ministry of Community and Social Services should work with the Ministry of the Attorney General and the Ministry of Community Safety and Correctional Services to support specialized diversion programs for individuals with developmental disabilities who are charged with criminal offences.
Recommendation 31
The Ministry of Community and Social Services should take the lead and work with other ministry partners to develop a responsive and proactive system of residential supports to divert adults with developmental disabilities away from the criminal justice and correctional systems.
Recommendation 32
The Ministry of Community and Social Services should ensure that senior officials take a proactive and robust approach to inter-ministerial initiatives aimed at reducing potential for the criminalization of individuals with developmental disabilities and dual diagnosis.
Recommendation 33
The Ministry of Community and Social Services should publicly post progress updates on initiatives and collaborative efforts relating to diverting adults with developmental disabilities from – and protecting them within – the justice system.
Recommendation 34
The Ministry of Community and Social Services should engage in targeted outreach and education of officials in the justice and correctional systems to improve understanding of the nature of developmental disabilities and the developmental services system, and to encourage implementation of best practices for responding to individuals with developmental disabilities, based on the advice of subject experts.
Recommendation 35
The Ministry of Community and Social Services should work with the Ministry of Children and Youth Services to ensure that it provides detailed case information about youths with developmental disabilities and dual diagnosis transitioning to the adult system, who have been involved with the youth justice system.
Recommendation 36
The Ministry of Community and Social Services should gather statistical information on the number of adults with developmental disabilities who enter the criminal justice and correctional systems, to help with planning to ensure there are adequate resources including supervised residential placements within the community as an alternative to incarceration.
Recommendation 37
The Ministry of Community and Social Services should consult with service providers, community groups and other relevant ministries – such as the Ministries of the Attorney General, Children and Youth Services, Community Safety and Correctional Services, Education, and Health and Long-Term Care – with a view to developing a co-ordinated system for gathering statistical and qualitative information to identify the number of individuals and types of situations that may require exceptional supports to minimize the risk of individuals who require developmental services defaulting to the criminal justice system.
Recommendation 38
The Ministry of Community and Social Services should work with the Ministries of the Attorney General and Community Safety and Correctional Services to develop an effective process for sharing information and facilitating resolutions of cases involving adults with developmental disabilities within the criminal justice and correctional systems.
Recommendation 39
The Ministry of Community and Social Services should work with other relevant ministries on a process for identifying and providing preventative supports for individuals at risk of becoming involved in the criminal justice system.
Recommendation 40
The Ministry of Community and Social Services should consult relevant stakeholders with a view to encouraging Developmental Services Ontario offices, service agencies and police services to work together to develop a provincewide vulnerable person registry to assist police and justice officials in responding to crisis involving adults with developmental disabilities.
Recommendation 41
The Ministry of Community and Social Services should continue to support the development, based on best practices, of guidelines and protocols for responding to physical aggression by adults with developmental disabilities, balancing the need to protect clients and staff with the goal of avoiding criminalization of those with developmental disabilities.
Recommendation 42
The Ministry of Community and Social Services should engage in consultation and outreach with justice officials, including police services, correctional officials, Crown prosecutors and the judiciary, relating to best practices for addressing the needs of individuals with challenging behaviours.
Medically complex cases
Recommendation 43
The Ministry of Community and Social Services should engage the Ministry of Health and Long-Term Care in the multi-ministry planning process in medically complex cases to ensure appropriate specialized medical and community resources are available as they transition into the adult system.
Recommendation 44
The Ministry of Community and Social Services should ensure that Developmental Services Ontario offices actively pursue opportunities for sharing of resources across geographical boundaries to ensure that the urgent needs of individuals in underserviced areas are adequately met.
Abandonment and homelessness
Recommendation 45
The Ministry of Community and Social Services should analyze cases of abandonment to identify root causes and develop ameliorative measures to reduce the risk of abandonment in future.
Recommendation 46
The Ministry of Community and Social Services should add a requirement to its occurrence reporting system so that cases in which there is a substantial risk of abandonment or homelessness are reported to the Ministry and appropriately addressed.
Recommendation 47
The Ministry of Community and Social Services should ensure that sufficient resources are available to address situations or significant risks of abandonment or homelessness.
Recommendation 48
The Ministry of Community and Social Services should provide clear direction to its regional offices and Developmental Services Ontario officials about co-ordinating services to meet the needs of clients who reside in and/or receive services from more than one jurisdiction.
Recommendation 49
The Ministry of Community and Social Services should work closely with the Ministry of Children and Youth Services, Ministry of Education, Ministry of Health and Long-Term Care, Developmental Services Ontario offices and service agencies to track individual cases and crisis events in the developmental services sector.
Recommendation 50
The Ministry of Community and Social Services should engage subject experts to advise on the likelihood and rate of life crises in the developmental services sector and use these projections in system planning.
Recommendation 51
The Ministry of Community and Social Services should direct Developmental Services Ontario, service co-ordination offices and agencies providing developmental services to adopt record-keeping practices requiring that contacts with families, the Ministry and other agencies be properly documented.
Vacancy management
Recommendation 52
The Ministry of Community and Social Services should provide direction to Developmental Services Ontario offices to ensure that individuals are matched to vacancies only where there is a realistic prospect of an appropriate fit.
Recommendation 53
The Ministry of Community and Social Services should ensure that service agencies provide detailed explanations for rejecting applicants for residential vacancies who are in crisis situations and/or have complex needs.
Recommendation 54
The Ministry of Community and Social Services should conduct research and consultation aimed at developing an inventory of residential placements for adults with developmental disabilities whose extreme behavioural or medical needs are not currently adequately accommodated.
Recommendation 55
The Ministry of Community and Social Services should ensure that there are consistent time requirements for notifying Developmental Services Ontario offices of residential vacancies.
Recommendation 56
The Ministry of Community and Social Services should review regional practices for using unfilled permanent residential vacancies with a view to encouraging temporary use of such vacancies for urgent cases.
Information and case management resources
Recommendation 57
The Ministry of Community and Social Services should take steps to ensure that adults with developmental disabilities have access to case management services throughout Ontario.
Recommendation 58
The Ministry of Community and Social Services should consult relevant ministries and stakeholder groups with a view to developing an online resource to help caregivers connect and share their knowledge and experiences.
Recommendation 59
The Ministry of Community and Social Services should formally recognize that it has an important role to play in facilitating the resolution of individual crisis cases.
Progress reporting
Recommendation 60
The Ministry of Community and Social Services should report back to my Office in six months’ time on the progress in implementing my recommendations, and at six-month intervals thereafter until such time as I am satisfied that adequate steps have been taken to address them.
Response
426 The Ministry of Community and Social Services was provided with an opportunity to review and respond to my preliminary findings, opinion, and recommendations. The Ministry’s comments were taken into consideration in the preparation of this final report.
427 In a meeting I had with the Minister and Deputy Minister, the Minister agreed with all of my recommendations. The Deputy Minister also provided a detailed response, outlining the steps that the Ministry is undertaking to address my recommendations. A copy of this response is appended to this report.
428 In her response, the Deputy Minister referenced the efforts that have been made to transform the developmental services sector to embrace a person-centred approach, reflecting the importance of individual choice. However, she acknowledged that some unacceptable situations, as identified in this report, still exist. She fully committed to working with my Office, individuals, families, and the sector to improve outcomes for those with developmental disabilities.
429 I am encouraged by the steps the Ministry has already taken over the course of my investigation to address system gaps, and by its positive response to my report. I will carefully monitor the Ministry’s progress in implementing my recommendations.
____________________
Paul Dubé
Ombudsman of Ontario
Appendix
This link opens in a new tabResponse from Ministry of Community and Social Services (accessible PDF)
[1] Ontario Ministry of Community and Social Services, “This link opens in a new tabApology by Premier Kathleen Wynne: Ontario’s apology to former residents of regional centres for people with developmental disabilities,” December 9, 2013. The apology concerned abuses that occurred at the Huronia Regional Centre between 1945 and 2009, and was extended to residents there and others “who were failed by a model of institutional care.”
[2] Names have been altered to protect personal privacy.
[3] Auditor General of Ontario, 2014 Annual Report, Chapter 3, Section 3.10: “This link opens in a new tabMinistry of Community and Social Services, Residential Services for People with Developmental Disabilities.”
[4] Legislative Assembly of Ontario, Select Committee on Developmental Services, This link opens in a new tabFinal Report, July 2014: Inclusion and Opportunity: A New Path for Developmental Services of Ontario, at page 11.
[5] Ibid., p. 3.
[6] Ontario Ministry of Finance, This link opens in a new tabBudget 2014: Fostering a Fair Society.
[7] Auditor General of Ontario, supra note 3, pp. 332-381.
[8] This link opens in a new tabHawley (Re), 2015 CanLII 93858 (ON OCCO), retrieved on April 12, 2016.
[9] Joffe, Kerri, This link opens in a new tabEnforcing the Rights of People with Disabilities in Ontario’s Developmental Services System, Law Commission of Ontario/ARCH Disability Law Centre, June 30, 2010, p.13.
[10] Williston, Walter B., This link opens in a new tabA Report for the Minister of Health on Present Arrangements for the Care and Supervision of Mentally Retarded People in Ontario, August 1971.
[11] Ontario Ministry of Community and Social Services, “This link opens in a new tabFrom Institutional to Community Living: A History of Developmental Services”.
[12] Legislative Assembly of Ontario, This link opens in a new tabSelect Committee on Developmental Services, Interim Report, March 2014, at page 4.
[13] Ontario Ministry of Community and Social Services, supra note 11.
[14] Ibid.
[15] Ibid.
[16] Ibid.
[17] Settlements were reached with the province with respect to Huronia in December 2013, and Rideau and Southwestern Regional Centres in February 2014. For information see these Ontario government news releases: This link opens in a new tab(1) and This link opens in a new tab(2). On April 27, 2016, the province also announced that the Superior Court of Justice had approved a $36-million settlement for survivors of 12 other provincially operated institutions for persons with developmental disabilities throughout Ontario. This link opens in a new tabNews release.
[18] This link opens in a new tabHansard, December 9, 2013, online.
[19] Of the nine former regions, Toronto Region remains – the other eight were realigned into four as follows: North Region (formerly North and North East); East Region (formerly East, South East and part of Central East); Central Region (formerly Central West and part of Central East); and West Region (formerly South West and Hamilton-Niagara).
[20] This was the maximum rate as of November 2015.
[21] The Ministry confirmed that the figure of 14,300 on the waitlist cited by the Auditor General in her 2014 Annual Report (supra note 3) was later found to be lower when the Ministry reviewed its data for 2014.
[22] Auditor General of Ontario, supra note 3.
[23] Ibid.
[24] This link opens in a new tabCoroner’s Inquest into the death of Guy Mitchell, verdict received July 24, 2015, available online.
[25] Hawley (Re), supra note 8.
[26] S.8(4), O.Reg 299/10, Regulation on Quality Assurance Measures, under the Services and Supports to Promote the Social Inclusion of Persons with Developmental Disabilities Act, 2008.
[27] Ibid., s. 1(1).
[28] Ibid., s.8.
[29] As of April 26, 2016.
[30] In 1996, the Ministry of Health and Long-Term Care established Community Care Access Centres. There are 14 across Ontario that help people access government-funded home and community services, and long-term care homes.
[31] Yona Lunsky; Elspeth Bradley; Janet Durbin; Chris Koegl; Maaike Canrinus; Paula Goering, “This link opens in a new tabThe Clinical Profile and Service Needs of Hospitalized Adults With Mental Retardation and a Psychiatric Diagnosis,” Psychiatric Services, January 1, 2006: Abstract.
[32] Dale Butterill MSW, MPA; Elizabeth Lin, PhD; Janet Durbin, PhD; Yona Lunsky, PhD; Karen Urbanoski, PhD (Candidate); and Heather Soberman, MA: This link opens in a new tabFrom Hospital to Home: The Transitioning of Alternate Level of Care and Long-stay Mental Health Clients, Centre for Addiction and Mental Health, September 2009.
[33] Ibid., p. 46.
[34] Lunsky Y, Lin E, Balogh R, Klein-Geltink J, Bennie J, Wilton A, Kurdyak P: “This link opens in a new tabAre adults with developmental disabilities more likely to visit EDs?” American Journal of Emergency Medicine, 2011. 29(4), 463-465. Abstract.
[35] Lunsky Y, Elserafi J.: “Life events and emergency department visits in response to crisis in individuals with intellectual disabilities.” Journal of Intellectual Disability Research, 55(7), 714-718.
[36] Provincial Review of Dual Diagnosis Programs: Final Report, October 5, 2012, KPMG.
[37] Office of the Correctional Investigator of Canada: “This link opens in a new tabSpeaking Notes for Mr. Howard Sapers, Correctional Investigator of Canada, Appearance before the Standing Committee on Public Safety and National Security”, June 2, 2009, 9:00-11:00, online.
[38] Office of the Ombudsman of Ontario, This link opens in a new tab“This link opens in a new tabSegregation: Not an Isolated Problem”: Submission in response to the Ministry of Community Safety and Correctional Services’ consultation on its review of policies related to segregation of inmates, Paul Dubé, May 9, 2016.
[39] Southern Network of Specialized Care, This link opens in a new tabUnderstanding Special Needs Offenders Who Have a Dual Diagnosis, June 2013. Available online.
[40] The Ministry originally planned for this initiative to be completed March 31, 2015.
[41] Poonam Raina, Tamara Arenovich, Jessica Jones and Yona Lunsky, “This link opens in a new tabPathways into the criminal justice system for individuals with intellectual disability,” Journal of Applied Research in Intellectual Disabilities, vol. 26 (2013): 404-409. Abstract online.
[42] Community Networks of Specialized Care, A Proposal to Develop, Facilitate Implementation and Monitor Province-wide Standards of Care and Treatment of Persons with a Dual Diagnosis and/or Challenging Behaviours, June 27, 2013, at page 1.
[43] “This link opens in a new tabCancer claims Cindy Gibson, mother who sought care for disabled daughter,” Ottawa Citizen, May 20, 2014.